Gériatrie et Psychologie Neuropsychiatrie du Vieillissement
MENUMedication reconciliation: a tool to prevent adverse drug events in geriatrics medicine Volume 15, issue 1, Mars 2017
Figures
- Key words: geriatrics clinical pharmacist, medication errors, aged, medication reconciliation
- DOI : 10.1684/pnv.2016.0642
- Page(s) : 19-24
- Published in: 2017
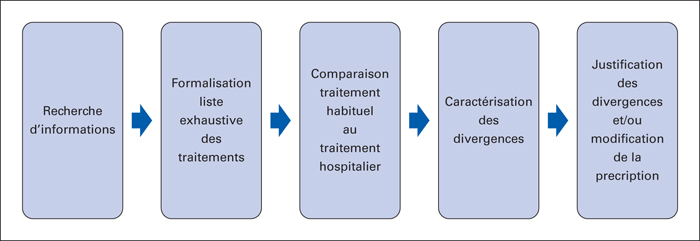
Iatrogenic effects represent a large part of emergency admissions among elderly people. Throughout the care pathway of a patient, whether he is at home or hospitalized, many different health professionals are involved regarding the patient's medication. Medication reconciliation is one way to prevent adverse drug events at all care transitions for every patient by eliminating undocumented intentional discrepancies and unintentional discrepancies in the patient's medication. The aim of this article is to present the different activities of clinical pharmacy developed since 2011 in a follow up and rehabilitation geriatric care service, including medication reconciliation activity. Monitoring of this activity started in March 2014, indicators show that almost 90% of patients were reconciled at admission and discharge from the geriatric unit. Physicians and pharmacists play an active role in reviewing, managing and monitoring a patient's medication. Care coordination and communication among the many members of the medical care team have become one of the greatest challenges healthcare professionals face. At the time of discharge, the patient also plays a key role in medication reconciliation and should be educated when it's possible on the importance of managing medication information. Finally, the hospital pharmacist's role is to keep the primary care physicians and community pharmacists informed about medication changes.