Hématologie
MENUIndications and procedure for CAR T-cell infusion Ahead of print
Figures
Tables
- Key words: care pathway, eligibility, cytokine release syndrome, immune effector cell-associated neurotoxicity syndrome
- DOI : 10.1684/hma.2022.1712
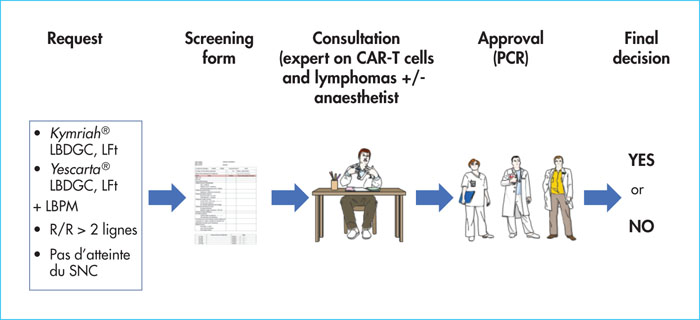
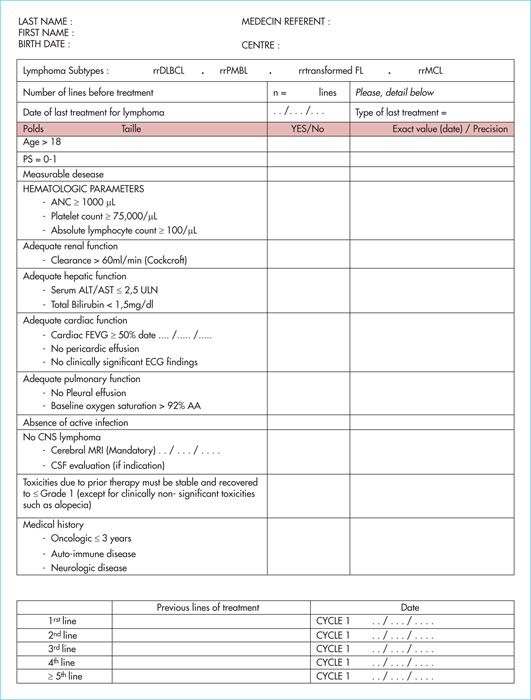
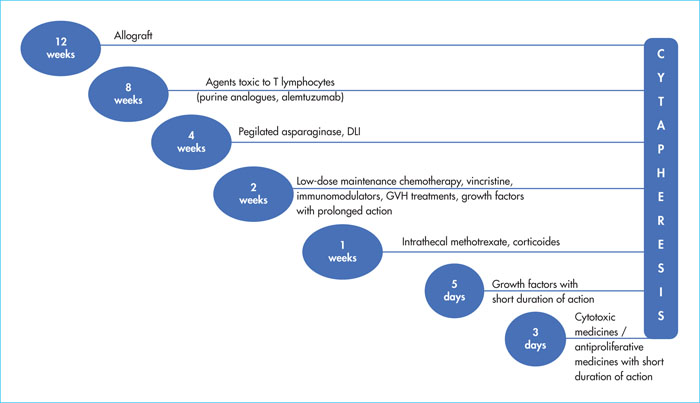
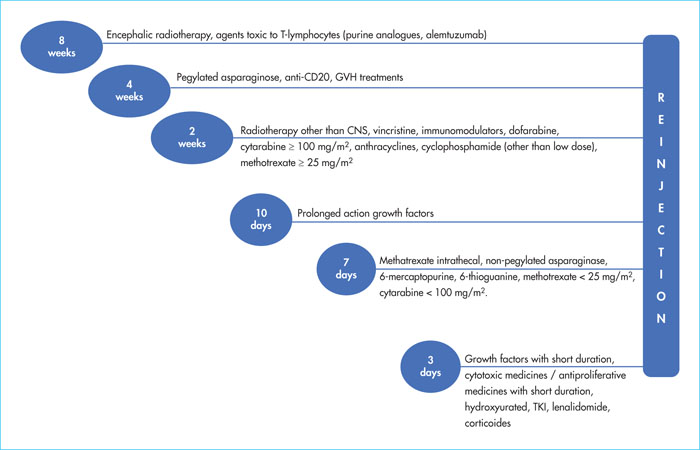
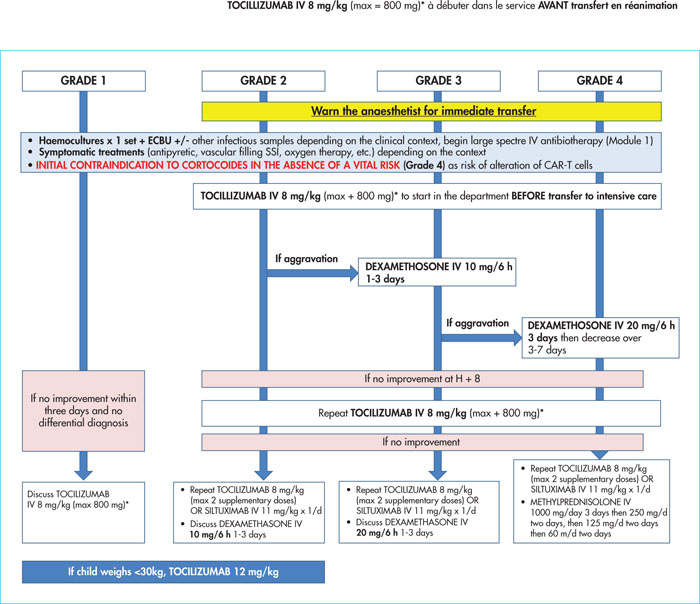
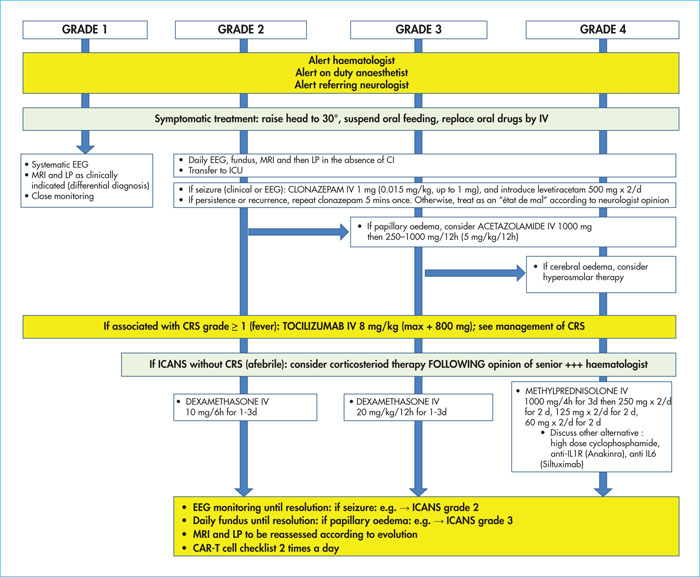
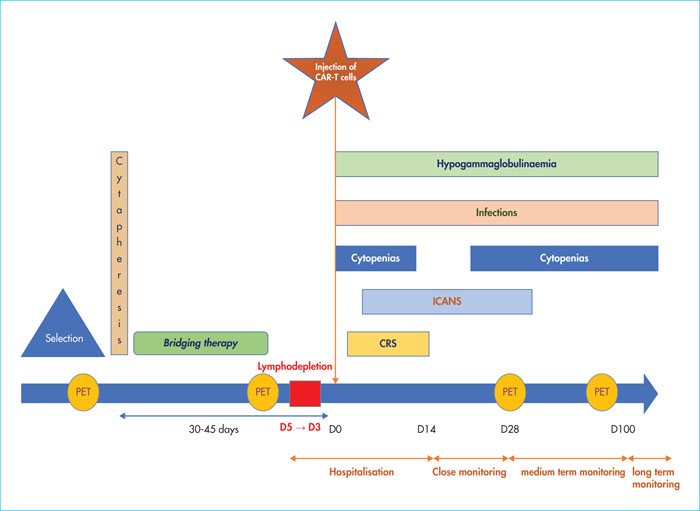
The use of anti-CD19 CAR-T cells (chimeric antigen receptor T-cells) in B-cell malignancies, in particular in relapse/refractory B-cell acute lymphoblastic leukaemia (ALL) and in diffuse large B-cell lymphoma (DLBCL), is increasing. Understanding the indications, contra-indications, and eligibility criteria is fundamental in order to optimise the use of this new therapy. Patients’ care pathways and referrals to centres accredited for the injection of CAR T-cells are now effective. Close collaboration between the patient centre and the CAR-T cell centre is the key for good medical care. Between the inclusion in the process and reinjection of the CAR-T cells, the patient often needs bridging therapy. In this article, we will provide details about how and when to stop anti-neoplastic and immunosuppressive drugs before cytapheresis and infusion. Information about the benefits, adverse events and practical modalities are presented in a multidisciplinary way, by the doctor and coordinating nurse. Recently, expert groups have proposed therapeutic algorithms for the two most frequent toxicities: cytokine release syndrome and immune effector cell-associated neurotoxicity syndrome, thus allowing a harmonisation of practices between the different CAR T-cell centres. We will also cover other complications including cytopenias, hypogammaglobulinaemia and infectious diseases. A multidisciplinary team is required involving haematologists, intensive care unit physicians, infectious disease specialists, neurologists, neuropsychologists, biologists, nuclear medicine specialists, radiologists, pharmacists, and the apheresis centre, together with the coordinating nurse. It is compulsory for CAR-T cell accreditation for centres to draft management procedures for these complications and for the interactions between these different actors.