Virologie
MENUViral reactivations in intensive care unit: biomarkers of immune dysfunction or true pathogens? Volume 25, issue 3, Mai-Juin 2021
- Key words: ICU patients, viral reactivations, HSV, CMV, virome
- DOI : 10.1684/vir.2021.0905
- Page(s) : 168-82
- Published in: 2021
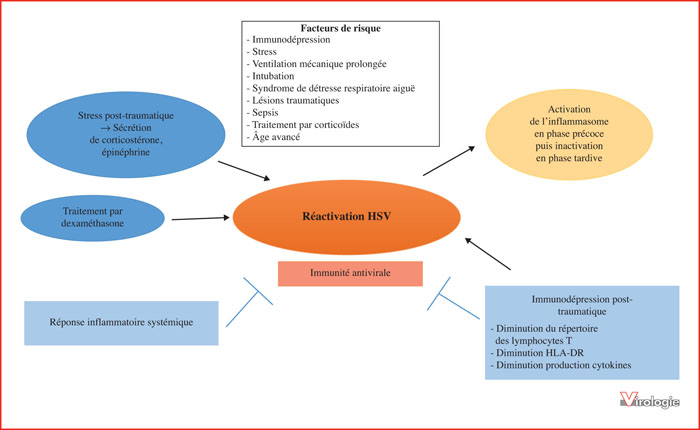
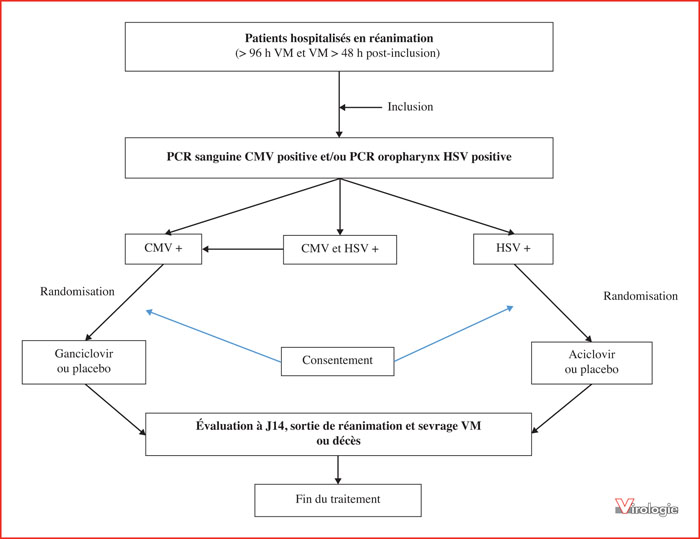
Studies performed in patients considered as immunocompetent and hospitalized in intensive care unit (ICU) have revealed profound immune alterations leading to an increased risk of viral reactivations. In particular, Herpesviridae reactivations (HSV and CMV) have been associated with an increased morbidity and mortality in ICU patients. Early diagnosis of these reactivations is now recommended in ICU patients, but the indications of an antiviral therapy remain to be better defined. Advances in molecular biology now allow us to study the human virome in different biological compartments. Among the more frequent viruses detected in the virome, Torque Teno Virus (TTV) has been shown to be associated to the immunocompetence level of immunocompromised patients at risk of opportunistic viral infections. In organ transplant patients, the TTV proportion in blood increases with the degree of immunosuppression and the risk of secondary infections. It remains to be evaluated in other immune dysfunction settings, such as ICU patients. Human virome modulation, as measured by metagenomics, is a promising tool to investigate immune status in various clinical settings. It could be an innovative marker for personalized care, including the evaluation of immunomodulatory molecules use for the prevention and treatment of infectious complications in ICU patients.