Hépato-Gastro & Oncologie Digestive
MENUUse of growth factors in liver disease Volume 27, issue 3, Mars 2020
- Key words: cirrhosis, alcoholic hepatitis, growth factors
- DOI : 10.1684/hpg.2020.1935
- Page(s) : 278-86
- Published in: 2020
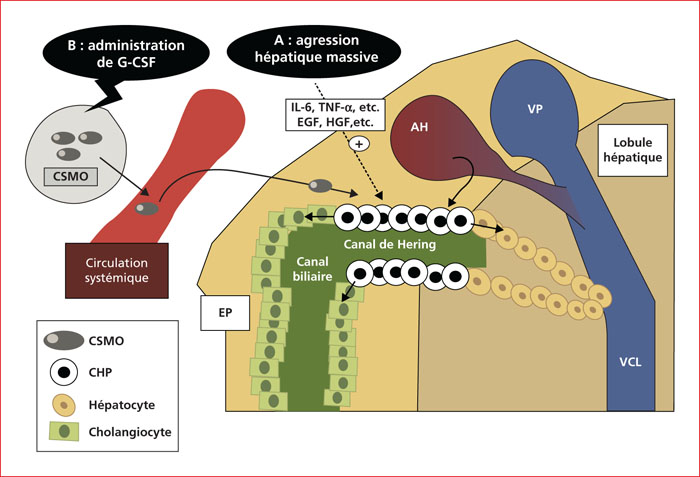
Chronic liver diseases are responsible for a high worldwide morbidity and mortality. Following hepatocellular injury, the remaining mature hepatocytes may proliferate and repair the damaged liver, but this regenerative process is often limited. When hepatocyte proliferation is compromised, hepatic progenitor cells may proliferate and differentiate into hepatocytes. Liver transplantation (LT) represents the only proven definitive treatment for patients with end-stage liver disease but LT is not always possible because of the scarcity of donor organs. Stem cell therapy, which could overcome this pitfall, is based on two strategies: The first one consists on the inoculation of bone marrow-derived stem cells (BMSC) and the second one uses granulocyte colony-stimulating factor (G-CSF) which mobilizes BMSC. G-CSF is currently used in hepatology, as part of therapeutic trials, in three different contexts, namely severe acute alcoholic hepatitis, decompensated cirrhosis and cirrhosis with organ failure. With G-CSF, the results on survival and on liver specific scores in these three indications appear promising. However, these trials are mostly Indian and sample sizes are small; in addition, interim results from a recent German study did not confirm the safety of G-CSF in ACLF patients and survival was not improved. Several studies using G-CSF in hepatology are currently in progress and will be able to confirm (or not) the relevance of G-CSF in severe liver disease.