Hépato-Gastro & Oncologie Digestive
MENUSolitary rectal ulcer syndrom: Break out of isolation… Volume 26, issue 6, Juin 2019
Figures
-
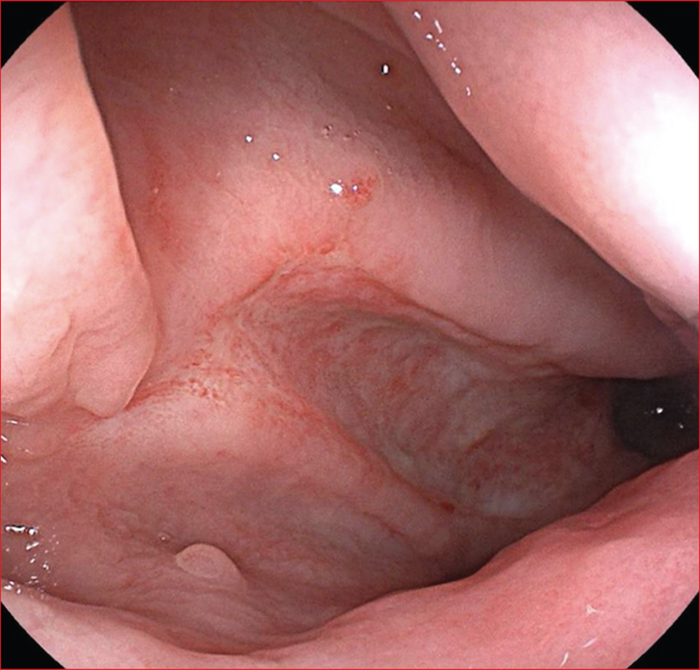
Figure 1 -
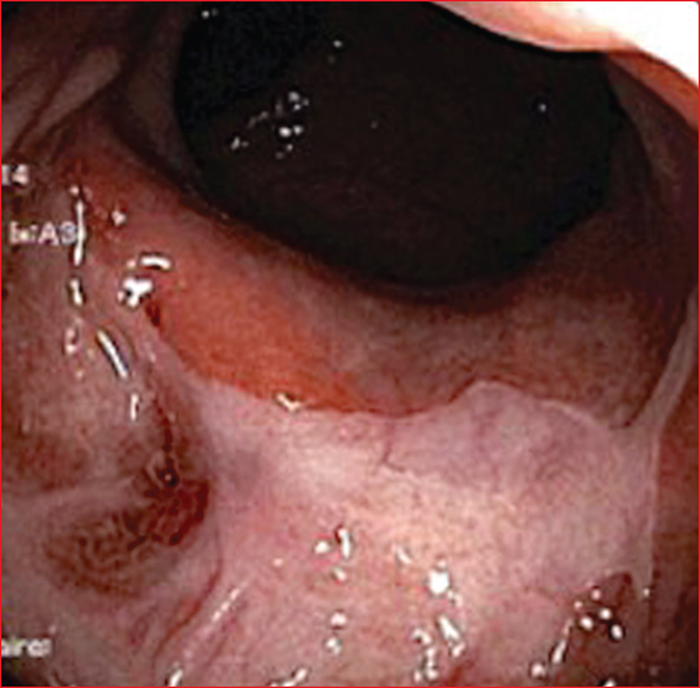
Figure 2 -
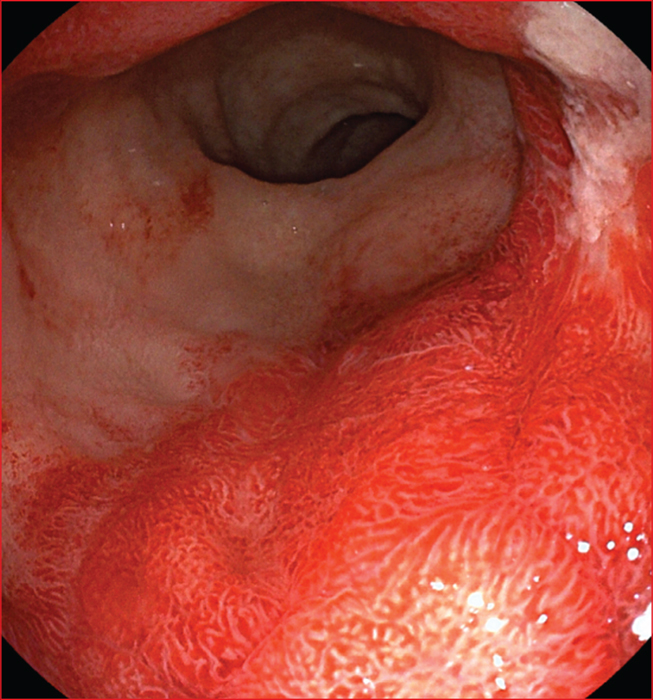
Figure 3 -
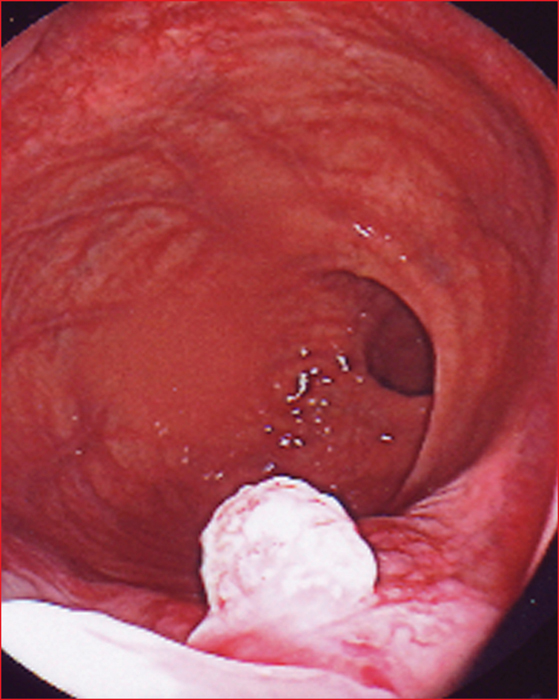
Figure 4 -
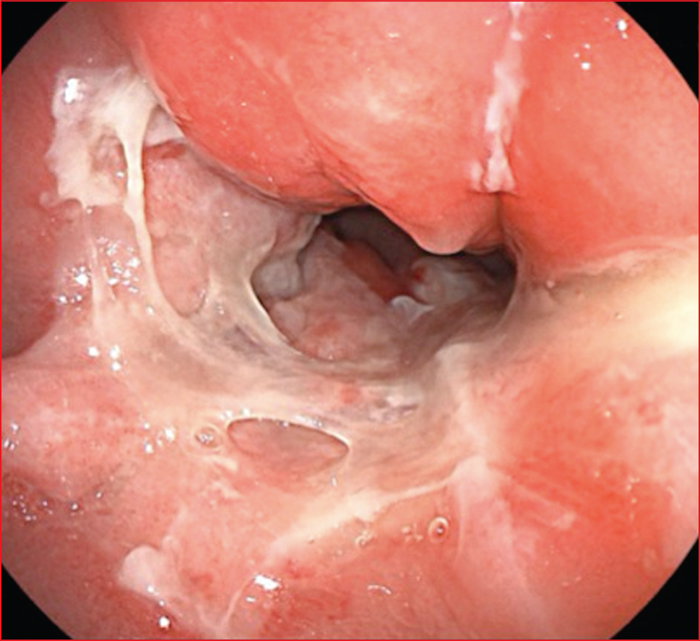
Figure 5 -
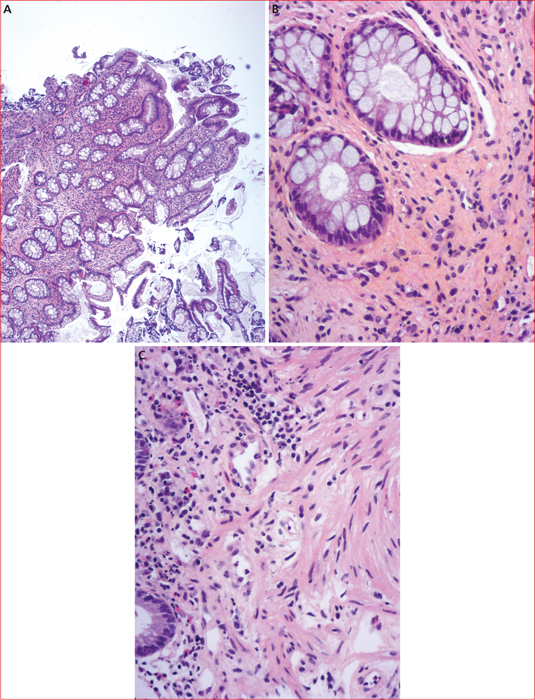
Figure 6 -
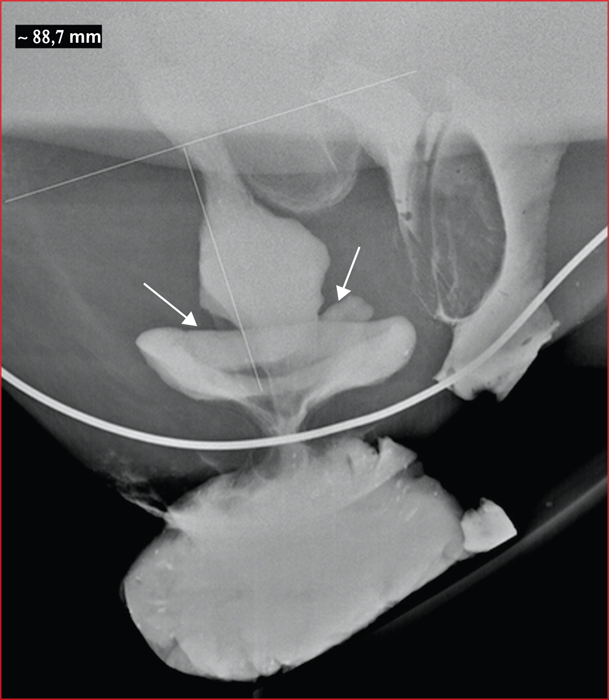
Figure 7 -
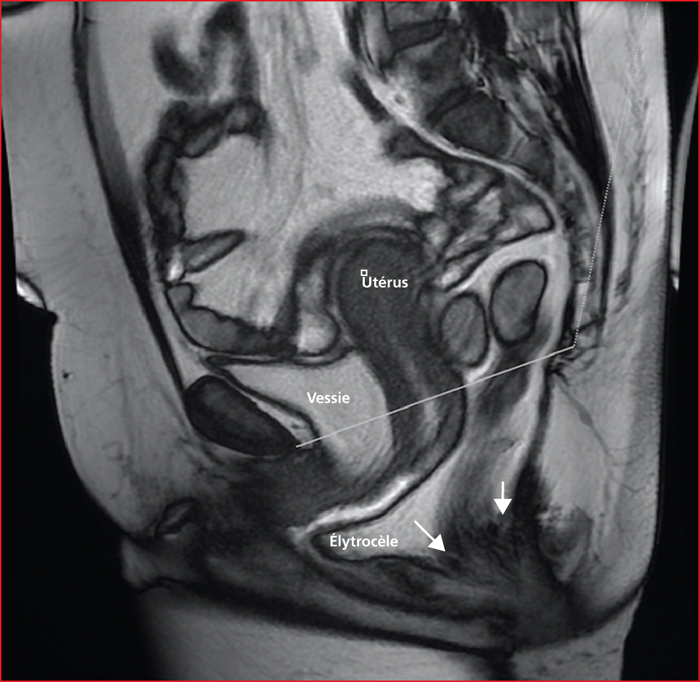
Figure 8 -
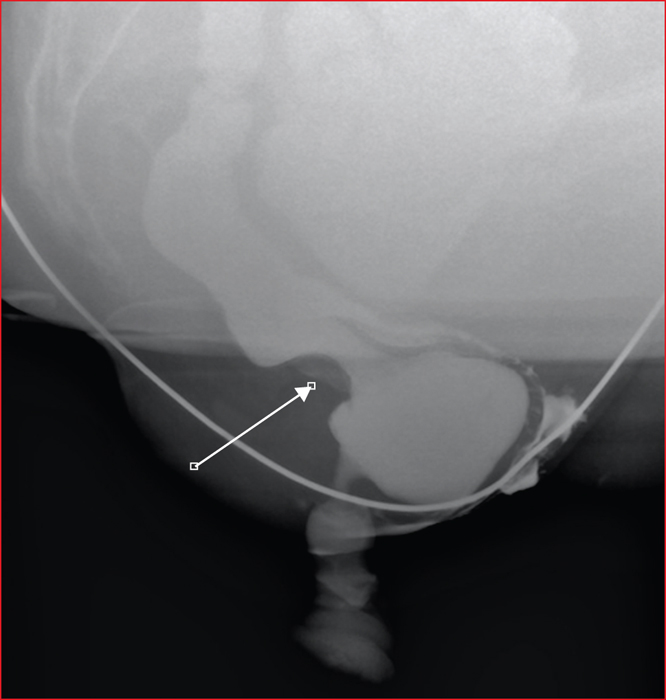
Figure 9 -
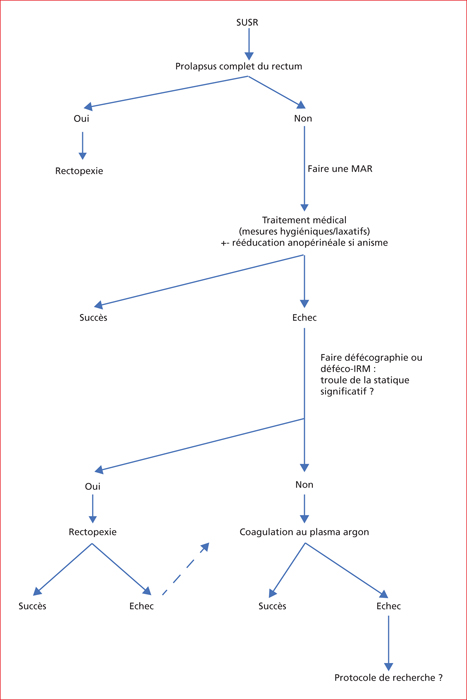
Figure 10 -
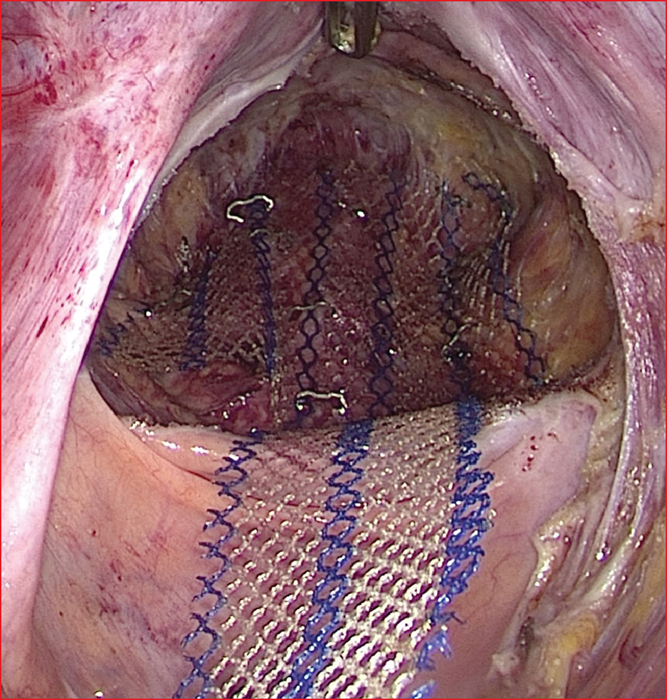
Figure 11
Tables
- Key words: solitary rectal ulcer syndrom, rectal prolapse, dyschezia, puborectalis muscle, biofeedback, ventral rectopexy
- DOI : 10.1684/hpg.2019.1797
- Page(s) : 605-15
- Published in: 2019
Solitary rectal ulcer syndrome (SRUS) is a benign, chronic and rare rectal disease. The incidence is estimated at 1/100,000 per year but SRUS is probably underdiagnosed. It most often affects the young adult, around the 3rd and 4th decades. However, cases have been reported in the elderly and in children. Its pathophysiology is not fully understood but mainly involves rectal prolapse and abnormal contraction of the puborectalis muscle during defecation. The diagnosis is based on the combination of clinical, endoscopic and histological criteria. Bleeding is the most common symptom, often associated with constipation and/or dyschesia, pain and mucus emission from the anus. The classic ulcer located on the anterior wall of the rectum is inconstant. SRUS may appear as a congestive or pseudopolypoidal proctitis or multiple or even circumferential ulcerations. The main differential diagnoses are cancer, IBD and infectious proctitis. Histological findings assess the diagnostic. Complementary examinations, anorectal manometry and dynamic pelvic explorations, specify the mechanism and can guide the treatment. The evolution of the SUSR is unpredictable. Its social repercussions can be significant, especially for young adults. The management of the SRUS is difficult. In cases of complete rectal prolapse, surgery for the correction of prolapse can be proposed. Otherwise, the treatment combines first-line transit regularization, defecatory hygiene measures and biofeedback, but their effectiveness is inconsistent. Argon plasma coagulation of haemorrhagic ulcers is a promising “last resort” technique. In all cases the management must be multidisciplinary. The rate of recurrence is high.
![]() This work is licensed under a
Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License
This work is licensed under a
Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License

