Epileptic Disorders
MENUAwake craniotomy for epilepsy surgery on eloquent speech areas: a single-centre experience Volume 23, issue 2, April 2021
- Key words: epilepsy surgery, awake craniotomy, eloquent cortex, cortical stimulation
- DOI : 10.1684/epd.2021.1275
- Page(s) : 347-56
- Published in: 2021
Objective.
In patients with intractable partial epilepsy who are eligible for epilepsy surgery, the best seizure control requires complete resection of the epileptogenic zone. When the epileptogenic zone is located very near to, or even with the eloquent cortex, this can be a challenge. In this study, we investigated the efficacy of awake craniotomy techniques to completely resect these epileptic zones while preserving the neural functions.
Methods.
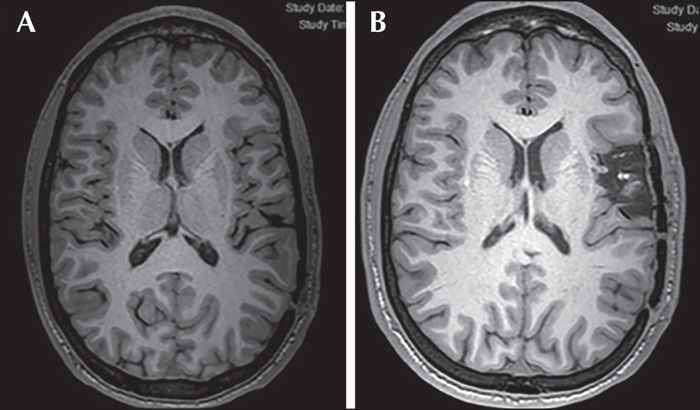
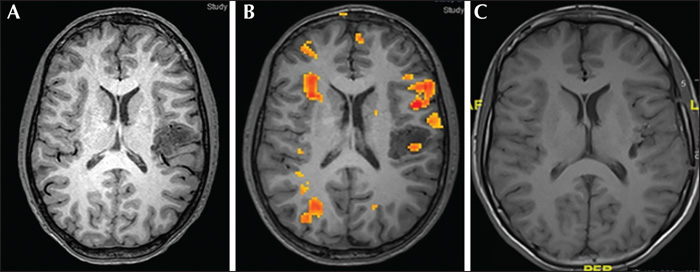
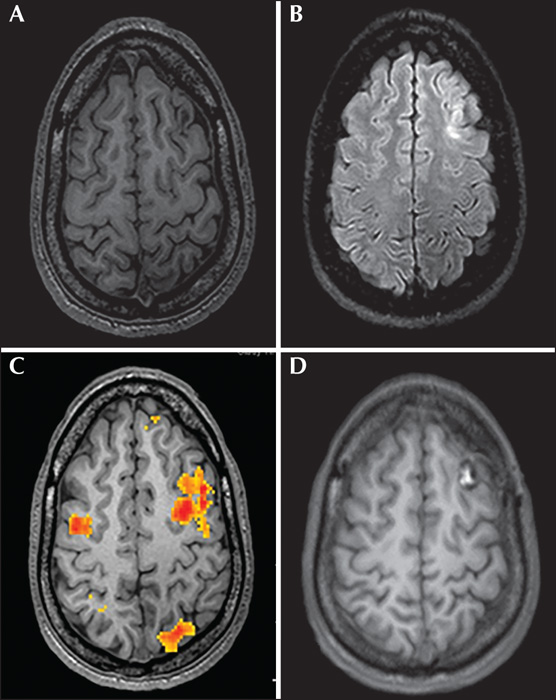
We conducted a retrospective cohort study of 17 consecutive patients with intractable partial seizures of different aetiologies (non-lesional epilepsy [n=3], tuberous sclerosis [n=1], hypoxic ischaemic insult [n=1], dysembryoplastic neuroepithelial tumours [DNET] [n=2], focal cortical dysplasia type 2 [FCD] [n=4], and other malformations of cortical development [n=6]), located in eloquent language cortex (frontal [n=7], insular [n=5], and latero-temporal [n=5] regions). All patients were operated on between 2010 and 2019 for resective epilepsy surgery under awake conditions, with the aid of direct cortical stimulation. This report aimed to study the feasibility, efficacy and limitations of using the awake craniotomy technique for surgical resections of epileptogenic zones involving eloquent language cortex.
Results.
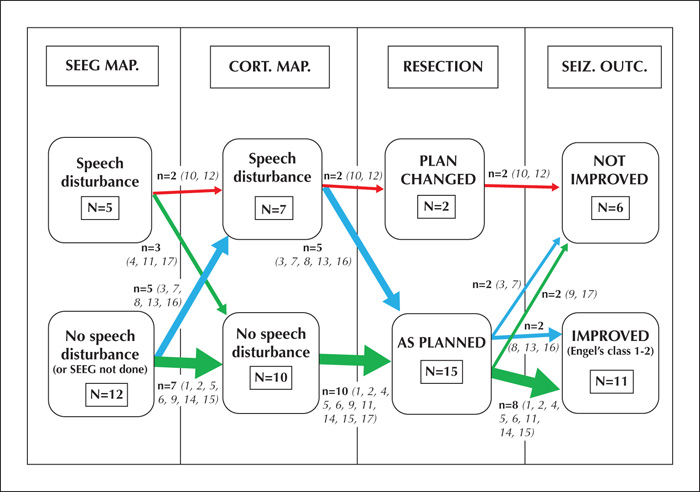
Postoperative epilepsy control and neurological function were assessed and followed. The mean follow-up period was 5.7 years. In one patient, the surgery was aborted before resection. In the other patients, Engel Class I was achieved in seven patients (43.75%) and Engel Class II in four patients (25%), and worthwhile improvement (Engel Class I and II) was achieved in 11 patients (68.75%). Postoperative neurological deficits were encountered in four patients (23.5%). However, all these deficits were regressive and were absent at the last follow-up visit.
Significance.
Using the awake craniotomy technique, seizure freedom can be achieved in a high proportion of patients with epileptogenic zones located in language areas, who were previously considered only candidates for palliative measures.