Epileptic Disorders
MENUAnoxic‐epileptic seizures: home video recordings of epileptic seizures induced by syncopes Volume 6, issue 1, March 2004
Auteur(s) : John Stephenson1, Galen Breningstall2, Chris Steer3, Martin Kirkpatrick4, Iain Horrocks1, Alla Nechay1,5, Sameer Zuberi1
1. Fraser of Allander Neurosciences Unit, Royal Hospital for Sick Children, Glasgow, UK
2. Noran Neurological Clinic and Department of Neurology, University of Minnesota Hospitals, Minneapolis, USA
3. Paediatric Department, Victoria Hospital, Kirkcaldy, UK
4. Paediatric Neurology Department, Ninewells Hospital, Dundee, UK
5. Neurology Department, Paediatric Hospital no. 1, Kyiv, Ukraine
Received October 3, 2003; Accepted November 14, 2003
A few examples of true epileptic seizures induced by syncopal attacks have been reported over the past 20 years [1-15], but almost certainly the sequence of syncope followed by epileptic seizure is under-recognized and misinterpreted. Insofar as the non-epileptic anoxic seizures of pure syncopes and the epileptic seizures as seen in the epilepsies have distinct and totally different mechanisms [5, 16], we have called this sequential combination (of anoxic and epileptic seizure), an anoxic-epileptic seizure [2, 6, 12, 17-19], a terminology followed by others [4, 14]. The purpose of this paper is to provide the first published video-recordings of these anoxic-epileptic seizures (AES). In three home video clips, we show the actual transition from the anoxic seizure to the epileptic seizure, and in two further examples we show the type of epileptic seizure most commonly triggered by syncopes in the very young.
Case studies
Patient 1
A 13 month-old boy from Minnesota, USA presented with a 4-month history of episodic loss of consciousness and convulsion. Typically, after a minor bump or hurt, or after being frustrated he would be upset and agitated and become intensely cyanotic. Then he would lose consciousness and frequently would convulse. Some sort of episode would occur 3 or 4 times a day with the convulsion lasting up to about 2 minutes. He had 3 siblings in good health and a maternal uncle with a history of some kind of seizures. An inter-ictal EEG was normal awake and asleep. Ocular compression induced only minor bradycardia, without asystole [5]. Head CT scan was normal. The impression at this time was that the boy was having cyanotic “breath-holding” spells, otherwise called episodes of prolonged expiratory apnoea, with no more than anoxic seizures without an epileptic component. He had been given carbamazepine without sustained benefit, and later became allergic to this drug.
From about the age of 18 months the semiology changed and he developed a new phenotype. Now, after a minor head injury especially when tired or being made to do something he did not wish to do, he would first have the “breath-holding spell” with the usual stiffening tonic posturing and cyanosis, but then a convulsion would occur lasting for about 4 minutes, with jerking or clicking of the tongue and jerks of his face and limbs. The parents managed to videotape some of these episodes at their home, and review of these recordings confirmed that his “breath-holding spells” were now inducing epileptic seizures. Further details of the video-recorded events are given in video legends patient 1. He was diagnosed with anoxic-epileptic seizures and received anti-epileptic therapy until the age of six years. Two “small seizures” occurred three months later, but he then remitted, with no further episodes aged 10 years.
Patient 2
A 31 month-old girl from Fife Scotland presented with a history of “attacks” from early infancy, probably from around 12 months of age, that were initially, from the parents’ description, typical cyanotic “breath-holding spells” of the prolonged expiratory apnoea variety. During these she would cry out, hold her breath in expiration, become pale and blue and lose consciousness for a few seconds. These episodes would always, on careful enquiry, be triggered by fright, anger, or by hurting herself. The initial frequency was around three times per week but had increased to three times per day over recent weeks. She was an only child, with no family history of epilepsy or syncope.
The attacks had also changed in character from the age of 21 months. Up until then, the sequence of events was described as either crying, holding her breath, going blue and passing out, or, on other occasions, just gasping, going very pale and passing out. Both of these events occurred in response to pain or anger or a fright as before, but after a period of about twenty to thirty seconds of unconsciousness this was followed, on some occasions, by stiffening, followed by jerking of the arms and legs and “twitching” of the eyes for up to five minutes, followed by vacant staring for up to ten minutes. On coming round she would be distressed, ask for a drink and would usually sleep for up to an hour. These modified attacks were now occurring about three times per week.
Observation in hospital on three occasions, immediately after these “new” attacks, revealed no neurological abnormalities and no evidence of fever or systemic upset. Vital signs were all normal and measurement of blood glucose and other routine laboratory tests showed no abnormality. Her EEG and ECG at age 23 months had shown no abnormalities. Her mother had been supplied with rectal diazepam for prolonged episodes (longer than three minutes), and with first aid positional advice; anti-epileptic drugs had not been prescribed.
On examination in the clinic at the age of 31 months, she was a bright, slightly fractious girl who separated poorly from her mother. Both parents were extremely anxious and the mother had given up her job to care for the girl who could not be left with anyone else. It was at this stage that a home video was obtained, and a diagnosis of anoxic-epileptic seizures made (for further details see video legend, patient 2).
At age 36 months, the frequency of the anoxic-epileptic seizures had reduced to weekly, along with breath holding/syncopal attacks up to eight per day. Sodium valproate was commenced but not tolerated: she was changed to carbamazepine, but follow-up remains short. A psychological assessment was requested.
Patient 3
This boy from Massachusetts, USA, was brought by his parents to Glasgow aged eight years. His development had been aberrant. He always walked on his toes and although he could repeat sentences at two years, he made little intellectual advance after age three. The features suggested autism or autistic spectrum disorder, with particular impairments in language and symbolic thought, but relative preservation of spatial skills, and compulsive pasting of sticky labels. He had no relevant family history.
From about age two and a half or three years of age (that is about four or five months after the birth of his sister), he began to “breath-hold”. He would pant (hyperventilate) and then stop breathing. The episodes evolved over months. He would stare, or stagger with garbled speech, or fall over, as often as several times an hour. Somehow, in the USA he had acquired a (temporary) diagnosis of late infantile neuronal ceroid lipofuscinosis. Cardiological studies demonstrated that his carotid blood flow ceased and his ECG amplitude halved during his compulsive Valsalva manœuvres. In his worst attacks, as in the video (patient 3), he would extend his upper limbs more than once, fall down and lie with vibrating limbs for up to one and a half minutes followed by disorientation for some 45 minutes.
His parents had found that episodes could be prevented if he were physically restrained (as by the wearing of a wrestler’s belt) from doing Valsalva’s. He was found to have a high plasma metencephalin level, and thereafter was started on the opioid antagonist naltrexone. This reduced episode frequency [20], but only for six months. Episodes continue at the age of 23 years.
Patient 4
This boy from Ayrshire Scotland presented, aged 15 months, with a history of “breath-holding spells” since the age of five months. Anoxic seizures would occur at least once daily, but from age 10 months epileptic seizures were provoked by the “breath-holding”, and by now the anoxic-epileptic seizures were occurring about twice a week. His “breath-holding spells” were not associated with changes in heart rate, but were episodes of pure, prolonged, expiratory apnoea, induced by any unpleasant stimulus or frustration. His parents had already filmed the “breath-holding” and the epileptic component at home, but did not manage to capture the transition between the syncope and the epileptic seizure. The film provided (patient 4) is a home video of the type of epileptic seizure that was very frequently induced. These epileptic seizures never occurred spontaneously. Sodium valproate prevented the epileptic component from manifesting (the family felt this was important once he began primary school), and anoxic-epileptic seizures did not occur after age six, despite “breath-holding spells” continuing up to eight years of age, uninfluenced by any therapy including expert psychological intervention.
His family history is of interest. His younger brother has had “breath-holding spells” and a febrile (epileptic) seizure. In his pedigree, there are individuals with “breath-holding spells” alone, early epileptic seizures alone, and both in the same individual.
Patient 5
This boy’s history has been previously reported in brief [6] (Case 11.6). He is the only one of the five children presented here to have epilepsy in the usual sense of repeated unprovoked epileptic seizures, first noted at age seven months. These were jerky episodes with variable impairment of consciousness and elevation of his upper limbs. The appearances suggested myoclonic absences (albeit slightly atypical) and the ictal EEG contained approximately 3/second spike wave (albeit somewhat ragged). There was a definite history of anoxic-epileptic seizures, in that several of his epileptic seizures were precipitated by syncopes in the form of “breath-holding”, possibly prolonged expiratory apnoea. His parents affirmed that the spontaneous epileptic seizure captured on home video (patient 5) looked the same as the epileptic seizures that were induced by “breath-holding”. Anoxic-epileptic seizures ceased before the age of three years, but his epilepsy has persisted beyond the age of 20 years with some associated developmental delay.
Discussion
That paroxysmal EEG discharges may be activated or induced by hypoxia has been known for over 40 years [21, 22]. We have previously published in this journal video-recordings of syncopes with pure anoxic seizures [19], but the existence of syncope-triggered epileptic seizures has been doubted by some, even within the last decade [23]. The author of that review of reflex anoxic seizures also wrote [23] “Occasionally, sudden pain may induce tonic-clonic seizures in patients with epileptic seizures, but this should be easy to recognise”. We have been unable to find evidence to support that contention. In stimulus-sensitive epilepsy such as startle epilepsy [24], it is the startle rather than the pain (if any pain is involved), that is the trigger.
The prime objective of the present publication is to demonstrate the existence of these anoxic-epileptic seizures in that “seeing is believing”. A separate paper will analyse the types of syncopes and epileptic seizures observed in a large number of children with anoxic-epileptic seizures seen at a single centre of paediatric neurology, including therapeutic options. Here, we are constrained by the limitations of what has been videotaped in the homes of affected families. If paediatricians, paediatric neurologists, adult neurologists, epileptologists and even cardiologists recognize the phenomenon illustrated, those afflicted must be better served. n
Acknowledgements
We thank the families for their cooperation and the provision of video material and Alastair Irwin Head of the Medical Illustration Department, Yorkhill Hospitals, Glasgow, for making the videos accessible.
|
|
|---|
| Patient 1 – Boy aged 18 months from Minnesota, USA
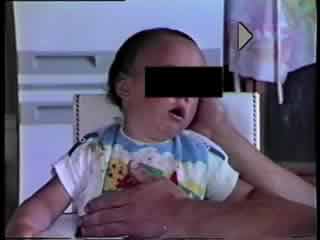
a. First home video of an anoxic-epileptic seizure, beginning at end of “breath-holding” with upper limbs extended followed by a twice repeated respiratory noise. Upper limbs are extended and adducted, followed by “uh-uh-uh”, deviation of his eyes to the left and extension/abduction of upper limbs. Semi-rhythmic jerks soon become evident in all four limbs. The trigger was “just a little bump”. Jerking involves the face, with continued deviation of eyes to the left, before waning of twitching movements and contra-lateral deviation of eyes to the right. Jerky phonation accompanies re-awakening. |
| Patient 2 – Girl aged 20 months from Fife, Scotland
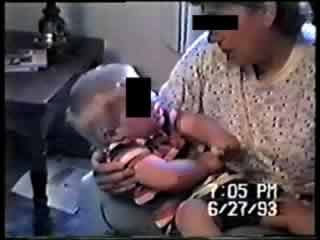
A respiratory noise precedes extension of her left upper limb, with wrists flexed and eyes open in a stare. Then twitching of her eyebrows begins with regular twitching of her limbs. Repetitive noises accompany continued twitching of eyebrows and upper limbs. Her eyes are probably deviated to the left. There is brief twitching of the left eyelids. Her eyes move to the midline as repetitive grunts continue. As the motor activity declines she becomes more quiet and her eyes deviate to the right and then open. |
| Patient 3 – Boy aged eight years from Boston, USA
He is standing behind a chair. Just beforehand his father has said to him “John, hold your breath”. John has his mouth open. “That’s how he starts”. He bends his trunk forwards and makes a respiratory noise. His upper limbs elevate abducted and extended. “There it is”. His elbows flex and he makes an “ooh” noise twice. Lying on the floor, his upper limbs are flexed and adducted across his chest. Snorty respiration with slurpy grunts accompany fast shaking of his upper limbs. Once the shaking has ceased he lies supine, unresponsive and with his eyes deviated to the right. He makes snorty inspirations and coughs. “He wet himself”. He chews. “Sometimes the seizures last a bit longer”. Finally he sits up. |
| Patient 4 – Boy aged 15 months from Ayrshire, Scotland
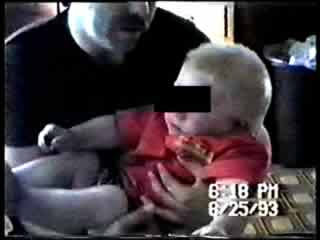
A “breath-holding spell” (prolonged expiratory apnoea) has induced this epileptic seizure that began before the camcorder could be switched on. He is supine on the floor, with semi-rhythmic twitching of four limbs and his eyes open. His mother tries to stimulate him by sound, by stroking his feet, and later by moving her fingers in his visual field. After a minute his eyes are deviated to the right. The film ends before he wakes up. |
| Patient 5 – Boy aged 15 months
He is sitting in his high-chair in the kitchen. In this 20s clip, his upper limbs are elevated and jerk rhythmically at a rate of about 3/second. At seven seconds into the film there is a reduction in the jerking and improved alertness with some rhythmic vocalization as if he is trying to speak. At 19 seconds the seizure ends. |






 Videotape captions
Videotape captions