Epileptic Disorders
MENUEffective posterior extension of callosotomy by gamma knife surgery Volume 22, numéro 3, June 2020
- Mots-clés : epilepsy, drop attacks, callosotomy, step-wise, gamma knife, radiosurgery, minimally invasive
- DOI : 10.1684/epd.2020.1170
- Page(s) : 342-8
- Année de parution : 2020
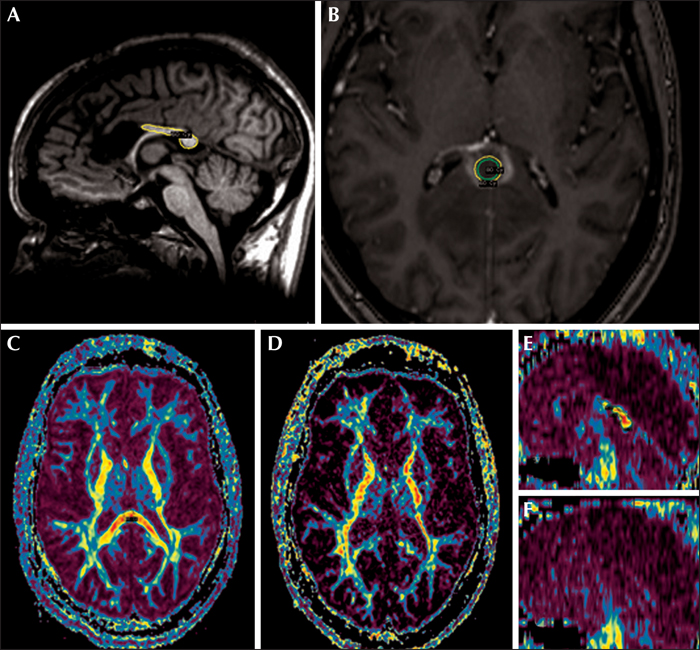
Drop attacks are the most responsive seizure type to open callosotomy, however, surgical complications can worsen the prognosis. Various less invasive techniques have been explored in an effort to minimize the risk. We present a patient who suffered from life-threatening traumatizing drop attacks in whom previous open anterior callosotomy and vagal nerve stimulation were unsatisfactory. Following posterior extension of the callosotomy by non-invasive gamma knife surgery, the rate of drop attacks declined from 30 a day to once a day, or every few days over a four-month period, without complications.
Open callosotomy is an invasive and high risk treatment option for patients with drop attacks. The procedure has a potential for complications and neurological consequences that can worsen the functional capacity of a patient who already suffers with disability. Recently, in an attempt to decrease the invasiveness associated with this technique, additional technical refinements and less invasive procedures have been explored in a few studies.
Here, we report a case of refractory epilepsy with life-threatening traumatizing DA, in which the patient was treated by radiosurgical posterior callosotomy after unsatisfactory open anterior callosotomy and vagal nerve stimulation.