Epileptic Disorders
MENUMight the olfactory bulb be an origin of olfactory auras in focal epilepsy? Volume 18, numéro 4, December 2016
“Stimulation results…we have never produced a sensation of smell from any region except the olfactory bulb and the uncus.” Wilder Penfield and Herbert Jasper (1954)
Olfactory auras or phantosmia are false perceptions of odours, usually unpleasant and unprovoked by ambient surroundings. They are epileptic phenomena associated with focal complex seizures of mesial temporal lobe origin. They occur as isolated phenomena, usually lasting seconds or a few minutes, or may be followed by motor activity or cognitive impairment as a component of more complex and sequential clinical events. Auras were known since the time of Pelops of Ancient Greece, master of Galen (130-210 A.D.). The word aura, meaning breeze, was introduced into medical terminology not by a physician or scientist, but by a patient of Galen who so described it (Temkin, 1945). Auras were described by Hughlings Jackson in the late 19th century as “the so-called warning” (Jackson, 1871; Jackson and Stewart, 1899). The term “uncinate fits”, applied in the early and mid-20th century (Daly, 1958), is now obsolete. The most recent (2010) proposal by the International League Against Epilepsy (ILAE) Commission on Classification and Terminology is that an aura corresponds to a focal seizure involving subjective sensory or psychic phenomena (Berg, 2010). Olfactory stimuli can provoke reflexive epilepsy in some patients (Llik and Pazarli, 2015).
Olfactory auras are the least frequent type of sensory aura, comprising a wide estimate of 0.9% to 16% of auras of all types (Lennox and Cobb, 1933; Acharya et al., 1998; Chen et al., 2003, 2007). They are associated with paroxysmal foci, as identified by pre-operative and intra-operative electographic recording in the mesial temporal lobe, and believed to arise in the entorhinal cortex (part of the parahippocampal gyrus), the amygdala, or the rostral insula. Olfactory auras occasionally co-exist with other sensory auras; mainly gustatory but also occasionally auditory, visual, and abdominal visceral (Penfield and Jasper, 1954; Palmini and Gloor, 1992; Fried et al., 1995; West and Doty, 1995; Acharya et al., 1998).
It is suggested that the olfactory system may modulate, but not initiate, epileptic discharges (Lin, 2015). The sensory spread or co-expression of auras of different types, including genetic disorders such as autosomal dominant partial epilepsy with both auditory and olfactory auras, neither supports nor refutes the hypothesis proposed here, on the basis of presently available data. In temporal lobe epilepsy associated with hippocampal sclerosis, olfactory auras are not prognostic for surgical outcome of mesial temporal lobectomy (Dupont et al., 2015). Olfactory impairment is found in patients with either left or right temporal lobe epilepsy, and is unrelated to the duration of epilepsy, frequency of seizures, and/or medications administered (Desai et al., 2015). Olfactory auras are difficult to confirm in infants and young children because they require verbal description, though they might be inferred by a facial grimace, wrinkling of the nose, or wiping the hand across the nose (Sarnat, 1978; Sarnat and Flores-Sarnat, 2016a).
Olfactory hallucinations also are reported in migraine but, unlike visual and other sensory auras, they are not included in the International Classification of Headache Disorders (Coleman et al., 2011; Hong et al., 2012; Ahmed et al., 2015). Whether olfactory auras in migraine differ from visual and other auras because of divergent neuroanatomical localization, and indeed their relation to epileptic olfactory auras, are unresolved issues.
Data are lacking from experimental animals or humans on whether the unique laminated cortical architecture of the olfactory bulb and its synaptic circuitry possess a potential for generating epileptiform activity and transmitting such discharges to other structures trans-synaptically. We reconsider a concept first suggested by Penfield and Jasper in their classic textbook (1954) based upon their report of smell detected by awake adult patients at craniotomy, induced by stimulation of the olfactory bulb, though they did not fully elaborate their observations as a hypothesis. Here, we propose that some olfactory auras arise primarily in the olfactory bulb and are only secondarily mediated by the amygdala, entorhinal cortex, or rostral insula. This hypothesis does not exclude that other olfactory auras may indeed arise primarily in olfactory areas of neocortex or amygdala.
Developmental neuroanatomy of the olfactory bulb
The olfactory bulb has unique architecture (figure 1), unlike that of any other laminated cortex of the brain (Crosby et al., 1962; Parent, 1996; Sarnat, 2016b), and its sequence of neuronal maturation and synaptic circuitry are equally unique and not yet mature at birth (Sarnat and Yu, 2016; Sarnat and Flores-Sarnat, 2017b). Complete maturation of the olfactory bulb is not necessary for initial function, though maturational progression in the olfactory threshold of neonates are observed (Lipsitt et al., 1963; Schaal et al., 2004; Marlier et al., 2007; Sarnat, 2017; Sarnat and Flores-Sarnat, 2017a). A diagram of the histological structure and microscopic and immunocytochemical illustrations of the olfactory bulb are provided in the on-line powerpoint supplement to this article. The targets of efferent olfactory projections from mitral and tufted neurons are mainly to its relay, the anterior olfactory nucleus, and are summarised in table 1.
The unique histological lamination of the olfactory bulb was well described in the late 19th century by numerous investigators, as recently reviewed by Sarnat and Yu (2016). The olfactory bulb was the first structure of the human brain to be defined by Golgi silver impregnations, in a paper by Camillo Golgi himself in 1875 (Golgi, 1875). During ontogenesis, none of its neurons arise from the primitive neural tissue of the olfactory bulb itself; neuroblasts stream into the olfactory bulb from the rostral telencephalon and then secondarily migrate radially, a migratory pathway known as the rostral migratory stream (Kishi et al., 1987; Rousselot et al., 1994; Lois et al., 1996). The migration is facilitated by a neuron-specific class III beta-tubulin (TUJ1) and a highly polysialated neural cell adhesion molecule (NCAM) (Lois et al., 1996).
Early neuroembryologists and neuroanatomists observed that the morphogenesis of the olfactory bulb is complete very early, compared with other telencephalic structures and, based on histogenesis, asserted that it was mature by 11 weeks of gestation (Humphrey, 1940). More recent studies using modern immunocytochemical markers of neuronal maturation demonstrate persistent immaturity of the human olfactory bulb in the term neonate, with regard to expression of specific neuronal maturational proteins, synaptogenesis, myelination, and postnatal involution of the olfactory ventricular recess from the lateral ventricle (Sarnat and Yu, 2016). The olfactory epithelium of the upper respiratory cavities also remains immature in the term neonate (Pyatkina, 1982). The olfactory tract is much more than a simple longitudinal bundle of axons. It includes as much grey as white matter. Granular neurons extend from the olfactory bulb at one end, and pyramidal neurons of the anterior olfactory nucleus from the other (Sarnat and Yu, 2016). The olfactory tract also includes processes of resident progenitor cells that persist into adult life.
Olfactory reflexes can be reliably tested clinically in the neonate, in premature infants, and in children (Lipsitt et al., 1963; Sarnat, 1978; Schaal et al., 2004; Marlier et al., 2007; Sarnat and Flores-Sarnat, 2017a). Odorous molecules in the amniotic fluid circulate through foetal nasal passages to activate receptors and produce behavioural responses even prenatally (Schaal et al., 1998, 2004). Cranial nerve 1 is only occasionally tested by neurological examination at any age, except in elderly patients with dementia who often have hyposmia or anosmia associated with tau deposition in the olfactory bulb. A few reports of dysplasias and other anomalies of the olfactory bulbs are published, such as in hemimegalencephaly (Robain et al., 1988; Sarnat and Yu, 2016), but documentation of malformations of the olfactory bulb is sparse because this structure is rarely examined microscopically at autopsy.
Neuropathological study of the olfactory bulb in humans can only be performed post-mortem, but reported autopsies of patients dying with seizures or SUDEP do not address this structure, in large part because the olfactory bulb rarely is taken for histological examination, and even when studied, rarely are immunocytochemical antibodies applied, hence data are sparse. Metabolic markers of epileptic foci, regardless of the presence or absence of a structural lesion, are becoming available. For example, the small heat shock protein α-B-crystallin often exhibits a gradient of reactivity that weakens in intensity 2-3 cm away from the cortical epileptic focus in surgical resections (Sarnat and Flores-Sarnat, 2009). Another example is hypermetabolic neurons with excessive mitochondrial enzymatic activity, seen histochemically in frozen sections of resected brain (Sarnat et al., 2011).
Potential sites of origin of olfactory auras
The entorhinal area is a neocortical region receiving afferent projections from the olfactory bulb itself and more extensively from its relay, the anterior olfactory nucleus (Crosby et al., 1962; Parent, 1996). The amygdala is another major recipient of many olfactory projections. It is proposed as the major site of origin of unpleasant, but also some pleasant, olfactory auras (Andy, 1967; Acharva et al., 1998; Chen et al., 2003; 2007; Rayport et al., 2006). The insula receives no direct axons from the olfactory bulb and relatively few afferents from the anterior olfactory nucleus, but it was suggested that pleasant auras of odours emanate from the insula (Ostrowsky et al., 2000). Functional mapping of the insular cortex by stereo-EEG reveals topographic organisation with a visceral network in the anterior part of the insula, from which emanates a network extending into mesial temporal structures. Hence, this part of the insula is most likely related to olfactory auras, particularly pleasant sensations (Ostrowsky et al., 2000). The orbitofrontal cortex also has been implicated as the site of origin (Bancaud, 1987). On the basis of functional MRI, other authors even localize pleasant odours to the right, and unpleasant odours to the left cerebral hemispheres, a lateralization of olfactory-activated temporal and anterior frontal cortices that is suppressed by narcoleptic medications (Henkin and Levy, 2001). Unilateral resection of the anterior mesial temporal lobe on either side in adults impairs odour identification (Juran et al., 2015).
In one study, olfactory auras arising in the amydala were more commonly due to tumour than to mesial temporal sclerosis (Acharya et al., 1998), but other studies showed the opposite predominance (Fried et al., 1995; Chen et al., 2003). Perven and So concluded that olfactory auras could arise anywhere within the complex olfactory network, but did not consider the olfactory bulb itself as a potential source of auras (Perven and So, 2015). There are no direct olfactory bulb axonal projections to the hippocampus without intermediate synapse, mainly in the anterior olfactory nucleus and amygdala (Acharya et al., 1998). The hippocampus would not likely be the origin of auras because the hippocampus does not project axons directly to neocortex to bring such perceptions to conscious awareness, though it is a repository of olfactory memory as with other memories. Multiple olfactory cortical areas transmit signals to hypothalamic neurons of corticotrophin-releasing hormone, which controls stress responses in animals to the odours of predators (Kondoh et al., 2016), but this circuit would not provide a basis for auras.
Olfactory bulbectomy in mice, by contrast, may lead to the development of epilepsy (Jiang et al., 2015); further evidence of a direct role of the olfactory bulb in epileptogenesis that, under some conditions, may suppress rather than enhance seizure discharges. Human data in this regard are lacking.
Development of the synaptic circuitry of the olfactory bulb
Axonal terminals of primary olfactory neurons pass through the thin bony cribriform plate to enter the ventral surface of the olfactory bulb, where they form synaptic glomeruli (glomerulus [Greek] = ball of threads) with dendrites of the layer of mitral and tufted cells. Despite the horizontal anatomical lamination of the olfactory bulb, its synaptic organization involves functional columns (Kauer and Cinelli, 1993; Willhite et al., 2006), similar to the barrels or columns of the neocortex (Rakic, 2000; Feldmeyer et al., 2013). Lateral synaptic connectivity within the olfactory bulb is much sparser (Kim et al., 2011).
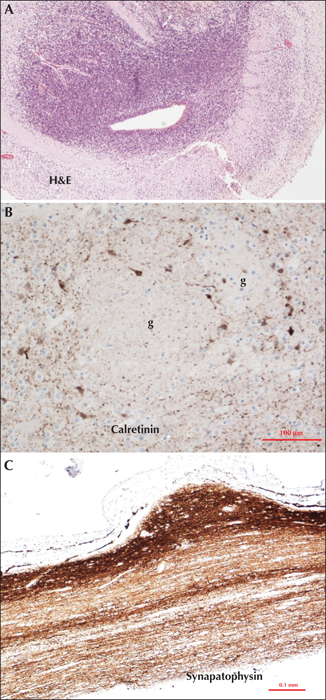
In tissue sections, antibody against synaptophysin can be applied as an immunoreaction. Synaptophysin is one of several important glycoproteins that are essential in the assembly and structure of synaptic vesicles in pre-synaptic axonal terminals, regardless of the nature of neurotransmitter they will contain, the site of the synapse (axo-somatic; axo-dendritic), or its function (excitatory or inhibitory) (Sarnat and Born, 1999; Sarnat, 2013, 2015). Synaptophysin is synthesized in the perinuclear region of the perikaryon and transported in the axon to its terminals. Other insoluble glycoproteins of the synaptic vesicle include synaptobrevin, synaptotagmin, and SNAP-25, in addition to several water-soluble synaptic proteins, such as synapsin 1 and 2, which are functional but not structural. A family of soluble calcium-binding proteins, which includes calretinin, parvalbumin, and calbindin D28k, serve as immunocytochemical markers for GABAergic inhibitory interneurons (Ulfig, 2002; Sarnat, 2013, 2015). Neuron-specific proteins can be applied to immature or dysplastic brain tissue as maturational markers, some expressed late in neuronal differentiation (e.g. NeuN; synaptophysin) and others expressed early in neuronal differentiation (e.g. MAP2; calretinin) (Sarnat et al., 1998; Ulfig, 2001; Sarnat, 2013, 2015).
Synaptic glomeruli exhibit less synaptophysin expression at 16 weeks than at older gestational ages; all are reactive by term. Calretinin, by contrast, is not yet expressed in most of the synaptic glomeruli at mid-gestation, but is strong in the primary olfactory nerve axons forming layer 1 (Sarnat and Yu, 2016). The later appearance of calretinin in synaptic glomeruli during foetal development implies that few primary axons have penetrated the glomerular parenchyma to establish synapses or that these axons have not established synaptic contact with mitral cell dendrites. Some neurons remain dormant for long periods before developing synaptic relations, even though pre-synaptic and post-synaptic membranes are in close proximity, a feature exemplified by primary olfactory receptor neurons in relation to mitral cells in the synaptic glomeruli of the olfactory bulb (Hinds and Hinds, 1976). The delayed expression of calretinin relative to synaptophysin in the olfactory glomeruli may be explained by this phenomenon.
Small periglomerular interneurons also occur, and often form sheet-like processes that envelop other small periglomerular neurons (Reese and Brightman, 1970). Spine-laden dendrites of periglomerular cells ramify within two or occasionally more glomeruli. Their axons extend across as many as six glomeruli as they contact local interneurons. These periglomerular neurons are heterogeneous in morphology, neurochemistry, and physiology; only 10% lack synapses with olfactory neurons (Kratskin and Belluzi, 2003). Periglomerular neurons synthesize and co-localize GABA and dopamine as neurotransmitters (Kosaka et al., 1985; Gall et al., 1987; Ohm et al., 1990, 1991). More than 20 known neurotransmitters or modulators are identified in the olfactory bulb (Hawkins and Doty, 2009).
The progressive concentric multiple lamination of the granular layer is well demonstrated by layers of granular neurons shown by NeuN, each layer separated by alternating layers of their dendro-dendritic synapses, shown by synaptophysin. This laminar maturation begins in the most peripheral part of the granular core; the deep core is the last to become laminated in the early postnatal period, but calretinin is expressed earlier in the granular layer when its neuroepithelial cells are still immature (Sarnat and Yu, 2016). At term, about 30-40% of granular neurons remain non-reactive to NeuN, mainly deep in the core. NeuN is a late marker of neuronal maturation expressed only when the neuron is nearly mature and functional (Sarnat, 2013, 2015).
Dendro-dendritic synapses are found sparsely throughout the neuraxis, except perhaps in the cerebral cortex, but are in greatest density of concentration in the olfactory bulb, where not only do they interconnect the GABAergic inhibitory neurons of the granular layer, but also form connections of granule cells with dendrites of the excitatory, glutamatergic mitral and tufted neurons (Kaba and Keverne, 1992; Hayashi, 1999, McTavish et al., 2012).
Synaptic circuitry in the murine olfactory bulb remains plastic not only in the immature neonatal condition but persists as long as the body is still growing (Pomeroy et al., 1990). Postnatally, the length of mitral cell dendritic branches increases by a factor of 11; the number of glomerular and extra-glomerular synapses increases by factors of 90 and 170, respectively (Hawkins and Doty, 2009). In addition, olfactory receptors in the mucosa have many de novo genetic mutations (Fleischer et al., 2009).
Myelination in the olfactory bulb and tract are entirely postnatal over several months (Sarnat and Yu, 2016). Primary olfactory nerve axons from the nasal mucosa undergo continuous turnover and never become myelinated.
Electrophysiological studies
Electrophysiological studies demonstrate that early olfactory deprivation greatly modifies and diminishes synaptic organisation of the olfactory bulb (Wilson et al., 1990). On the other hand, homotopically transplanted olfactory bulbs in neonatal rats after bulb removal are able to mature and re-establish relations with both the brain and the periphery (Zigova et al., 1990). Investigations of recording spontaneously generated electrical activity from the olfactory bulb are almost non-existent in humans and sparse even in animals, largely limited to a period of interest in rodents in the 1980s. As noted earlier, classical studies by Penfield and Jasper of electrical stimulation of the human olfactory bulb of awake patients intra-operatively, showed that olfactory perception was generated in the absence of odours (Penfield and Jasper, 1954).
Animal studies
The rodent brain should be a good model for the study of electrical potentials in the olfactory bulb, not only because this structure is relatively large in relation to the forebrain in rodents, but because the intrinsic synaptic organisation of the olfactory bulb is similar in all mammals, including humans. A few differences do occur between mammals and non-mammalian vertebrates, for example, mitral cells usually contact several olfactory glomeruli in the latter, but project only to one glomerulus in mammals, as shown by ultrastructural studies (Turner and Singer, 1974). Whether a propensity for generating epileptic potentials is the same in rodent and human olfactory bulbs, is unknown.
Synapatic factors conducive to epileptogenesis
All structures of the mature nervous system can be divided into those that are synaptically stable and those that are synaptically plastic. Synaptic stability means that there are few and seldom changes in the interneuronal connections, whereas synaptic plasticity implies continuous dendritic remodelling, pruning, or retraction of old synapses and formation of new ones. Synaptically stable regions of the central nervous system include the spinal cord, brainstem nuclei, cerebellum, basal ganglia, and thalamus; none of these structures are epileptogenic. Synaptically plastic regions of the brain include the hippocampus; amygdala; much of the neocortex, particularly associative zones and the temporal lobe; and subcortical white matter neurons and their synaptic plexi (i.e. networks) associated with focal cortical dysplasias; all are highly epileptogenic zones (table 2). The mature retina was previously believed to be a synaptically stable structure, but recent evidence indicates that it also exhibits considerable plasticity (Schmidt et al., 2011; Baden et al., 2016), though not epileptogenic.
The olfactory bulb exhibits a precise number of synapses per type of neuron and preserves a ratio of neurons of each type. Each glomerulus receives as many as 25,000 axons of olfactory nerve neurons; the convergence of about 1,000 receptor cell axons upon every second-order neuron (rabbit) results in major summation or amplification of olfactory stimuli (Liem et al., 2001). About 80% of synaptic contacts between neurons are organised as reciprocal pairs; mitral-to-granule cell synapses are excitatory, in contrast to granule cell-to-mitral neuronal synapses which are inhibitory (Kosaka et al., 1985). This mathematical precision is reminiscent of two other structures of the brain with predictable ratios of neuronal types and their connections; the cerebellar cortex which is not epileptogenic and the hippocampus which is highly epileptogenic.
The hippocampus must be plastic to enable the formation of new memory engrams and to facilitate deletion of others of no permanent importance (Moser et al., 1994; Engert and Bornhoeffer, 1999; Sanders et al., 2012; Yang et al., 2014; Attardo et al., 2015; Ryan et al., 2015), whereas stability of hippocampal dendritic spines is associated with the conservation of long-term memories (Yang et al., 2009).
The amygdala, associated with emotions, fear, anxiety, and other psychological phenomena is another region of great synaptic plasticity throughout life and may be influenced by hormones, DNA methylation by alcohol, hypoxia, neurotoxins, and other exogenous factors (Arruda-Carvalho and Clem, 2014; Alisch et al., 2014; Kuhn et al., 2014; Li and Rainnie, 2014; Marin, 2014; Boitard et al., 2015; Dall’Oglio et al., 2015; Galvin et al., 2015; Kim et al., 2015; Stolyarova and Izquierdo, 2015).
The olfactory bulb is another of the most synaptically plastic structures of the brain (Pomeroy et al., 1990; Mouly and Sullivan, 2010), yet its epileptogenic potential is unknown because this aspect has been little investigated or even considered in animals or humans. Primary olfactory neurons, the somata of which lie in the nasal epithelium, are continuously lost and replaced by an active regenerative process; their unmyelinated axons extend through the cribriform plate into the synaptic glomeruli of the olfactory bulb, and are thus also in continuous turnover. Considerable intrinsic synaptic remodelling and plasticity are demonstrated throughout the olfactory bulb itself.
The amygdala is often the site of epileptic activity arising in the mesial temporal lobe; the amygdala may be altered histopathologically and this often accompanies hippocampal sclerosis (Yilmazer-Hanke et al., 2000; Blümcke et al., 2015). The amygdala has also been reported to demonstrate paroxysmal activity based on intra-operative electrocortical surface and depth recordings. The amygdala is the origin of many odour-driven appetitive and adversive behaviours that are not epileptic in nature (Root et al., 2014), mediating the large afferent input from the olfactory bulb directly and through intermediate relay via the anterior olfactory nucleus. Olfactory auras can be caused by focal amygdaloid networks without widespread projection, as demonstrated by depth electrodes in a patient with haemorrhage from a cavernous angioma in the mesial temporal lobe; the olfactory auras were successfully abolished by surgical amygdaloid resection (Hamasaki et al., 2014). However, this case does not necessarily signify that all olfactory auras originate in the amygdala.
The olfactory bulb and the hippocampus are the two most important repositories of abundant progenitor stem cells available for neuronal differentiation, not only in foetal but in adult life as well. This generation of progenitor cells that can differentiate as new neurons not only contributes to synaptic plasticity, but may be an additional factor rendering the hippocampus and possibly the olfactory bulb capable of generating paroxysmal activity. In the case of the olfactory bulb, such electrophysiological phenomena could be perceived as olfactory auras.
Though the cerebellum is a synaptically stable non-epileptogenic structure of the brain, it may suppress epileptic activity in the cerebral cortex. The rostral cerebellar projection is mainly from the dentate nucleus to the contralateral ventrolateral thalamic nucleus, the pathway crossing the midline in the caudal midbrain as the brachium conjunctivum. This cerebellar ouput is inhibitory. Experimental dentate nuclear stimulation in a mutant mouse with absence seizures suppresses this epilepsy by impeding oscillatory activity in thalamic nuclei (Eelkman Rooda, 2015). In the 1970s, electrical stimulators were implanted in the cerebellum of selected patients with refractory epilepsy and indeed had some success, but this approach had to be abandoned because chronic use resulted in irreversible cerebellar degeneration.
“Cerebellar epilepsies” have been suggested over many years (Webster and Weinberger, 1940; Harvey et al., 1996; Arzimanoglou et al., 1999; Hanai et al., 2010; Foit et al., 2016), based on case reports of ganglioglioma, an epileptogenic tumour of the cerebral cortex (Blümcke et al., 2015) that occasionally involves the cerebellum. Hemifacial seizures are the clinical correlate. However, the more frequent cerebellar neoplasms, such as astrocytoma and medulloblastoma, do not produce epilepsy and even extensive cerebellar malformations generally are not epileptogenic unless associated with forebrain dysgenesis (e.g. lissencephaly 2 and Walker-Warburg syndrome; ARX phenotypes). Rare cases of cerebellar dysgenesis in patients with epilepsy have been described, however (Lascano et al., 2013). The infrequent cerebellar ganglioglioma merits further consideration, but present evidence does not refute the concept that the cerebellum is synaptically stable with low epileptogenic potential. An association of tumours of the temporal lobe with olfactory auras, by contrast, has been recognised for more than a century (Mills, 1908).
Olfactory thalamic equivalent
All sensory systems with neocortical perception project first to the thalamus, except one, the olfactory. The reason that perception and discrimination of odours in the cortex do not need thalamic relay is that the olfactory bulb and tract incorporate their own intrinsic thalamic equivalent (figure 2). Three neuronal components comprise this olfactory thalamus neuroanatomically: axonless granular and periglomerular neurons and the anterior olfactory nucleus. Granular neurons form the core of the olfactory bulb initially as neuroepithial cells that mature as neurons, with some remaining undifferentiated as progenitor cells. Granular neurons extend caudally from the olfactory bulb into the distal end of the olfactory tract. Synaptic connections of granular and periglomerular neurons are entirely intrinsic, whereas the anterior olfactory nucleus receives afferents from the olfactory bulb and its efferent connections to the amygdala and entorhinal cortex are analogous to thalamocortical projections of other sensory systems. The anterior nucleus is really a group of neuronal aggregates at the proximal end of the olfactory tract with some nodules within the olfactory tract. Some authors feel that the name anterior olfactory nucleus is incorrect and redesignate it the retrobulbar region (Paxinos and Mai, 2004). The larger portions behind the olfactory tract have a loosely organised laminar architecture resembling a cortex, perhaps analogous to the layered lateral geniculate body of the thalamus that subserves the visual system.
Despite a projection from entorhinal cortex to the mesiodorsal thalamic nucleus for relay to the posterior orbital agranular insular cortex, the projection of olfactory cortex to the same orbital/insular area involves a series of many neurons. This thalamic projection, therefore, is not essential (Barbado, 2002).
In granular and periglomerular neurons, calretinin is strongly immunoreactive, indicating GABAergic inhibitory neurons, similar to many intrinsic neurons of the thalamus. Neurons of the anterior olfactory nucleus are not calretinin-reactive, by contrast (Sarnat and Yu, 2016), but rather are glutamatergic or monoaminergic, as with thalamo-cortical neurons. More than 20 neurotransmitters and neuromodulators have been identified in the mammalian olfactory bulb (Hawkins and Doty, 2009). Some epilepsies, formerly classified as “generalized”, were believed to possibly arise in the thalamus, but it is now demonstrated that the paroxysmal activity actually originates in the cerebral cortex. Generalized epilepsies are now regarded as “network disorders” with cortical and thalamic interactions highly integrated. The same is likely true in the olfactory bulb and its thalamic equivalent.
Approaches to testing the hypothesis
The rodent serves as a common experimental model for epilepsy, based on both the use of inducing paragenetic factors as well as genetic strains of epileptic mice. The olfactory bulb is relatively large in rodents, as a ratio of the entire telencephalic volume, rostral to the rest of the cerebrum rather than beneath it, and thus should be amenable to direct electrophysiological monitoring with subdural or depth electrodes. Attempts to induce epileptogenic foci in the olfactory bulb might also be made, as already achieved in the cerebral cortex. Rodents, of course, cannot describe olfactory auras.
In humans, EEG recording from the olfactory bulb is more difficult and invasive, though invasive depth recordings from hippocampus, amygdala, and neocortex are performed. Olfactory hallucinations were elicited by direct electrical stimulation of the olfactory bulb and tract via subdural electrodes, but not from stimulation of olfactory neocortex alone (Kumar et al., 2012), confirming the earlier observation of Penfield and Jasper (1954). Whether it is possible to perform a localized recording from the olfactory bulb using appropriately placed intranasal electrodes during CT or MRI merits investigation. If confirmed, this method could be used in patients with focal epilepsy who manifest olfactory auras. For patients who have suffered olfactory auras during life and who have died for some other reason, careful neuropathological examination of the olfactory bulbs and related structures might yield additional clues.
Supplementary data
Summary didactic slides are available on the www.epilepticdisorders.com website.
Disclosures
None of the authors have any conflict of interest to declare.
* Presented at the 31st International Epilepsy Congress (International League Against Epilepsy, ILAE), Istanbul, Turkey, 5-9 September 2015.