Epileptic Disorders
MENUIntraoperative electrocorticography-guided microsurgical management for patients with onset of supratentorial neoplasms manifesting as epilepsy: a review of 65 cases Volume 16, numéro 2, June 2014
- Mots-clés : electrocorticography, epilepsy, microsurgery, neoplasm, epileptogenic focus
- DOI : 10.1684/epd.2014.0662
- Page(s) : 175-84
- Année de parution : 2014
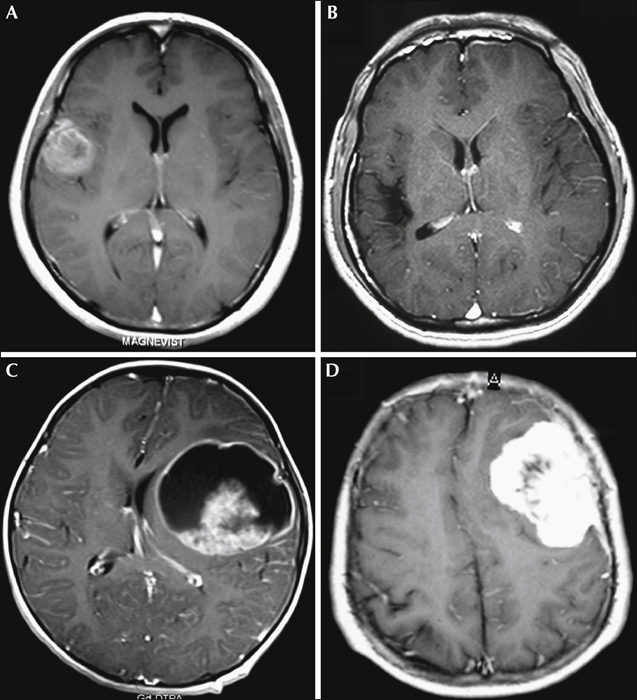
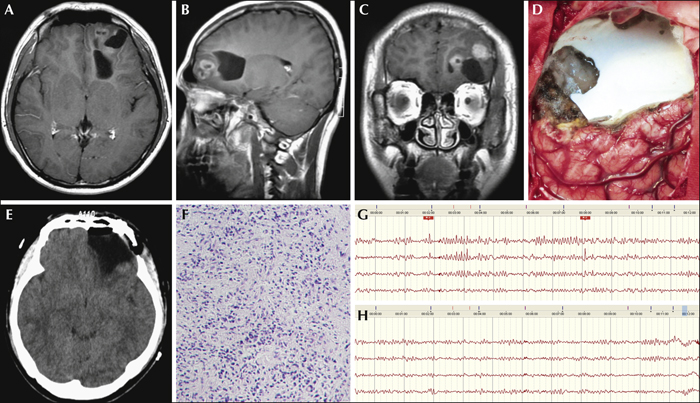
Aim. We reviewed the surgical procedures guided by intraoperative electrocorticography and outcome of 65 patients with onset of supratentorial neoplasms manifesting as epilepsy. Method. Clinical data were obtained for 65 patients with supratentorial neoplasms who received surgery, with the aid of intraoperative electrocorticography to screen epileptogenic foci before and after removal of neoplasms, and depth electrodes when needed. According to electrocorticography findings, appropriate surgical procedures were performed to treat the epileptogenic foci. In the control group, 72 patients received simple lesionectomy. Postoperative seizure outcomes were documented and analysed retrospectively. Results. In the case group, 33 patients received lesionectomy only, while the other 32 patients underwent intraoperative electrocorticography-guided tailored epilepsy surgery. In total, 57 patients (87.7%) in the case group and 38 patients (52.8%) in the control group were seizure-free (Engel Class I). Comparing outcomes of patients with temporal lesions between the two groups, 80.0% patients (12/15) in the case group and 20.0% (3/15) in the control group were seizure-free. Furthermore, comparing the seizure outcomes of patients who finally underwent tailored epilepsy surgery and simple lesionectomy (33 after electrocorticography and 72 without electrocorticography), intraoperative electrocorticography-guided tailored epilepsy surgery demonstrated superiority over lesionectomy (Engel Class I; 87.5% vs. 63.8%, respectively). Conclusions. Electrocorticography plays an important role in the localisation of epileptogenic foci and evaluation of the effects of microsurgical procedures intraoperatively. Isolated lesionectomy is not usually sufficient for better postoperative seizure outcome. In addition, for patients with temporal tumours, especially in the non-dominant hemisphere, a more aggressive strategy, such as an anterior temporal lobectomy, is recommended.