Hépato-Gastro & Oncologie Digestive
MENUFaecal immunochemical tests: Resembling a Swiss army knife Volume 29, issue 2, February 2022
- Key words: colonoscopy, colorectal neoplasia, faecal immunochemical tests, faeces, occult blood, quality assurance, screening
- DOI : 10.1684/hpg.2022.2324
- Page(s) : 165-80
- Published in: 2022
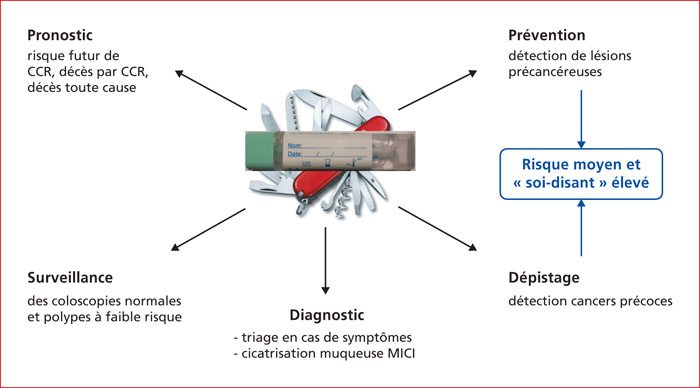
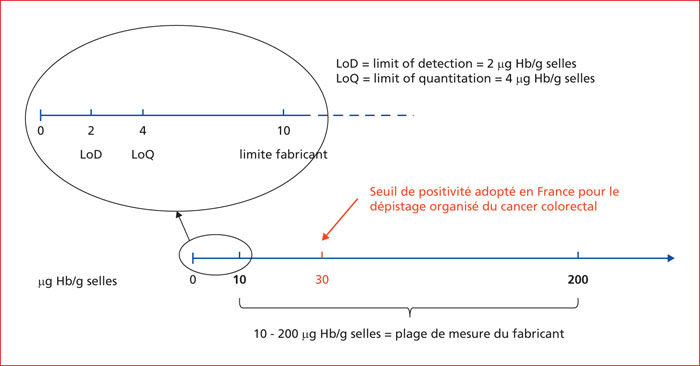
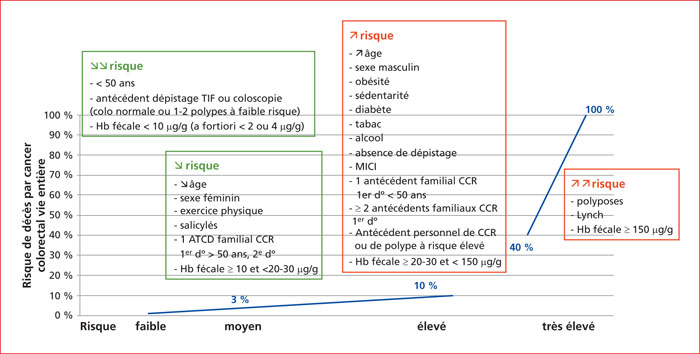
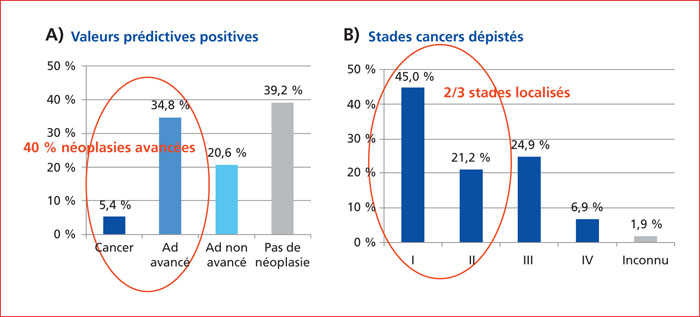
The detection of blood in faeces has often been perceived as an inadequate investigation, probably because of the poor performance of the now considered obsolete guaiac faecal occult blood tests (e.g., Hemoccult). Qualitative faecal immunochemical tests (FIT) performed by medical laboratories have many disadvantages and should also be considered as obsolete and discontinued. In contrast, the performance of quantitative FIT, which generate estimates of faecal haemoglobin concentration, is such that they have become widely considered as the best non-invasive investigation for use in screening programmes for individuals at average risk of colorectal cancer (CRC). In France, quantitative FIT (OC-Sensor FIT at a 30 μg/g threshold for a positive test result) are reserved exclusively for the population-based CRC screening programme. However, uses of FIT in other clinical applications have been evaluated and validated. FIT can be used for CRC screening in individuals allegedly at high risk, namely those with a family history of colorectal neoplasia, and in surveillance of individuals after polypectomy of 1 or 2 low risk polyps. Several neighbouring countries, particularly the United Kingdom and Spain, use FIT in general practice to determine the indication for colonoscopy in patients presenting with lower gastrointestinal symptoms, and to assess the degree of urgency, with decision thresholds different from organised screening programmes: a faecal haemoglobin concentration above 4-10 μg/g should be investigated by colonoscopy, which should be considered as urgent if the concentration is above 150 μg/g. The measurement of faecal haemoglobin has been proposed as an alternative to faecal calprotectin in inflammatory bowel disease affecting the colon in the diagnosis and monitoring of mucosal damage and healing and for the prediction of relapse. Further uses of FIT are still under evaluation and offer interesting perspectives, such as personalised screening according to sex, age and serial faecal haemoglobin concentrations. To make the best use of the good diagnostic performance of quantitative FIT, French recommendations concerning CRC risk evaluation, CRC screening in individuals with a family history, and indications for colonoscopy need to be updated. Similarly, the management, organisation and specifications of the French organised screening programme need to be reviewed. Lowering the positivity threshold from 30 to 20 or even 15 μg/g is proposed.