Epileptic Disorders
MENUIntraoperative methods for confirmation of correct placement of the vagus nerve stimulator Volume 3, issue 2, June 2001
- Key words: vagus nerve stimulation, intraoperative testing, lead placement
- Page(s) : 75-8
- Published in: 2001
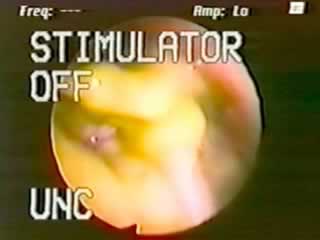
Vagus nerve stimulation is a progressive therapy for intractable epilepsy. Variations in cervical anatomy can complicate localization of the vagus nerve and may lead to inappropriate placement of the stimulator leads. We have developed two intraoperative techniques that improve correct identification of the vagus nerve. Both of these techniques utilize the co-localization of the recurrent laryngeal nerve with the vagus nerve. For patients undergoing stimulator placement with regional and local anesthesia, the stimulator current intensity is increased until alteration of voice can be confirmed with a voice test. Patients undergoing general anesthesia can also be tested by direct stimulation of the isolated vagus nerve. Utilizing visualization of the larynx and vocal cords via fiberoptic endoscopy, direct stimulation of the vagus nerve will produce a contraction of the left lateral wall of the larynx and tightening of the left vocal cord. Neither of these procedures produce any untoward effects for the patients. We have found these methods improve our ability to confirm correct placement of the stimulator with minimal increase in operative time (with Video).