Epileptic Disorders
MENUAbsence status induced by lacosamide adjunctive therapy Volume 21, numéro 1, February 2019
- Mots-clés : lacosamide, absence status, idiopathic generalized epilepsy, antiepileptic medications, seizure aggravation
- DOI : 10.1684/epd.2019.1032
- Page(s) : 97-101
- Année de parution : 2019
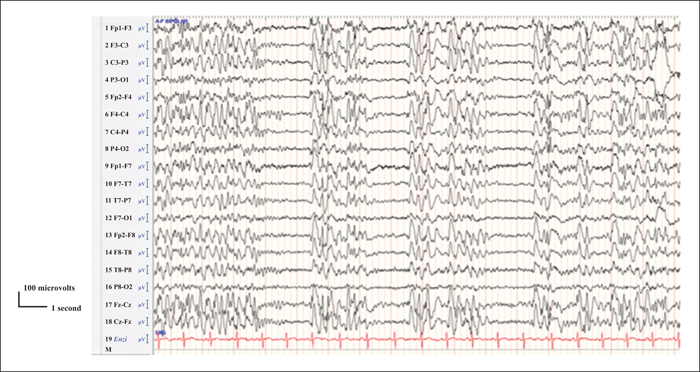
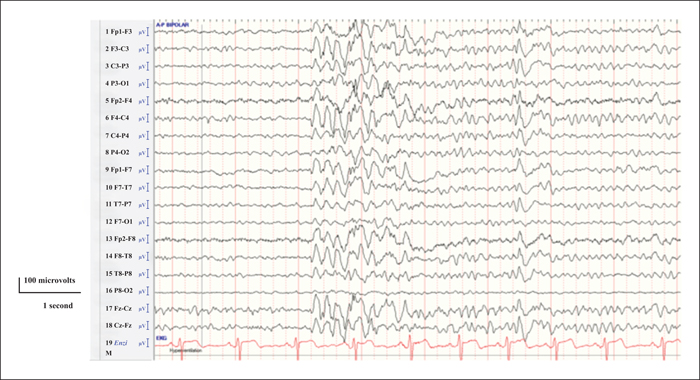
Since lacosamide was approved as an adjuvant agent for the treatment of medically refractory focal epilepsy over ten years ago, it is becoming more widely used for the treatment of idiopathic (genetic) generalized epilepsies. Several studies have demonstrated efficacy in reducing primary generalized tonic-clonic seizures (GTCS), but efficacy is less well-characterized for myoclonic and absence seizures. A 29-year-old man with juvenile myoclonic epilepsy and medically refractory GTCS on a combination of levetiracetam and topiramate was started on lacosamide adjunctive therapy with the plan to replace topiramate. While his GTCS became controlled, he was witnessed to have confusional episodes, with waxing and waning responsiveness, lasting a few days, several times a month. After eight months of adjunctive lacosamide therapy, he was admitted to the epilepsy monitoring unit, where paroxysms of generalized spike-and-wave complexes, lasting for 30-90 minutes, were recorded, interrupted only by sleep. During these periods, he demonstrated psychomotor slowing and disorientation on examination. The absence status was successfully broken by lorazepam, and lacosamide was discontinued. The patient had no further confusional episodes at the most recent follow-up visit, four months after discharge.