Epileptic Disorders
MENUNon-convulsive febrile status epilepticus mimicking a postictal state after a febrile seizure: an ictal electroclinical and evolutive study Volume 24, issue 2, April 2022
- Key words: febrile seizures, febrile status epilepticus, twilight state, ictal EEG
- DOI : 10.1684/epd.2021.1402
- Page(s) : 387-96
- Published in: 2022
Objective
Febrile status epilepticus evolves from a febrile seizure (FS) in 5% of cases. Its prompt recognition is challenging, especially when motor manifestations are absent or subtle. We describe the ictal electroclinical features of non-convulsive febrile status epilepticus (NCFSE) following an apparently concluded FS, initially misinterpreted as postictal obtundation and in some way mimicking the described “non-epileptic twilight state”.
Methods
We present an electroclinical study of 18 children, collected in our unit, who presented with NCFSE after an apparently resolved FS, longitudinally followed for one year to seven years and nine months (mean: four years and three months). The age at first NCFSE ranged between one year and two months and five years and eight months (mean: two years and six months). Patients were examined after spontaneous or rectal diazepam-induced resolution of a FS, while showing persisting impairment of awareness.
Results
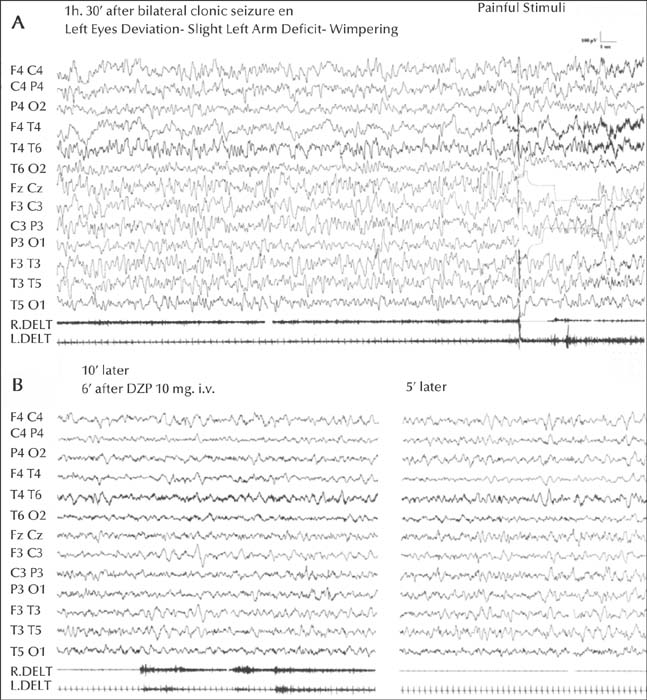
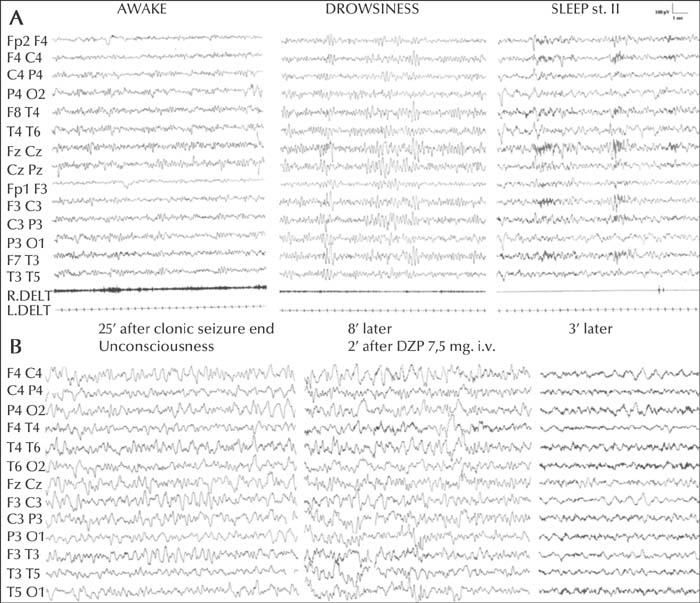
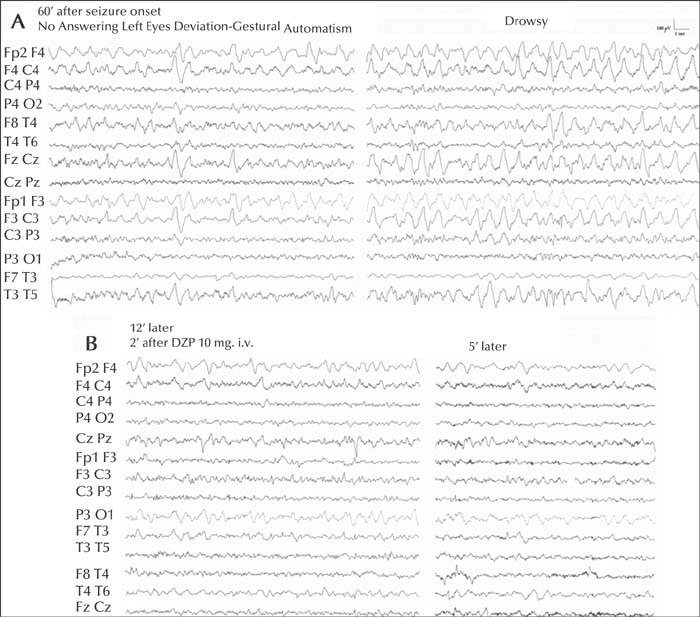
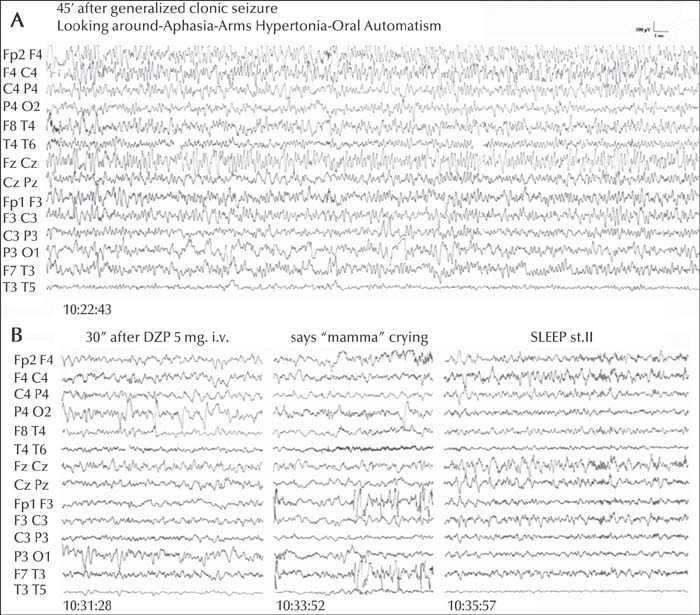
A lack of responsiveness to painful stimulation, abnormal posturing and aphasia were present in all cases, variably associated with perioral cyanosis, hypersalivation, automatisms, gaze deviation and other lateralizing signs; eyes were open. The EEG recording started 20 to 140 minutes after the apparent resolution of the FS and was invariably characterized by delta or theta-delta pseudorhythmic activity, mainly involving the fronto-temporal regions, with hemispheric predominance in two thirds of the cases. The electroclinical condition, lasting 25 to 210 minutes, quickly recovered after intravenous diazepam. Follow-up revealed normal neurodevelopment and EEG in almost all patients (learning disability emerged in three). In five subjects, NCSE relapsed (twice in two). None presented afebrile seizures.
Significance
Our series highlights the electroclinical features of focal NCFSE. Distinctive elements are a lack of reactivity, cyanosis, lateralizing clinical and EEG signs, and resolution clearly tied to intravenous benzodiazepine administration.