Epileptic Disorders
MENUEarly add-on treatment vs alternative monotherapy in patients with partial epilepsy Volume 16, numéro 2, June 2014
- Mots-clés : cluster-randomized, controlled trial, antiepileptic drug, guidelines
- DOI : 10.1684/epd.2014.0650
- Page(s) : 165-74
- Année de parution : 2014
Aim. The aim of this study was to evaluate the impact of two different therapeutic strategies in patients with partial seizures who were intractable to the first prescribed antiepileptic drug (AED); alternative monotherapy vs early add-on treatment.
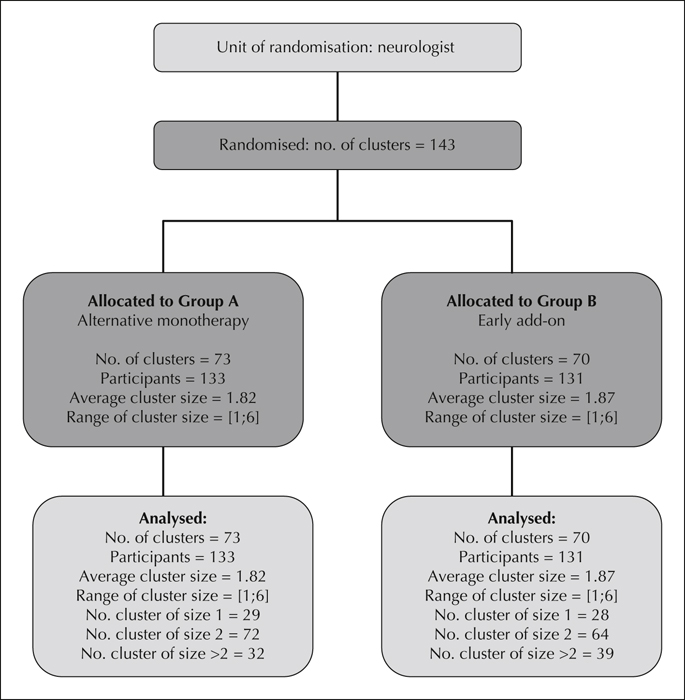
Methods. We conducted an open, cluster-randomised, prospective, controlled trial in patients with persistent partial seizures, despite treatment with one AED, who were never administered any other AEDs. Neurologists were randomised to two strategies: in group A, an alternative monotherapy with a second AED was employed; in group B, add-on treatment with a second AED was employed. The primary outcome was the percentage of seizure-free patients during a two-month period after six months of treatment. The secondary outcomes were: (i) the percentage of patients achieving a 50% reduction in the number of seizures at six months; (ii) the quality of life based on the Quality Of Life In Epilepsy scale; and (iii) tolerability.
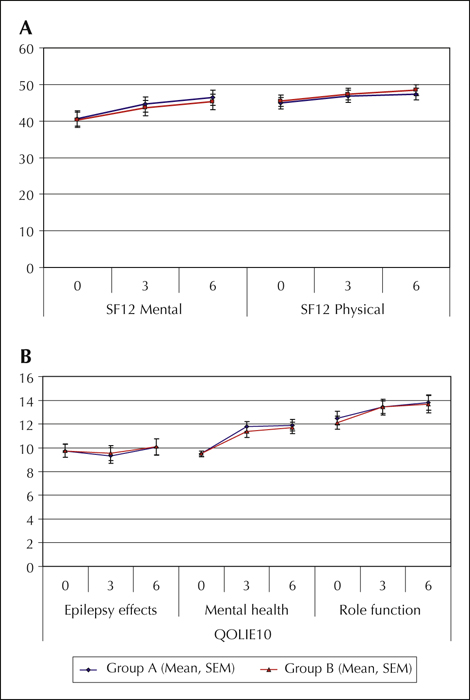
Results. A total of 143 neurologists were included and randomised, and 264 patients were evaluated. At six months, the primary outcome was 51% in group A and 45% in group B (p=0.34). The percentage of patients achieving a 50% reduction in the number of seizures at six months was 76% in group A and 84% in group B (p=0.53). The quality of life and the tolerability did not significantly differ between the two groups.
Conclusions. Alternative monotherapy or early treatment initiation with another AED drug resulted in similar efficacy, and the side effects associated with monotherapy and combined therapies were similar, which suggests that individual susceptibility is more important than the number and burden of AEDs used.