Epileptic Disorders
MENUDe novo psychosis after left temporal lobectomy: a case of forced normalization? Volume 24, issue 1, February 2022
- Key words: forced normalization, epilepsy surgery, psychosis, temporal lobe seizure, partial epilepsy, drug-resistant epilepsy
- DOI : 10.1684/epd.2021.1380
- Page(s) : 191-6
- Published in: 2022
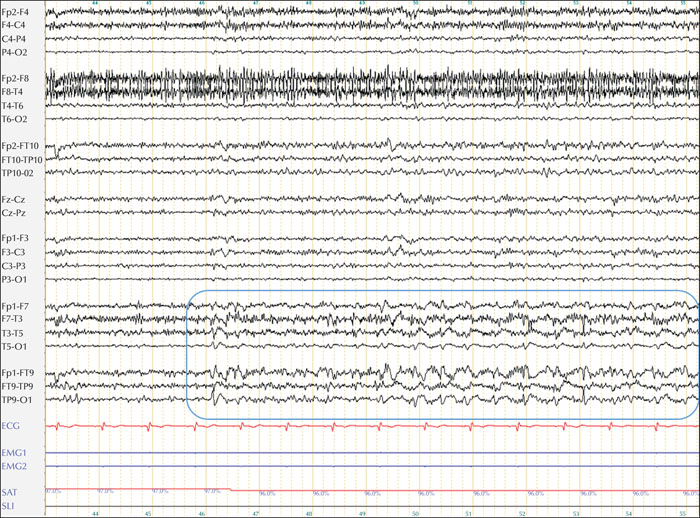
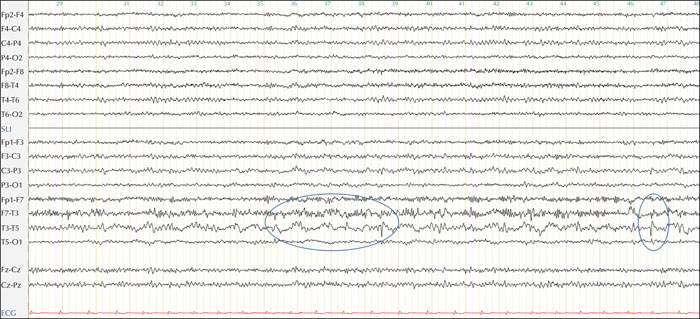
Forced normalization is a clinical entity defined by the appearance of psychiatric disturbance following control of epileptic seizures that were previously uncontrolled. It was first described by Landolt in 1953. The first cases described were mostly psychosis, however, subsequent work suggested that any behavioural disturbance of acute/or subacute onset concomitant with seizure control could be considered as forced normalization. We report the case of a 65-year-old, right-handed Caucasian patient who was followed in the Epilepsy Centre of Marseille, for left temporal drug-resistant epilepsy. The frequency of seizures was one seizure per month at the time before surgery. Left anterior temporal lobectomy was proposed based on presurgical evaluation. The patient remained seizure-free after surgery, but he presented with an episode of acute psychosis three months after. At this point, EEG was performed, showing rare left temporal epileptiform activity mainly provoked by hyperventilation, with breach rhythm over the left temporal surgical. The appearance of acute psychosis after cessation of epileptic seizures and reduced epileptiform activity on the EEG led us to question the forced normalization process in this case. Another hypothesis would be the effect of surgery itself, since there is an increased risk of any psychiatric disturbance unrelated to seizure cessation during the postoperative period. In conclusion, psychosis in this case could have resulted from the combination of several factors, including the effect of surgery itself and seizure cessation. This case illustrates the need for specific psychiatric care in the perioperative period in patients with epilepsy.