Hépato-Gastro & Oncologie Digestive
MENUAutoimmune pancreatitis Volume 24, issue 8, Octobre 2017
- Key words: autoimmune pancreatitis, IgG4, cholangitis, acute pancreatitis, pancreatic ductal adenocarcinoma, corticoids, immunosupressive treatment, rituximab
- DOI : 10.1684/hpg.2017.1505
- Page(s) : 846-56
- Published in: 2017
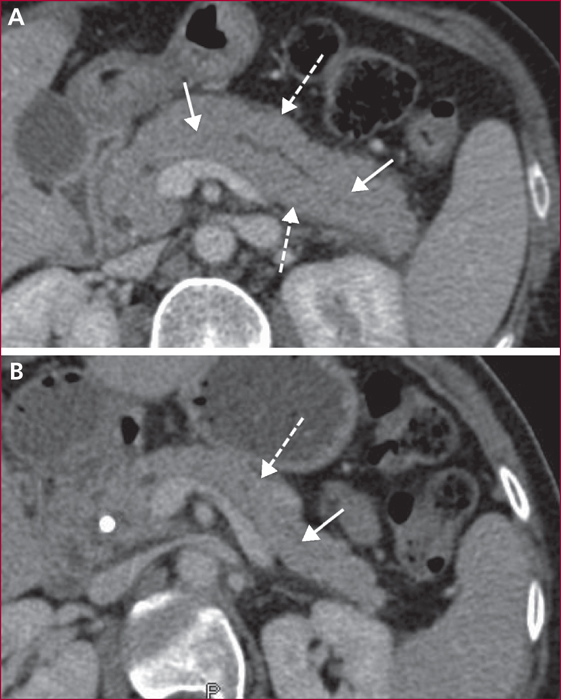
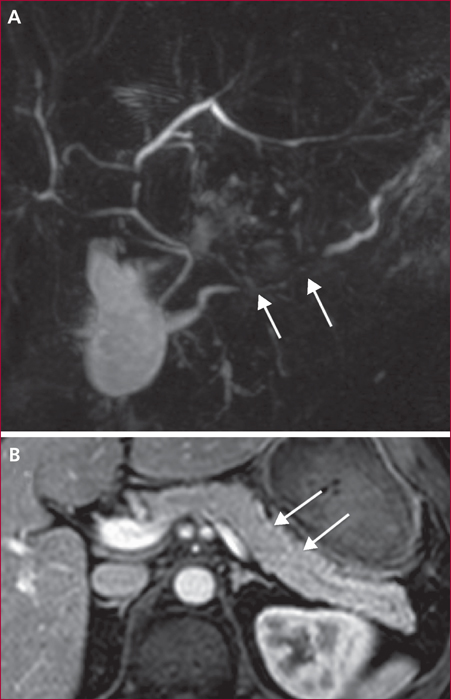
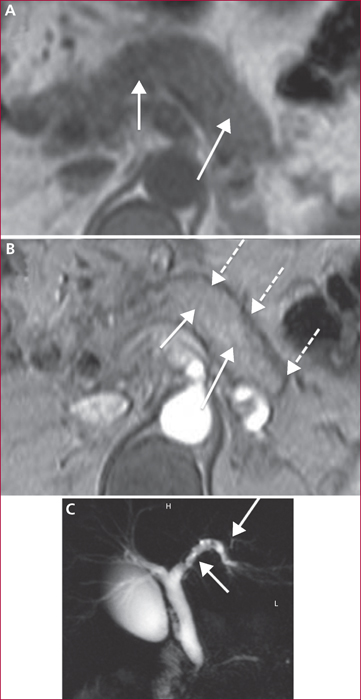
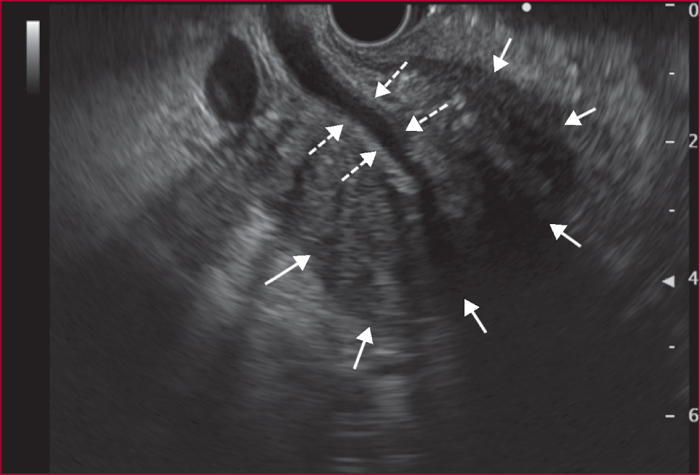
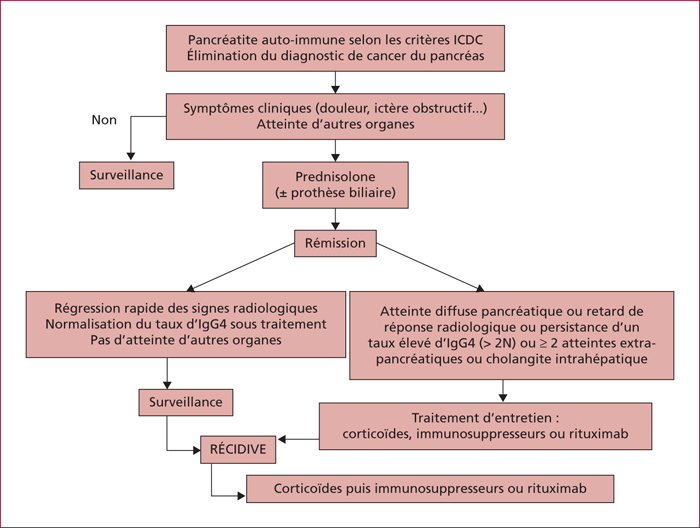
Autoimmune pancreatitis (AIP) is divided into two separate entities. In the type 1 AIP, the pancreatic involvement is associated with an elevated level of serum IgG4 (≥ 2ULN) and, in near 50% of cases, extra-pancreatic lesions mainly on biliary tract, salivary glands, retro-peritoneum, kidneys, and lungs. Type 2 AIP is confined to pancreas except an association with chronic inflammatory bowel disease in 20 to 30% of cases. The main clinical signs are jaundice due to a pseudotumoral form within the pancreatic head and/or sclerosing cholangitis, chronic pancreatic pain, recurrent acute pancreatitis. Diagnosis of AIP is setup upon CT and MRI imaging displaying a focal or diffuses hypo-attenuating swelling (often with a peri-pancreatic “halo” of inflammation), a vanishing main pancreatic duct or segmental stenosis without upstream dilatation. EUS detects diffuse or localized inflammatory aspect of the pancreatic parenchyma together with stenosis of main duct associated with a hyper/hypoechoic wall thickening. EUS-guided fine needle aspiration biopsy may sometimes contribute for the positive and differential diagnosis especially with pancreatic adenocarcinoma. After a therapeutic test with prednisolone during 12 weeks, it is necessary to obtain a rapid (two weeks) regression of both clinical and radiological signs of AIP. If a complete response is obtained in near 90% of cases, a recurrence occurs in 10 to 30% of cases especially for type 1 AIP with a diffuse pancreatic involvement and/or with extra-pancreatic lesions (≥2 such as cholangitis), with a baseline elevated level of serum IgG4 (>4 ULN). In these cases, a second treatment with corticoids is then proposed together with an immunosuppressive maintenance treatment (azathioprine, rituximab) to avoid a subsequent recurrence. The prognosis of AIP is good despite exocrine and endocrine insufficiencies in near 30% of cases.