Epileptic Disorders
MENUPaediatric epilepsy surgery in the posterior cortex: a study of 62 cases Volume 16, numéro 2, June 2014
- Mots-clés : occipital epilepsy, parietal epilepsy, epilepsy surgery, extratemporal epilepsy, children
- DOI : 10.1684/epd.2014.0648
- Page(s) : 141-73
- Année de parution : 2014
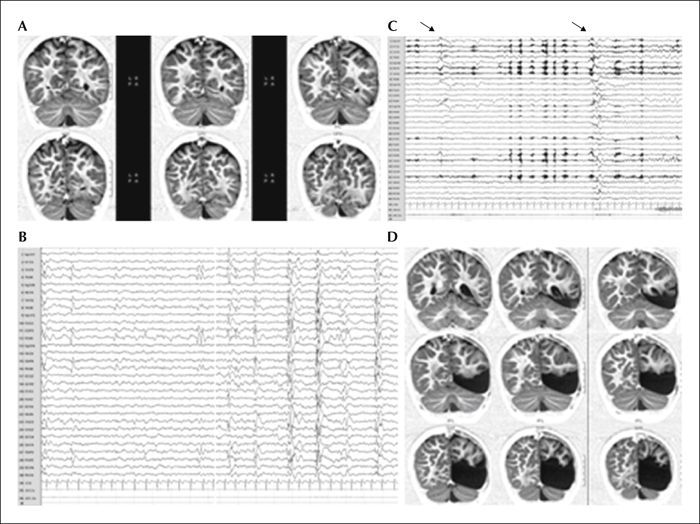
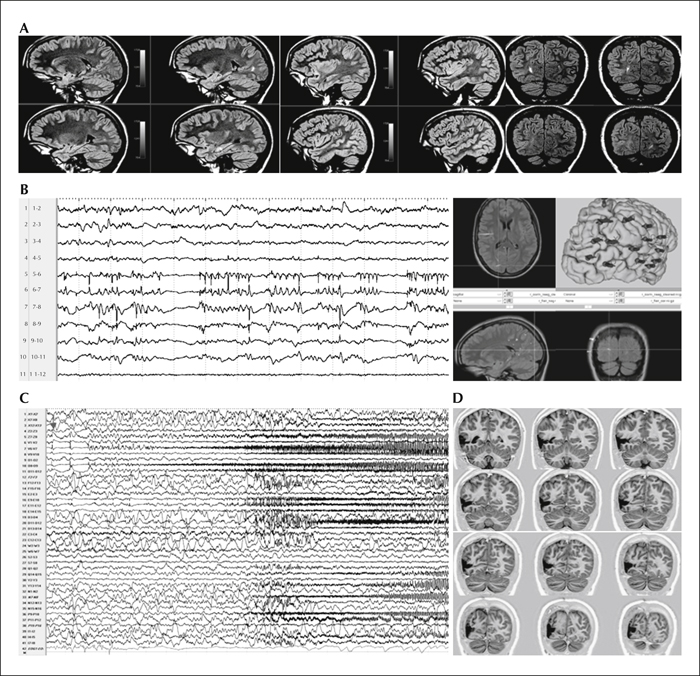
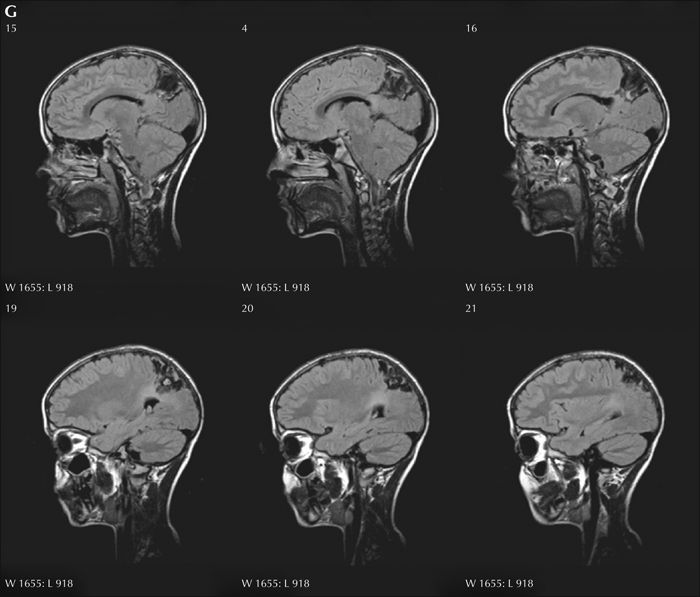
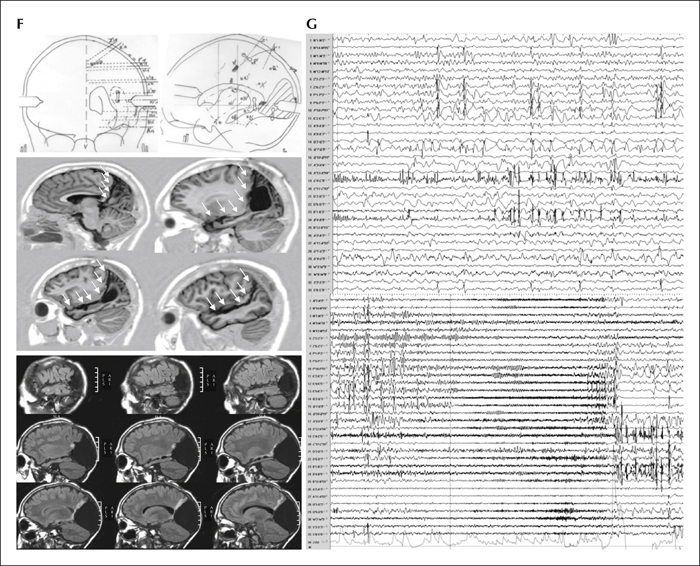
Past surgical series have emphasized the diagnostic complexity of posterior cortex epilepsy. Available data are sparse, especially in children, and most published series report a high number of surgical failures and post-operative neurological deficits. In this article, we present a paediatric cohort of 62 children who underwent surgery for drug resistant posterior cortex epilepsy before the age of 16 years with a mean post-operative follow-up of 6.94 years (range: 2-16). Mean age at epilepsy onset was 3.2 years and 28 children (45%) had onset before 1 year of age. The mean age at surgery was 7.9 years (range: 1-16). Daily seizures were present in 63% of children. MRI was positive in 58 cases (93.5%) and invasive stereo-EEG was judged mandatory in 24/62 (39%) of patients.
Surgery was confined to the parietal lobe in 11 children, the occipital lobe in 8, the occipito-parietal region in four, the occipito-temporal region in 18, and involved both the temporal and parietal lobes in the remaining 21. Following surgery, 53 subjects (85.5%) remained seizure-free and among those who underwent a SEEG procedure, 75% achieved seizure freedom. Focal cortical dysplasia was the most frequent histopathological diagnosis (50%), followed by tumoural (24%) and gliotic lesions (14.5%).
An older age at epilepsy onset, the presence of a rather restricted epileptogenic area, and a complete resection of the epileptogenic zone were predictive of a favourable surgical outcome. These results demonstrate that a good surgical outcome is possible in children with drug resistant posterior cortex epilepsy. Accurate analysis of the chronology of ictal semiology and electrophysiological features, viewed in the context of the complete electroclinical pattern, provides a topographical orientation for posterior cortex epilepsy and, together with the presence of a lesion detectable on imaging, may improve the rate of surgical success of posterior cortex epilepsy at paediatric age.