Hépato-Gastro & Oncologie Digestive
MENUManagement of gastroparesis Volume 21, issue 7, Septembre 2014
Faculté de Médecine et de Pharmacie,
1 rue de Germont,
76031 Rouen Cedex,
France
- Key words: gastric emptying, diabetes mellitus, prokinetics, gastric electrical stimulation, pyloroplasty, nutritional status
- DOI : 10.1684/hpg.2014.1043
- Page(s) : 482-92
- Published in: 2014
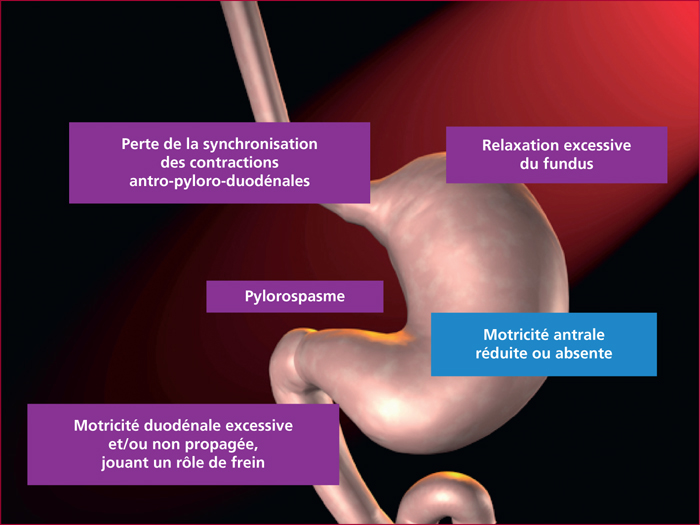
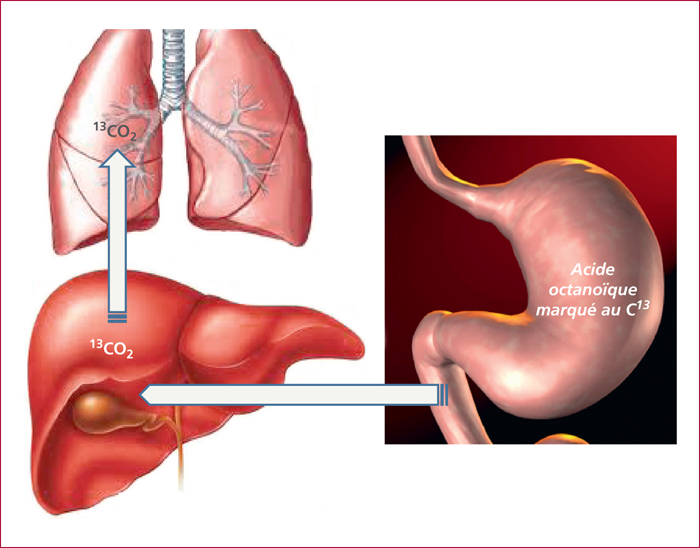
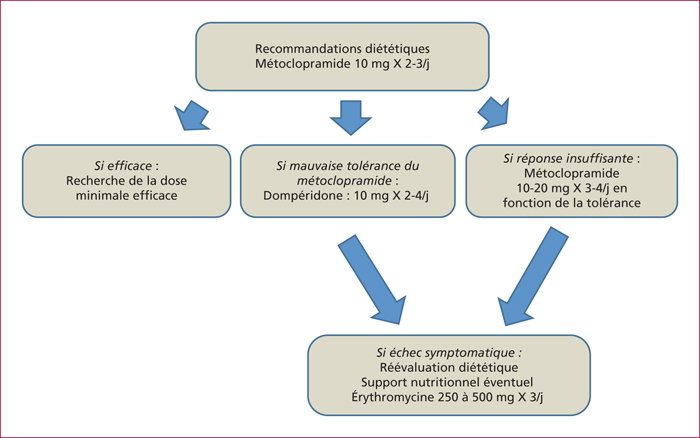
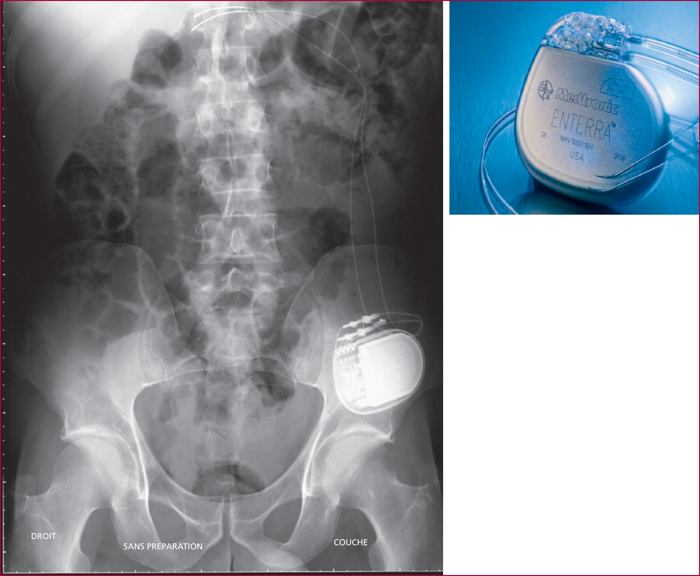
Gastroparesis is characterized by a delayed gastric emptying in the absence of mechanical obstruction. Major underlying conditions are diabetes mellitus (mainly type 1), surgical procedures including a truncal vagotomy and/or a distal gastric resection, the use of some drugs such as opioids or antidepressants. In about 30% of the cases, the gastroparesis is considered idiopathic. The diagnosis of gastroparesis has to be discussed when the patient's complaint is an epigastric fullness relieved by vomiting, a feeling of prolonged gastric emptying or an epigastric pain unexplained by any endoscopic finding. Other suggestive conditions are a poorly controlled diabetes mellitus or a gastroesophageal disease refractory to usual treatment in a compliant patient. A gastric emptying test is necessary to assess the diagnosis because of the low predictive value of symptoms. First-line treatment options include dietary recommendations, prokinetics, antiemetics and the optimal control of diabetes. In refractory cases, even to second-line prokinetics such as erythromycin or azithromycin, other options are, particularly when the nutritional status of the patient is impaired: enteral feeding, gastric electrical stimulation or pyloric endoscopic procedure (dilation or Botox® injections). Whether some patients are potential candidates for surgery remains poorly demonstrated. To date, on the basis of the available data, surgery has to remain an exceptional option.