Epileptic Disorders
MENUFibromyalgia and seizures Volume 18, issue 2, June 2016
- Key words: seizure, fibromyalgia, neurology, spells, psychogenic, non-epileptic
- DOI : 10.1684/epd.2016.0823
- Page(s) : 148-54
- Published in: 2016
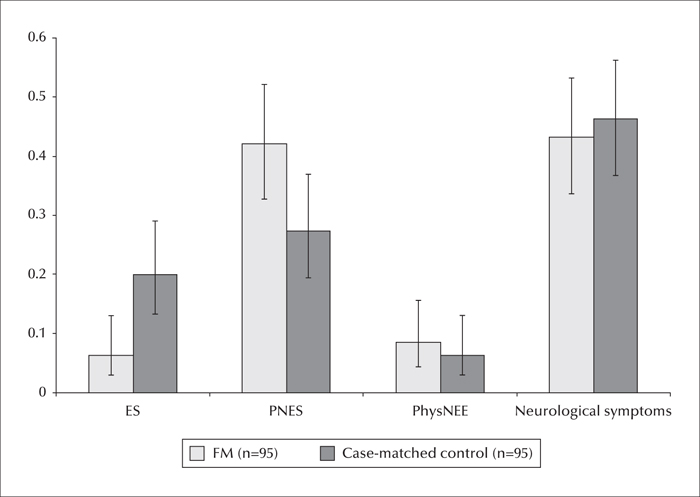
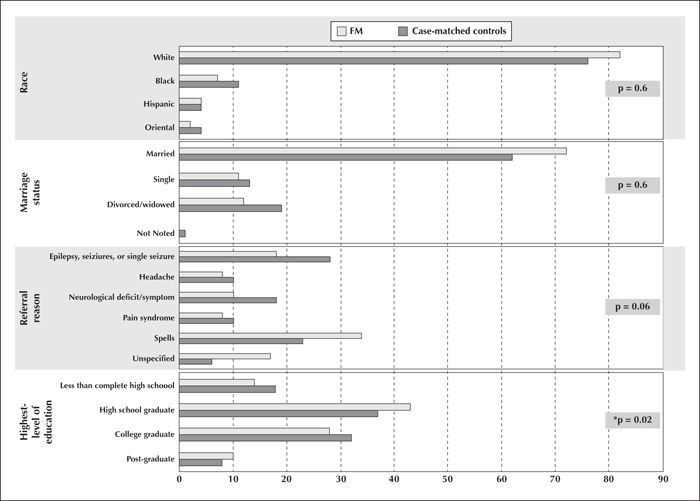
The purpose of this case-matched study was to determine how frequently fibromyalgia is associated with different paroxysmal neurological disorders and explore the utility of fibromyalgia as a predictor for the diagnosis of psychogenic non-epileptic seizures. The billing diagnosis codes of 1,730 new, non-selected patient encounters were reviewed over a three-year period for an epileptologist in a neurology clinic to identify all patients with historical diagnoses of fibromyalgia. The frequency with which epileptic seizures, psychogenic non-epileptic seizures, and physiological non-epileptic events were comorbid with fibromyalgia was assessed. Age and gender case-matched controls were used for a between-group comparison. Wilcoxon tests were used to analyse interval data, and Chi-square was used to analyse categorical data (p<0.05). Fibromyalgia was retrospectively identified in 95/1,730 (5.5%) patients in this cohort. Females represented 95% of the fibromyalgia sample (age: 53 years; 95% CI: 57, 51). Forty-three percent of those with fibromyalgia had a non-paroxysmal, neurological primary clinical diagnosis, most commonly chronic pain. Paroxysmal events were present in 57% of fibromyalgia patients and 54% of case-matched controls. Among patients with fibromyalgia and paroxysmal disorders, 11% had epileptic seizures, 74% had psychogenic non-epileptic seizures, and 15% had physiological non-epileptic events, compared to case-matched controls with 37% epileptic seizures, 51% psychogenic non-epileptic events, and 12% physiological non-epileptic events (p = 0.009). Fibromyalgia was shown to be a predictor for the diagnosis of psychogenic non-epileptic seizures in patients with undifferentiated paroxysmal spells. However, our results suggest that the specificity and sensitivity of fibromyalgia as a marker for psychogenic non-epileptic seizures in a mixed general neurological population of patients is less than previously described.