Gériatrie et Psychologie Neuropsychiatrie du Vieillissement
MENUInterest of ambulatory management of patients with chronic heart failure by protocolized follow-up and therapeutic education: results of the USICAR experiment Volume 19, issue 1, Mars 2021
- Key words: heart failure, protocolized follow-up, therapeutic education, care pathway, coordination unit, personalized medicine, telemedicine
- DOI : 10.1684/pnv.2021.0917
- Page(s) : 42-52
- Published in: 2021
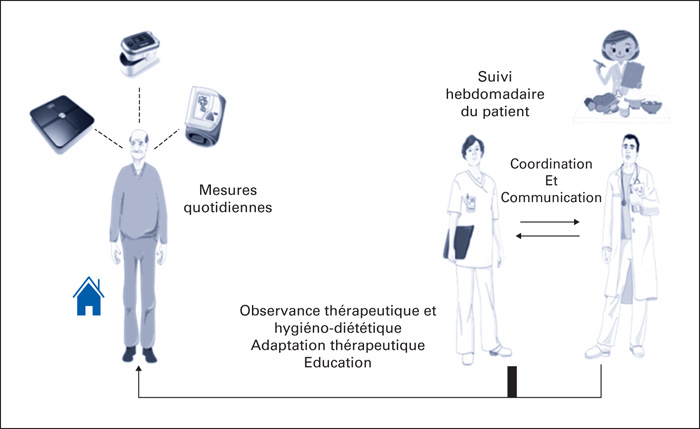
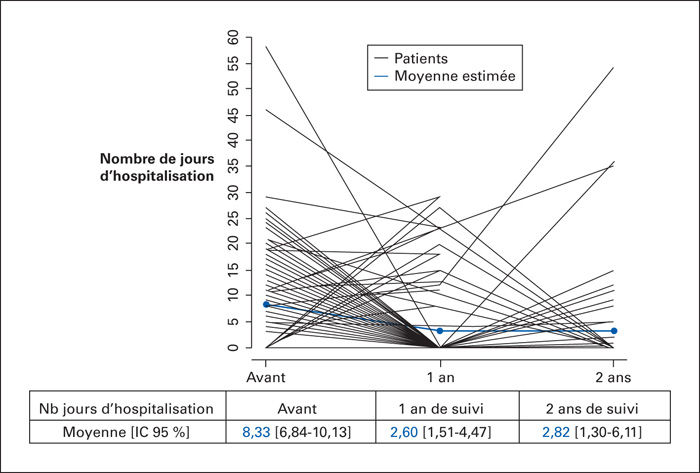
Objective: The objective of this study is to determine whether the implementation of regular and structured follow-up of patients with chronic heart failure (CHF), combined with therapeutic education, led to better management of these patients. Patients and Method: This was a monocentric, retrospective study on a cohort of patients with a proven CHF, followed in the Mulhouse region (France), between January 2016 and December 2017, by the Unit for Monitoring Heart Failure Patients (USICAR). These patients benefited from a regular protocolized follow-up and a therapeutic education program for a period of 2 years. The main criterion of this study was: the number of days of hospitalization for HF per year and per patient. The secondary endpoints were: the number of days of hospitalization for cardiac causes other than HF and the number of hospital stays for HF per patient. These criteria were collected over the one-year period before inclusion, at one-year-follow-up, and at two-years-follow-up. Results: 159 patients with a mean age of 72.9 years were included in this study. They all had a CHF, mainly stage I-II NYHA (88.7%), of predominantly ischemic origin (50.9%), with altered left ventricular ejection fraction in 69.2% of cases. The primary endpoint averaged 8.33 days (6.84-10.13) in the year prior to inclusion, 2.6 days (1.51-4.47) in the first year of follow-up, and 2.82 days (1.30-6.11) (p <0.01 for both comparisons). The mean number of days of hospitalization for other cardiac causes other than HF to patient numbers was: 1.73 days (1.16-2.6), 1.81 days (1.04-3.16), and 1.32 days (0.57-3.08) (p = ns). The percentage of hospitalization for HF for each patient was: 69.5% (60.2-77.4) before inclusion, 16.2% (10-25.2) during the first year of follow-up and 19.3% (11-31.8) during the second (p < 0.001 for both comparisons). Conclusion: This study demonstrates the value of a protocolized follow-up associated with a therapeutic education program to improve the management of ambulatory CHF patients, particularly for moderate CHF.