Epileptic Disorders
MENUILAE Neuroimaging Task Force highlight: Review MRI scans with semiology in mind Volume 22, issue 5, October 2020
- Key words: ictal semiology, MRI, DNET
- DOI : 10.1684/epd.2020.1202
- Page(s) : 683-7
- Published in: 2020
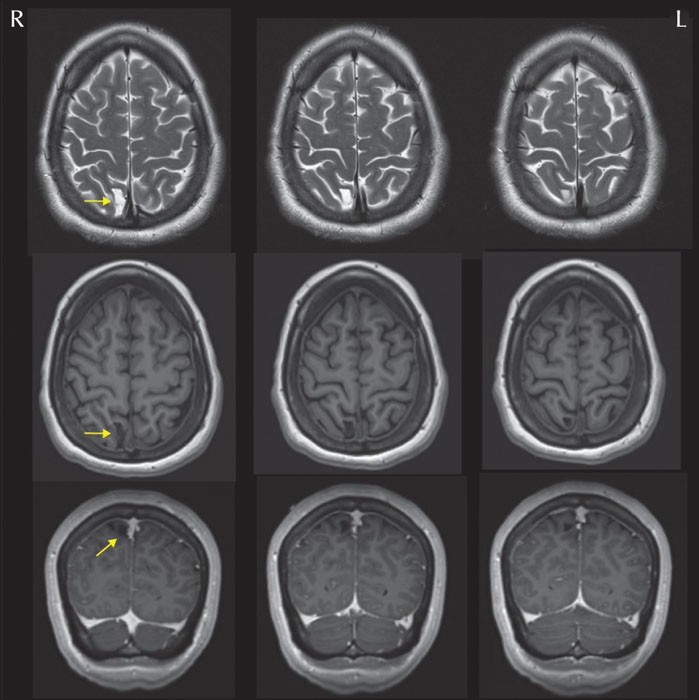
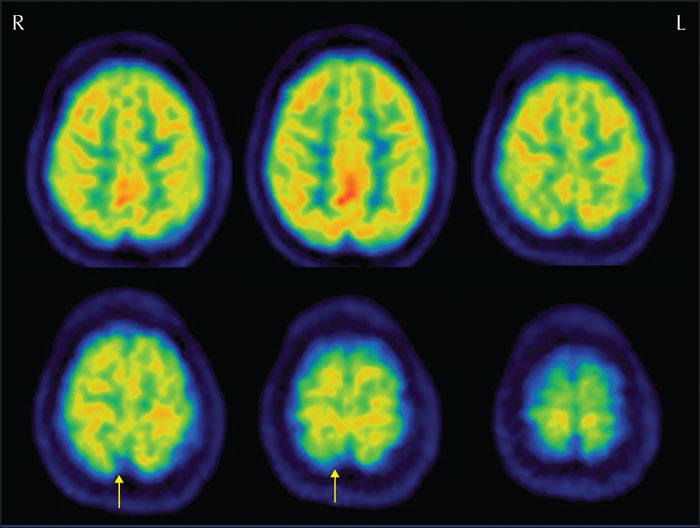
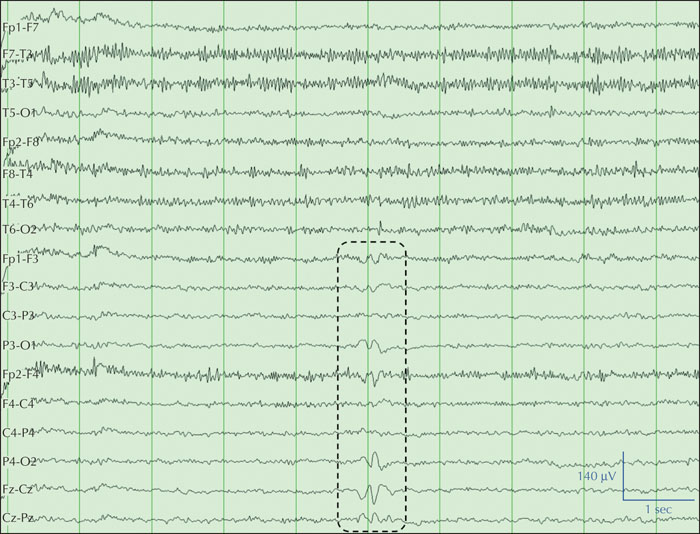
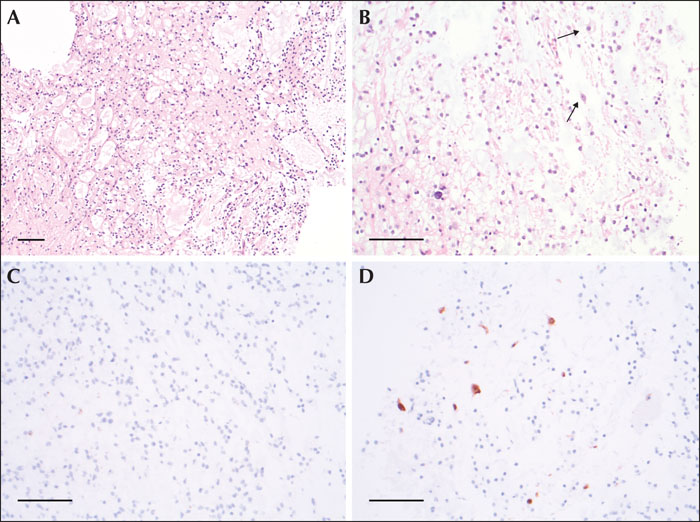
The ILAE Neuroimaging Task Force aims to publish educational case reports highlighting basic aspects related to neuroimaging in epilepsy consistent with the educational mission of the ILAE. It is important to obtain MRI scans early in the clinical course of epilepsy, using an optimized protocol. Furthermore, it is critical that MRI scans are reviewed by experts who have been provided with all the clinical information and results from other investigations. We report a patient with a 21-year history of drug-resistant seizures who was admitted from another centre for presurgical evaluation. She had four previous MRI scans from this centre which were reported as unremarkable. However, a review of the MRI scan obtained on the day of admission, with the patient's ictal semiology in mind, resulted in identification of an epileptogenic lesion which was later confirmed by video-EEG monitoring and interictal PET. This lesion was present on all previous MRI scans and showed no change. The patient underwent lesionectomy, and histopathology of the resected specimen was consistent with a dysembryoplastic neuroepithelial tumour. The patient remains seizure-free, 2.5 years after surgery. This case highlights the importance of obtaining detailed descriptions of seizure semiology and considering them when reviewing MR images.