Epileptic Disorders
MENUEpilepsy in adults with neurodevelopmental disability - what every neurologist should know Volume 24, numéro 1, February 2022
This seminar covers the Level 3 Learning Objective 6.1.4 of the International League Against Epilepsy (ILAE) Curriculum: Demonstrate the ability to recognize and manage the special needs of persons with epilepsy (and neurodevelopmental disorders [NDDs]) [1].
Epilepsy in association with comorbid neurodevelopmental disorders requires specific consideration with regards to assessment, treatment, and service provision. This paper will consider the evidence for approaching epilepsy care in these complex populations as a constituent of a global neurodevelopmental picture, as opposed to a discrete condition, and provide good practice evidence-based insights for the practicing clinical neurologist in managing epilepsy in people with neurodevelopmental disability. Details regarding the specific diagnosis and management of epileptic encephalopathies, most of which lead to neurodevelopmental disorders, are outside the scope of this manuscript.
The ILAE clinical definition of epilepsy includes considering a diagnosis for individuals with one unprovoked seizure when the risk of recurrence is more than 60% [2]. In this context, it is interesting to start to consider the presence of an NDD as a potential significant risk factor. For example, the prevalence of epilepsy in a pooled sample of people with intellectual disability (ID) has been estimated at 22.2% [3]. In comparison, the point prevalence of epilepsy in the general population has been consistently identified at approximately 0.6% (6.38 per 1,000 persons [95% CI: 5.57-7.30]) [4]. Epilepsy is not only more common among those with ID, but is also more challenging to treat, with over two thirds of people with epilepsy and ID identified as treatment resistant, necessitating polypharmacy [5].
Diagnostic criteria and epidemiology
The Diagnostic and Statistical Manual of Mental Disorders fifth edition (DSM5) refers to an NDD as a condition with childhood emergence (in the developmental period), with characteristic deficits in core domains of language, cognition, social skills, and motor function [6]. NDDs primarily include intellectual disability (ID), autism spectrum disorder (ASD), and attention deficit hyperactivity disorder (ADHD), among other specific communication/learning and motor disorders. This report will exemplify the strong correlation between epilepsy and the classified NDDs discussed [7].
Intellectual disability (ID)
The DSM 5 defines ID as comprising of deficits in both cognitive and adaptive function across conceptual, social, and practical domains. The level of ID can be categorised based upon impact on the individual, from mild to profound, and the population is heterogeneous as a result of the wide diagnostic criteria. Therefore, this must be considered when interpreting any cohort of people with ID included in clinical trials. An Intelligence Quotient (IQ) test may form part of the assessment process and a score of two standard deviations below the average is considered a cognitive deficit. However, even standardised, culturally appropriate IQ tests have limitations and a diagnosis should not be made based on the test alone but in the context of other aspects of cognitive abilities and adaptive functioning. These deficits must be present in the developmental period [6].
A meta-analysis of population-based studies indicates that the prevalence of ID in the general population is approximately 1% (10.37/1000 [95% CI: 9.55-11.18]) [8]. Among people with ID, the epilepsy prevalence rate varies between 14 and 44% dependent upon the population sample [9-12]. The prevalence of epilepsy increases with the severity of ID, with a prevalence of 10% in mild ID, increasing to 30% to 50% in moderate to profound ID [3]. Conversely, people with ID make up approximately one quarter of the epilepsy population [13].
Autism spectrum disorder (ASD)
The definition and diagnostic criteria for ASD have evolved and broadened over time. However, the core features of impairment in reciprocal social interaction, communication, and repetitive/stereotyped behaviours remain consistent within the DSM5 classification [6].
A report by the Centre for Disease Control and Prevention (CDC) in the United States (US) reports an autism prevalence of 1 in 54 children [14]. There is also an association with other NDDs and the prevalence of ASD in individuals with ID is approximately 18 times higher than that in the general population [15]. There are two peaks in the incidence of epilepsy in patients with autism; in the early years and then unusually in the teenage years. The lifetime prevalence of epilepsy in ASD has been observed at 30% [16]. A pooled data analysis (n=2112) has demonstrated that the point prevalence of epilepsy in ASD with comorbid ID is far higher than in ASD alone (21.5% vs 8%) [17]. ASD features may also be a constituent part of a genetic syndrome phenotype such as Rett syndrome [18].
A retrospective follow-up study of 130 individuals with ASD identified 33 (25%) individuals who developed seizures [19]. The majority (61%) presented with focal seizures, and over two thirds (68%) of the group with epilepsy were found to have epileptiform changes on electroencephalogram (EEG) before the onset of epilepsy. The onset of epilepsy in this cohort was between the ages of eight and 26 years of age. A population-based cohort study (n=64,188) found the odds ratio for ASD among people with epilepsy at 22.2 (95% CI: 16.8-29.3) [20]. There may be underlying common pathophysiological mechanisms that predispose to the development of both ASD and epilepsy. Sometimes, the underlying condition is obvious, for example, tuberous sclerosis complex, but often it is not [21].
Attention deficit hyperactivity disorder (ADHD)
The DSM5 criteria for ADHD states that a diagnosis may be made in the presence of five or more symptoms of inattention and/or five or more symptoms of hyperactivity/impulsivity inconsistent with developmental level with negative impact upon functioning across a number of domains. These symptoms must persist for six months or longer [6].
A large systematic review and meta-analysis has found that the pooled worldwide prevalence of ADHD is an estimated 5.29% (95% CI: 5.01-5.56) [22]. The prevalence of ADHD in children with epilepsy may be between 31 and 65% dependent upon population sample [23, 24]. The relative risk of epilepsy in children with ADHD is more than double that of those without [25]. ADHD is more likely to be associated with a history of febrile seizures, frontal lobe epilepsy, and abnormal inter-ictal EEG findings [26]. However, there are no clear data available on whether there is any temporal relationship between epilepsy and ADHD [27].
An epidemiological survey of adults with active epilepsy (n=1,361) found that almost one in five (n=251) self-reported symptoms are consistent with ADHD [28]. This result was replicated in a cross-sectional study of 200 adults with epilepsy without ID, which revealed that 70 participants had a positive ADHD screen. It must be noted that the presence of symptoms is not diagnostic without the impact upon functioning using commonly recognised criteria such as the DSM5 classification [29].
Epilepsy-NDD conundrum
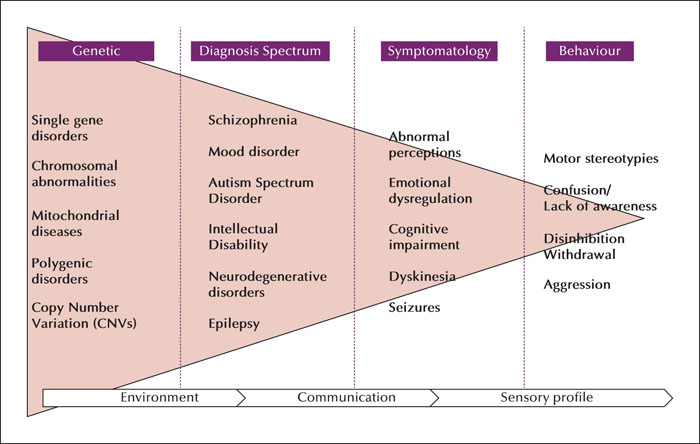
The epidemiological evidence supports the argument that epilepsy and associated NDDs and neurological deficits may be influenced by the same or related causative mechanism (figure 1). The aetiology may be unique to that individual and may be influenced by genetic predisposition and/or structural abnormalities. A follow-up study in a specialist epilepsy centre (n=98) of 6-13-year-olds with active epilepsy demonstrates the strong relationship between autism, ADHD, moderate-to-profound ID, and cerebral palsy, present together in over two thirds of the children studied [30]. A review of neurobehavioral comorbidities in children with active epilepsy (n=85) also found that the majority had a diagnosable neurodevelopmental disorder- ID (40%), autism (21%), and ADHD (33%) [31]. Considering ASD specifically, a systematic review and meta-analysis has found that individuals with ASD are more likely to have a wide range of neurological co-morbidities (migraine, macrocephaly, hydrocephalus, CP) including epilepsy (11.3-17.2%) [32].
People with epilepsy and NDDs are a heterogeneous population. There are known single gene disorders, rare epilepsy syndromes, and established disease genes that are associated with the susceptibility for both epilepsy and neurodevelopmental disorders. Genetic epilepsies and epileptic encephalopathies are not currently included within the DSM5 classification of NDDs. However, the evidence demonstrates that the relationships between them should be considered closely. The advances in diagnostics imply that a retrospective diagnosis of a genetic aetiology is now often possible in cases where none have been identified previously. Considering the impact of epilepsy as part of the global NDD picture will help in the move towards individualising care and optimising outcomes. This could be a step away from condition-based treatment to person-centred care where specialists and services for NDDs and epilepsy need to work collaboratively [7].
Co-morbidities associated with epilepsy and NDDs
Physical
ID
People with ID and epilepsy have more physical co-morbidities than those with ID without epilepsy, which results in higher health costs and increased mortality rates [33]. People with ID in general are significantly more likely to suffer with multi-morbidity (two or more long-term conditions) than the general population. A population-based cross-sectional study (n=1,424,378) investigating 32 physical and six mental health conditions found that people with ID have a significantly higher burden of co-morbid conditions at a far earlier stage of life, irrespective of major environmental factors [34]. At the observed point in time, 14 physical health conditions were more prevalent in people with ID. Aside from epilepsy (18.8%), the most common co-morbid physical health conditions included constipation in 14% (OR=11.19; 95% CI: 10.97-12.86) and visual impairment in 3.2% (OR=7.81, 95% CI: 6.86-8.89). Hearing impairment (8.2%), gastroesophageal reflux (10.3%), and thyroid disorders (7.9%) were also more common. A large population-based review across the lifespan indicates multi-morbidity rates of 98.7% in people with ID [35]. People with ID also have higher rates of dysphagia (8.1-11.5%), with the point prevalence increasing with severity of ID, presence of CP, and age [36].
ASD
A population study (n=6649) in Scotland based on census data found that more than one in five adults over 25 years with ASD had a physical disability, and with high levels of hearing (13%) and visual (12.7%) problems. Thirty percent of this population also had ID [37]. Results from the UTAH ASD epidemiological study (n=92) identified a significant burden of medical co-morbidities (62% with ID). More than half (59%) were known to have gastrointestinal problems, most commonly constipation (36%). The neurological burden was also high (54%), and 57% had ear, nose and throat problems (ear infections, tooth decay, hearing loss). Other common co-morbidities included sleep disturbance (41%), urological problems (40%), cardiovascular disease (35%), skin conditions (36%) and musculoskeletal concerns (36%) [38]. A large-scale study in the United States of adults with ASD (n=1507) and matched controls found that most major medical conditions across a range of organ systems were significantly more common in the ASD population [39]. These conditions included GI disorders (34.7%), sleep disorders (17.6%), dyslipidaemia (22.8%), hypertension (25.6%), diabetes (7.6%), obesity (33.9%) and thyroid disorders (7.0%). Within the ASD cohort, nearly a fifth (19.7%) had ID.
A nationwide study of children (5-14 years) in Germany with ADHD (n=258,662) investigated the presence of a wide range of co-morbid medical conditions. In this population, the majority (86%) had at least one identified comorbid disease, compared to 40% in the general population. On average, children with ADHD had four co-morbid conditions. Excluding mental and behavioural disorders, the most common co-morbidities included diseases of the respiratory (30%), visual (16%), and endocrine system (12%) and skin (12%) [40].
Psychiatric
ID
The lifetime risk of psychiatric disorders in people with ID appears to be considerably higher than in people without ID [41]. The standardised odds ratio for a serious mental illness such as psychosis in a community sample has been observed at 7.16 (95% CI: 6.49-7.89) for people with ID. In the same sample, the prevalence of depression (15.8%), anxiety disorders (8.1%), and dementia was also significantly higher than in the general population [34]. A study of adults with ID attending a tertiary epilepsy centre (n=189) found high levels of anxiety (12.7%) and depressive symptoms (21.7%). This investigation also identified a significant correlation between seizure frequency and negative psychological functioning [42]. Furthermore, in people with ID and active epilepsy, the risk of mental illness was reported to be seven times higher over a 12-month period when compared to those with ID alone [43]. In comparison, in people with epilepsy without ID, the risk of active depression is around three times that of the general population [44].
ASD
The psychiatric co-morbidities of a clinical cohort of people with ASD (n=63), referred to a specialist clinic with behavioural and/or emotional difficulties, was compared to an age and sex-matched control group of individuals referred for psychiatric assessment [45]. The ASD group, as compared to controls, was found to have a significantly higher lifetime prevalence of depressive illness (77% vs 46%), multiple anxiety disorders (59% vs 11%), and obsessive compulsive disorder (24% vs 0). A large population study in the US found that 54% of the ASD cohort (n=1507) were diagnosed with a psychiatric condition [39]. The most common psychiatric co-morbidities identified included anxiety disorder (29.13%), depression (25.75%), ADHD (11.08%), bipolar affective disorder (10.55%), OCD (7.63%) and schizophrenia (7.83%). The risk for all these conditions was increased 2-6-fold relative to that of the matched controls. The odds ratio for schizophrenia (22.24 [99%C I: 14.34-34.48]) and OCD (9.81,[99% CI: 9.81-21.82]) were particularly raised.
ADHD
The prevalence of any of the considered comorbid psychiatric disorders in adults with ADHD (n=335) was reported to be significantly higher than in those without (49% vs 33%). This included a significantly higher prevalence of anxiety disorders (23%) and depressive illness (19%) [46]. A population-based sample (n=30,532) including people with ID (3.8%) found anxiety disorders (37.9%) to be the most prevalent co-morbidity with ADHD [47]. Other evidence suggests that almost 80% of people with ADHD meet the criteria for at least one psychiatric disorder during their lifetime, with depressive illness being the most common psychiatric co-morbidity (24.4%) [48].
Premature mortality
ID
Mortality rates are higher in patients with both epilepsy and ID, independently [49]. Those with both epilepsy and ID have a higher standardised mortality ratio (SMR), which has been observed at five times that of the general population [50]. The Learning Disabilities Mortality Review Programme (LeDeR) UK is a national programme reviewing factors relating to all deaths of persons with ID in England between the age of four and 74. The annual review demonstrates that people with ID continue to die prematurely from potentially avoidable causes including seizures. The 2017 annual report found that for 25 (4%) deaths, epilepsy was cited as the main cause of death [51]. In the 2018 report, a comparable proportion of epilepsy deaths were reported (4%) [52]. In the 2019 annual report, there was a rise in number of epilepsy-related deaths to 348 (6%) [53]. The 2019 annual report also detailed the median age of death for people with ID and co-morbid epilepsy at 50 years of age, over 10 years younger than those with the other most common causes of death including pneumonia and sepsis (conditions that are more frequent with advancing age) [53]. Of the 348 epilepsy death reviews completed in 2019, 32 directly mentioned SUDEP. Common themes identified included observed changes in the person prior to death, mention or absence of assisted technologies, and problems with care related to the person's epilepsy [53]. A more recent analysis of the data demonstrates that between 1st July 2016 and 31st December 2019, one in five epilepsy deaths reviewed (as a 45% sample of the total) by the LeDeR programme were recorded as sudden unexpected death in epilepsy (SUDEP) [54].
ASD
A nationwide population-based study using Swedish registers analysed mortality in ASD (706 ASD deaths) [55]. The findings demonstrated a 2.56 (95% CI: 2.38-2.76) increased odds of mortality in comparison to the general population, this risk was significantly increased with co-morbid ID (OR=5.78; 95% CI: 4.94-6.75). There was a significantly increased risk of death through all causes of mortality considered except for infection. The highest ORs were observed with diseases of the nervous systems (OR=7.49; 95% CI: 5.78-9.72) and suicide (OR=7.55; 95% CI: 6.04-9.44), compared to the general population. Cause-specific mortality rates were higher in the ID population when compared to those with ASD without ID.
3ADHD
A large population-based Danish study (24.9 million person years) investigating an ADHD cohort (5,580 deaths) found a significantly higher mortality rate ratio (2.07; 95% CI: 1.70-2.50; p<0.0001) for all causes of death compared to those without ADHD [56]. A nationwide population-based cohort study in Taiwan (n=275,980 cases, 4,321 deaths) found higher rates of mortality in the ADHD group compared to controls for suicide, unintentional injury, and homicide. However, there was no increased risk of mortality from “natural cause” (defined as any other cause of mortality) [57]. A prospective study of a US birth cohort (n=5718) including ADHD cases (n=367) also found a significantly higher standardised mortality ratio (4.83; 95% CI: 1.14-20.46) for suicide [58].
Sudden unexpected death in epilepsy (SUDEP)
People with epilepsy and NDD, particularly ID, have a range of seizure types, often in combination. They are more likely to have generalised tonic-clonic seizures which are associated with an increased risk of injury, hospitalisation, and SUDEP [59]. A primary-care-based community prevalence study (n=318) has shown that the most common seizure type in people with epilepsy and ID was tonic-clonic seizure (38%) [12].
The incidence of SUDEP may be up to 20 times higher than in the general population [60]. A register-based review of ID deaths (n=244) in the UK identified probable or definite SUDEP (n=26) as the second commonest cause of death in people with epilepsy and ID with SMRs of 37.6 for men (95% CI: 21.9-60.2) and 52.0 for women (95% CI: 23.8-98.8) [60]. ID is a recognised static risk factor for SUDEP [61]. Other risk factors associated with SUDEP include treatment resistance over many years, early onset of epilepsy, and generalised tonic-clonic seizures in the ID population [62].
Diagnostic challenge
The following section explores some of the challenges in diagnosing epilepsy for individuals with NDDs.
A systematic review has shown that the rate of misdiagnosis of epilepsy in people with NDD may be 28%-32% [63]. The reasons for misdiagnosis are often related to the complexity of assessment in people with ID and other NDDs. Misdiagnosis may be due to misattribution or misinterpretation of other physical health conditions, psychiatric/psychological presentations, and behavioural disturbances. If there is misdiagnosis, this will lead to risk of harm to the individual through untreated epilepsy, or conversely the risk of harm due to lengthy periods of over medication with AEDs that will be ineffective.
Distortions
Focal seizures may be associated with a number of sensory symptoms affecting hearing, vision and the olfactory system which may present as hallucinations. Auras are very useful localizing “warnings” that may occur at the onset of seizure activity and evolve with the spread of epileptiform activity. However, auras are subjective symptoms which may pose a diagnostic challenge for people with NDD and epilepsy [64]. Misinterpretation and underestimation of the broad manifestation of seizure semiology can lead to misdiagnosis of psychiatric illness.
Physical health conditions
In general, it is important to be aware of the wide range of other physical health conditions that can mimic seizure activity. Potential differential diagnoses include cardiac syncope, sleep disorders, and metabolic disturbances [65].
NDD complexities
It can be challenging to distinguish between focal seizure presentations and other neuropsychiatric disturbances. There is a high prevalence of repetitive stereotyped motor behaviours in people with ID and/or ASD [66]. On neurophysiological testing, repetitive movements thought to be of an epileptic nature have been found to be non-seizure related in up to 25% of cases [67].
In context, an individual with ID and/or autism may present with brief paroxysmal, semi-purposeful motor movements that are repetitive and similar in nature without any obvious precipitant. These events may be motor stereotypies related to sensory moderation, with no relation to seizure activity.
Behavioural disturbances
Behavioural manifestations are limited representations of the cumulative effect of predisposing, precipitating, and perpetuating influencers. Accurate diagnosis is reliant upon a detailed history of events that is not always readily accessible. The outcome or behavioural manifestation of an event may be represented by brief motor movements or vague confusional states that may be attributable to a number of factors associated with a spectrum of neurological and psychiatric diagnoses [68].
Communication
The presence of communication difficulties may reduce the reliability of assessment and diagnosis. Specifically, challenges in eliciting subjective experiences can limit the accuracy of information. [63].
During the assessment process, the presence of an informant who knows the individual well is essential, which may be aided by video recordings of events. Smartphone videos have become an important diagnostic tool. For complex behaviours, a detailed functional analysis may be required to help distinguish between seizures and other causes. This process may be lengthy, involve repeated observations and require a multidisciplinary approach with assessment from a wide range of healthcare professionals beyond contact in the clinic. Assessment may be aided with the use of diagnostic investigations including video-EEG when tolerated and practicable [69].
Management
In this section, we provide a guide on how to approach treatment safely and effectively.
Individuals, carers and families should be counselled on the risk of SUDEP at the earliest appropriate time in the diagnostic process [70]. The NICE quality standards state that each person with epilepsy should have a comprehensive epilepsy care plan that is communicated between all healthcare professionals involved [71]. This care plan should include specific details regarding the epilepsy, management plans, and risk assessment. Risk assessment should be personalised and each risk should be considered individually. Where available, risk assessments should be person-centred and include standardised semi-structured, evidence-based tools such as the SUDEP and Seizure Safety Checklist [72].
People with epilepsy and NDD and their families or caregivers need to be fully aware of the epilepsy care plan. This includes the steps that should be taken in an emergency. Those providing care to people with NDD and epilepsy require regular basic epilepsy training in terms of awareness of seizure presentations, first-aid, and risk. Training can also be tailored to the specific needs of the individual where necessary. This may take place through a combination of face-to-face training by epilepsy nurse specialists and online training platforms [73].
Perhaps the most important risk consideration is monitoring of seizure activity, specifically nocturnal GTC seizures to reduce the risk of SUDEP [74]. There needs to be a robust system in place that will be effective in accessing the individual very quickly, should they have a seizure. There is a wide range of advancing smart technology that may help with seizure safety, however, to date, no smart technology has 100% specificity and sensitivity [75]. Options for night-time monitoring, dependent upon the scenario, include one-to-one support, visual monitors, and sound monitors. The appropriate choice will depend upon the individual risk, seizure semiology and profile. The use of any such interventions has to be balanced against the intrusion on an individual's right to privacy and must be evidence based and reviewed regularly.
Approach to care for persons with epilepsy and NDDs should be multidisciplinary. The effect of a comprehensive inpatient treatment programme in addressing the concerns of relatives and caregivers and patients’ quality-of-life, as assessed by caregiver questionnaires, has recently been shown in a German epilepsy centre [76].
Treatment choice
A person-centred approach must be adopted when considering treatment. Any treatment plan should be developed in collaboration with patients and caregivers. Treatment should be profiled taking into account epilepsy phenotype, physical and psychiatric co-morbidities, and risk. When considering treatment, it is important to understand that this population is more likely to continue to have seizures despite treatment [5]. The remission rates for people with epilepsy and ID have been shown to be as low as between 19.5 and 32% [5, 12, 77].
Non-pharmacological
People with NDD and treatment-resistant epilepsy should be considered for surgical assessment. Where appropriate, surgical intervention cannot only reduce seizure burden, but also improve cognitive and behavioural functioning in people with epilepsy and ID [78]. Vagus nerve stimulation (VNS) may be considered as an adjunct to treatment, with efficacy in certain populations [79]. Corpus callosotomy may lead to a reduction in the frequency of drop attacks [80]. There is also some limited evidence to support the use of a ketogenic diet in specific epilepsy syndromes, which needs to be considered on an individual basis regarding tolerability.
Pharmacological treatment
One of the main concerns for patients and caregivers is the potential for adverse effects of AEDs, particularly regarding cognition and behaviour. The adverse effects of AEDs more commonly occur when titration is rapid and doses are high. Therefore, for people with ID, the advice is to initiate at low dose (usually sub-therapeutic) and titrate slowly with close monitoring [68]. The current evidence base alongside expert interpretation is considered in a technical report on the development of clinical guidance on the management of epilepsy in people with ID [81]. This is required because of the lack of robust data available to guide treatment choice. AEDs can be graded by suitability based upon efficacy, side effect profile, safety, and expert clinical experience (table 1). This AED coding system is under continuous revision, based upon emerging evidence for newer AEDs in the ID population (table 2).
Choice of medication will be influenced by a range of factors individual to that person, including previous treatment success or failure. Second-line treatment (table 1) may be the most appropriate option for an individual at any point in time. The restrictions on the use of valproate-containing medicines for women and girls of child-bearing age varies across Europe [82]. It is therefore important that clinicians are fully aware of local regulations. The prescribing of valproate-containing medicines for girls or women with NDDs with the potential for pregnancy should follow local guidelines and only be considered in very specific circumstances and not as a first-line treatment. In some jurisdictions, regulations for valproate prescription include a pregnancy prevention programme, including adherence to user-independent contraception. There will be situations for women of child-bearing age where valproate is the most appropriate and safest treatment option on balance. Some people with NDDs, with moderate-to-profound ID, may lack the mental capacity to consent to sexual relationships, and discussion of such a programme may be potentially distressing [83].
Establishing whether there is a genetic cause for the epilepsy may also influence treatment choice. Sodium channel blocking molecules may aggravate seizures in Dravet syndrome, an epileptic encephalopathy. Older AEDs, including phenytoin and phenobarbitone, should not be prescribed without good reason due to side effect profiles and potential for drug-drug interactions. However, there will be rare occasions in which such medication is an appropriate treatment choice. Such scenarios include areas where there are no other AEDs available, for example, in some third world countries, or when the benefits of prescribing outweigh the risk [81].
Many of the older AEDs have negative effects upon cognition, an important concern when prescribing for people with NDD [93]. Clinically, these effects are usually acute and dose related. Topiramate has been shown in persons with ID to have cognitive side effects, similar to those evidenced in persons who do not have ID [94]. The interaction between epilepsy and behaviour is complex and challenging to interpret. AEDs can have both a positive and negative impact upon an individual's neuropsychiatric profile. Certain AEDs (phenobarbitone, vigabatrin, gabapentin, levetiracetam, and perampanel) show evidence of associated behavioural changes, particularly aggression in the ID population [95]. In contrast, other AEDs (valproate, lamotrigine, and carbamazepine) have demonstrated a positive impact on mood regulation and aggression [96]. In addition, improvement in seizure control can sometimes, although not always, lead to improvement in neuropsychiatric symptoms including cognition. Conversely, treatment for co-morbid psychiatric illness has the potential to worsen seizure control. Antipsychotic medications and tricyclic antidepressants, in particular, are associated with a lowered seizure threshold. Any clinical impact upon seizure control is more likely at higher dosage and the treatment for psychiatric disorders should not be avoided for fear of a theoretical impact upon seizure control. It is imperative that prescribing decisions are not based solely on one dimension, i.e. seizure control etc., but holistically. Decisions upon treatment choice should be considered on an individual basis, considering quality of life [97].
It is important to be aware of the interaction between lamotrigine and valproate because of their combined efficacy. The increase in serum levels of lamotrigine caused by valproate may result in toxicity. For people with ID and communication deficits, subjective symptoms may not be readily elicited, and may occur even when serum levels are measured within the therapeutic range. Clinicians should actively assess for signs of adverse effects when changing AEDs or altering dosage.
People with ID and epilepsy are also more likely to have gastrointestinal problems including constipation and dysphagia, and require percutaneous endoscopic gastrostomy (PEG), which will impact treatment options in terms of formulation (affecting bioavailability), monitoring and efficacy [98].
Rescue medication
Some people with epilepsy and ID will have prolonged seizures or clustering of seizures. In these scenarios, rescue medication plans should be developed to reduce the risk of harm by halting the seizure or reducing the risk of further seizures. Buccal midazolam is a commonly prescribed effective drug for use as emergency cessation of seizures. In the UK, there is best practice guidance available for the training of caregivers for the administration of medication and monitoring of adverse effects. Rescue medication prescribing should be overseen by a specialist and reviewed regularly by the epilepsy team. Clobazam may be prescribed for a set period for an individual in particular circumstances, in order to prevent clustering of seizures.
Access to treatment
In 2014, an ILAE Task Force published a White Paper that highlighted areas of concern in the care of people with epilepsy and ID [99]. In response, the ILAE working group on services for adults with epilepsy and ID conducted a survey of key stakeholders involved in the delivery of care to this population [100]. As may be expected, people with epilepsy and ID have contact with a wide range of healthcare professionals and services. However, the level of expertise in assessing and treating people with epilepsy and ID varies significantly. People with epilepsy and ID are experiencing fragmented care provision without clear pathways or communication between professionals and services. There is also a clear lack of equitable access to specialist care with long waiting times for necessary investigations such as brain imaging and EEG which will require reasonable adjustments of clinicians and services e.g. MRI under general anaesthesia. There is a gap in training and awareness of risk assessment and a need for better co-ordination between healthcare and social care services.
The National Health Service (NHS) England Rightcare Epilepsy Toolkit (2020) provides a systems approach to use as a benchmark to identify opportunities that may be improved. The Toolkit focuses on reducing mortality, increasing accuracy of diagnosis, and optimising medicine management, and is based on NICE recommendations. The Rightcare document includes reference to the Purple Light Toolkit, specific for epilepsy and NDD, and is comprised of a self-assessment checklist to help drive service improvement and development.
Step together
There is a lack of evidence mapping the complex needs of people with epilepsy and ID, and a lack of robust randomised placebo-controlled trials investigating the effectiveness of treatment [101]. There is also little by way of national or international standards to help guide clinicians and commissioners on how to meet the heterogeneous needs of this vulnerable group of people who cannot always advocate for themselves. Access to specialists with the necessary expertise can vary and is dependent upon location, and until now, there has been no clear blueprint of optimum service provision. The Step Together report has been written to help move towards integrated care for people with epilepsy and ID. The document provides a clear route for clinicians and services to map their progress towards integrated and more equitable care [102].
Clinical competencies
Knowledge on NDDs with epilepsy should be considered a specific competency for neurologists in training (table 3). Neurologists should work in collaboration with epilepsy nurses and the ID MDT. Many of the skills identified here will overlap with other core aspects of the neurology curriculum. Increased awareness of important NDD specific factors and the concept of a global neurodevelopmental presentation will help improve clinical and quality of life outcomes. This includes key skills in eliciting a detailed developmental and seizure history, in line with current understanding of epileptic encephalopathies.
Service competencies
There is a need to develop an integrated service model with clear pathways for access to epilepsy care. The service must ensure that the standard of care given to people with epilepsy and a NDD is delivered in line with evidence-based guidance with the same quality as for individuals with epilepsy without NDD, or NDD without epilepsy. A specialist service aligns the outcomes of professionals to work in a multidisciplinary approach. Adopting this model will help individualise care and consider a global neurodevelopmental picture, rather than focusing on each condition discretely. Standardising epilepsy care for people with NDD will reduce risk for the individual in terms of polypharmacy, unnecessary hospital admissions, and epilepsy-related deaths including SUDEP.
Limitations
The DSM 5 definition of intellectual disability is functional but basic. It is recognised that the prevalence studies which have largely used the DSM criteria are more likely to provide crude estimates as opposed to precise figures. However, the use of DSM 5 diagnostic criteria is most common in any population-based research investigation. It is appreciated that this provides an extremely heterogeneous group, and that the literature available is limited, and this is discussed and reflected upon throughout the paper.
Similarly, the definition and diagnostic criteria for ASD have evolved and broadened over time. This has major implications for prevalence figures quoted at different times, as presented in this paper.
While the focus has been on authors using population-based studies to provide evidence-based insights, clinic-based studies have also been utilised. While the authors recognise that clinic-based study data are of relatively limited value at times, they could be the only evidence available.
A further consideration is the co-morbid psychiatric diagnosis such as OCD in ASD and anxiety in ADHD. As these are symptom-based diagnoses with considerable overlap of core symptomology, this may have resulted in a selection bias based on the papers reviewed. It is important that future research in this area encapsulates these matters robustly.
Disclosures
Christian Brandt has been a consultant/advisor/speaker to Actelion/Idorsia, Arvelle, Desitin Pharma, Eisai, GW Pharmaceuticals, UCB Pharma and Zogenix outside the submitted work. Rohit Shankar has received institutional and research support from LivaNova, UCB, Eisai, Veriton Pharma, Bial, Averelle and GW pharmaceuticals outside the submitted work. He was the author/lead of the Royal College of Psychiatrists reports CR203, CR206 and the National Step Together Report, discussed significantly in the current paper. He is also the medical lead of the freely available SUDEP and Seizure safety Checklist which is referenced in the paper. He is the developmental disabilities representative in the recent NICE revision/update of the epilepsies (2022), the NHS RightCare report (2020), the NHS England specialist commissioning report for epilepsy (2021) and the National Confidential Inquiry into epilepsy deaths. No other author has any declared conflict of interest related to this paper.Key points
Case study 1
A young adult man is admitted to hospital having focal seizures. He has an acquired brain injury following E coli meningitis as a neonate, resulting in cerebral palsy, focal epilepsy, mild intellectual disability and autism. The young man has recently turned 18 years of age and has been known to the children's hospital from birth. However, no transition plan is in place as he moves to adult services.
His specialist school is concerned that he is having long periods of focal seizures, leading to confusion, frustration and anxiety. He remains conscious throughout but needs to walk around when the seizure is active. As a result, assessment in hospital is required.
On attendance, there is no hospital passport in place. The nursing staff found it challenging to interpret the presentation of focal seizures and autism-specific factors. There is no consideration of potential autistic sensory overload.
Parents attempt to explain the presentation of his focal seizures; dilated pupils, repeating conversations, becoming anxious and the need to walk around. Masked autistic behaviours are exposed when he is compromised. No reasonable adjustments are made, causing further stress to the patient which resulted in increasing seizure activity. The doctors take information from nursing notes. The patient and family do not believe they are listened to and the patient is discharged from hospital with a prescription for sertraline. The patient does not have a diagnosis of depression or a mental illness. No explanation for this medication is given to the young man or his parents. Once medication is increased to a therapeutic dose, the seizure frequency increases, and the young man is readmitted to hospital.
Key points:
- •Transition to adult services is a complex, stressful time that requires effective communication and planning
- •A hospital passport is an essential document that provides key information regarding an individual's needs, not restricted to their physical health.
- •Diagnostic overshadowing- the young man's presentation is attributed to ID and autism factors.
- •Reasonable adjustments should be made for the individual to inform for a thorough equitable assessment.
- •Clinicians, the patient and family should work together collaboratively.
Case study 2
A teenage autistic boy is admitted to an adult hospital having clustering of focal seizures. He also has hemiplegia, autism and an intellectual disability. The patient is presenting with focal seizures without impaired awareness, something he has experienced throughout his life. His epilepsy is drug resistant. He has been trialled on psychotropic medication previously but has been formally assessed as not having a history of mental illness or psychosis. The patient does not have a history of behaviours that challenge. It is also noted that he is intolerant to all forms of antipsychotic medications. He is intubated to facilitate an MRI scan and following this develops chest sepsis. He has a full medical passport which details that antipsychotic medication must not be administered, however, antipsychotic medication is administered to anticipate any behaviour once sedation is reduced. Following administration, he develops neuroleptic malignant syndrome, his brain swells catastrophically and the boy dies.
Key points:
- •Diagnostic overshadowing- focal seizures are common in autism but poorly understood and misinterpreted.
- •Autism impacted by seizure activity is misunderstood.
- •Patients, families, and important information are not being listened to.
Oliver's Story: https://m.youtube.com/watch?v=MG_qK5R1_as&feature=youtu.be