Epileptic Disorders
MENUEpilepsy, interictal EEG abnormalities and hippocampal atrophy in patients with calcified neurocysticercosis: a population study in an endemic milieu Volume 23, issue 2, April 2021
- Key words: neurocysticercosis, cysticercosis, hippocampal atrophy, epilepsy, EEG abnormalities, inflammation, population study
- DOI : 10.1684/epd.2021.1276
- Page(s) : 357-65
- Published in: 2021
Objective
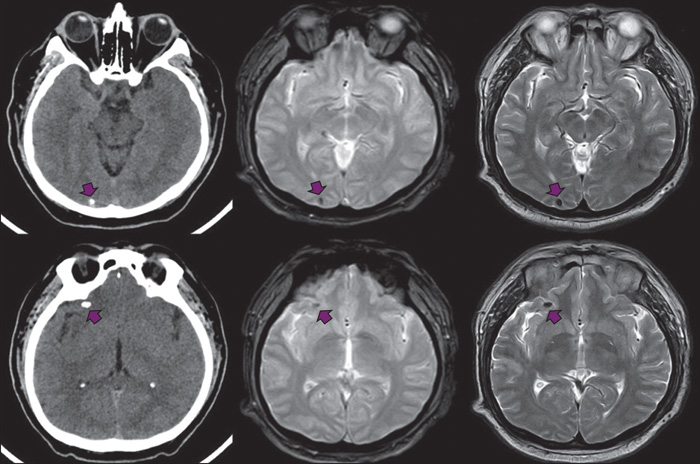
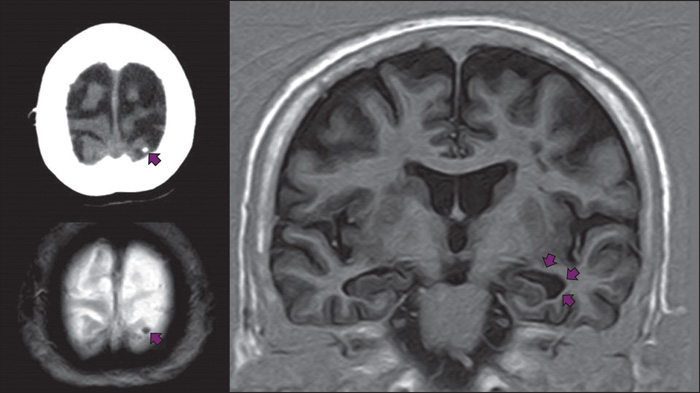
Calcified neurocysticercosis has been associated with hippocampal atrophy (HA). However, the pathogenesis of this association is still elusive. This study assessed the role of epilepsy or interictal EEG abnormalities in the occurrence of HA in the Atahualpa Project cohort.
Methods
Atahualpa residents aged ≥20 years, identified by means of door-to-door surveys, were offered an unenhanced head CT to identify neurocysticercosis cases. Individuals with cysticercotic parenchymal brain calcifications (121/1,299; 9.3%) underwent brain MRI, scalp EEG, and neurological evaluation to assess history of epilepsy. The independent association between combined exposures (epilepsy and/or EEG abnormalities) and HA (outcome) was assessed using univariate logistic regression models and a multivariate model adjusted for age, sex, level of education, alcohol intake and characteristics of calcifications.
Results
A total of 112 NCC patients were enrolled (mean age: 52.2 ± 16.9 years; 67% women); the remaining nine declined consent. A single calcification was noticed in 70% of cases. Thirty-one patients (27.7%) had HA, which was asymmetrical in 14. Calcification burden was higher among patients with HA than in their non-atrophic counterparts (p=0.012). Eighteen patients had epilepsy, abnormal EEG recordings, or both. Nine of these 18 patients (50%) had HA as opposed to 22 of 94 patients (23%) with a normal EEG and no history of epilepsy (p=0.025). This association became borderline significant based on a multivariate logistic regression model, after adjusting for all covariates (OR: 3.26; 95% CI: 0.91-11.68; p=0.070). In this model, having only one calcification was inversely associated with HA (OR: 0.32; 95% CI: 0.11-0.95; p=0.039).
Significance
Epilepsy and EEG abnormalities play a minor contributory role in the development of HA in neurocysticercosis patients. The burden of infection, leading to recurrent bouts of inflammation around calcified cysticerci, is a more likely contributor to HA development in patients with neurocysticercosis.