Hépato-Gastro & Oncologie Digestive
MENUAblation therapies for Barrett's esophagus: which alternatives to radiofrequency? Volume 26, issue 1, Janvier 2019
- Key words: Barrett's esophagus, dysplasia, radiofrequency ablation, cryoablation, argon plasma coagulation
- DOI : 10.1684/hpg.2018.1727
- Page(s) : 42-9
- Published in: 2019
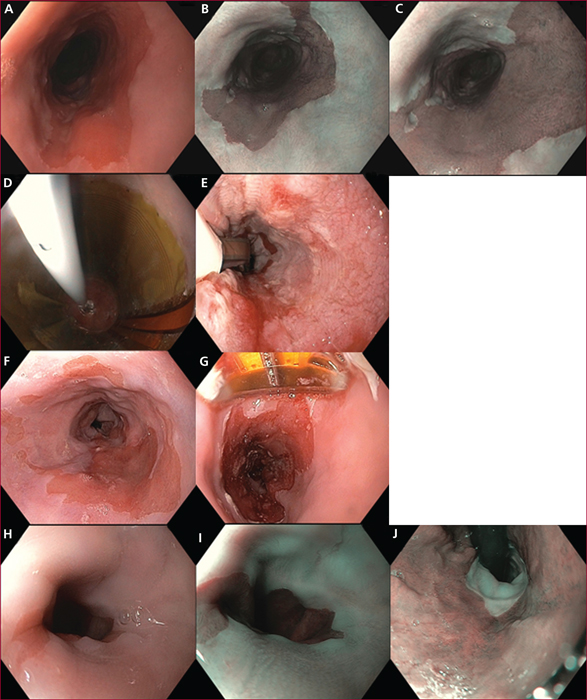
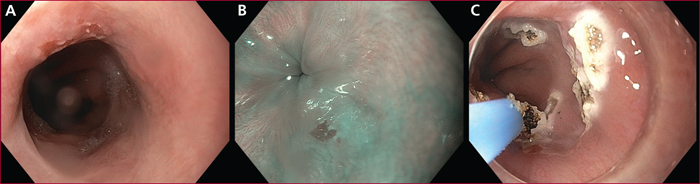
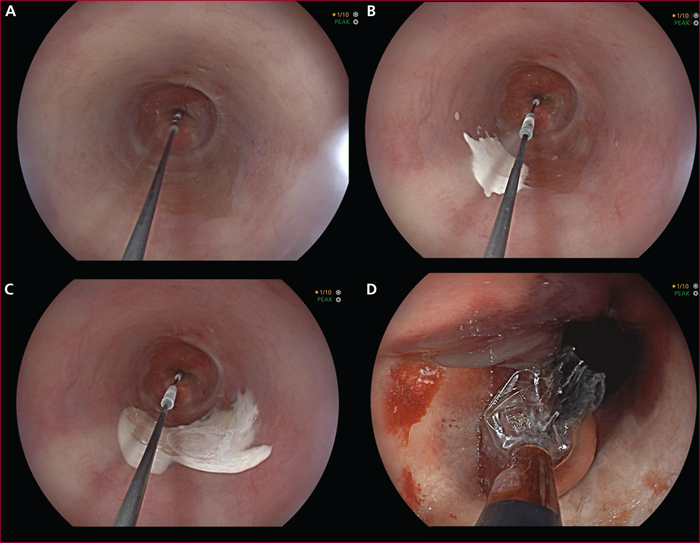
After the endoscopic resection of an early neoplasia arising in Barrett's esophagus, eradication of intestinal metaplasia is recommended to prevent metachronous recurrence of esophageal neoplasia. Given the high stricture rates after extensive endoscopic resection for Barrett's esophagus, endoscopic ablative techniques are currently recommended. They include radiofrequency ablation, argon plasma coagulation, and cryoablation. The other indications for ablation are flat, high grade dysplasia, and more recently, low grade dysplastic Barrett's esophagus in selected patients with a high risk of neoplastic progression. The outcomes are good, with 90-92% eradication rates of intestinal metaplasia, but long-term follow-up data report 8% annual recurrence rate of intestinal metaplasia at the gastroesophageal junction, most of the time non dysplastic. Ablative techniques have an excellent safety profile, with virtually no early morbidity except from chest pain, and about 8% strictures. However, their use is limited by their high cost, the occurrence of buried metaplasia in up to 20% of patients, and the absence of histological assessment of the treated mucosa, requiring a minute endoscopic examination to rule out any visible lesion that would indicate endoscopic resection. Radiofrequency ablation is the most widely studied ablation technique, and currently the best to treat circumferential Barrett's esophagus. However, data on a new argon plasma coagulation device allowing for submucosal injection (Hybrid APC) and cryoablation are encouraging and make of these techniques acceptable alternatives to radiofrequency ablation.
![]() This work is licensed under a
Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License
This work is licensed under a
Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License