Epileptic Disorders
MENUFall related to epileptic seizures in the elderly Volume 17, issue 3, September 2015
Figures
- Key words: injury, epilepsy, EEG, antiepileptic drug, age
- DOI : 10.1684/epd.2015.0752
- Page(s) : 287-91
- Published in: 2015
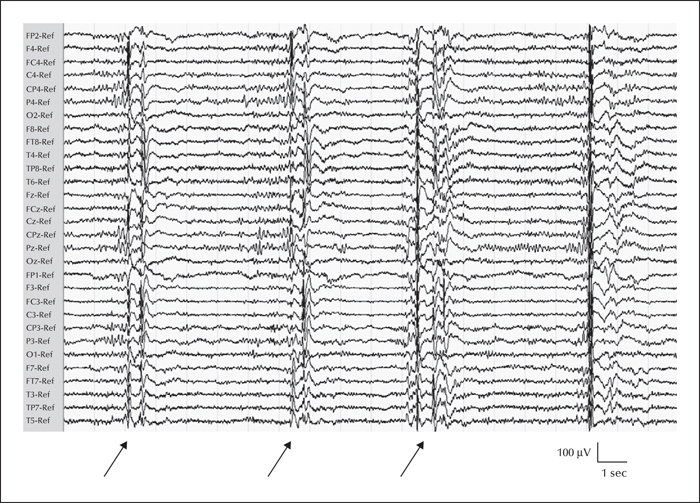
It is well known that both falls and epileptic seizures are very frequent and harmful in the elderly. Moreover, although seizures may cause falls, their relationship is poorly documented in this population. We report four women (mean age: 84.5 years) who presented falls with: late-onset focal seizures of possible parietal (Case 1) or frontal localisation (Case 2), early onset with late aggravation of juvenile myoclonic epilepsy (Case 3), and generalised situation-related myoclonic seizures (Case 4). Falls were presumably associated with tonic posturing of left (Case 1) or right (Case 2) hemibody, to bilateral and massive myoclonic jerks (Cases 3 and 4) with a loss of consciousness (Case 3). The diagnosis of seizures was difficult and routine EEG was unremarkable in Cases 1 and 2, requiring video-EEG monitoring to capture the clinical events. Adequate treatment offered recovery from seizures and falls in all patients. Other mechanisms of seizure-induced falls in older patients and their management are discussed. In conclusion, falls may be caused by different seizure types and appear to be underestimated due to difficulties in seizure diagnosis in the elderly. Recognizing falls related to seizures is important in geriatric practice, as it facilitates adequate management.