European Journal of Dermatology
MENUNodular primary cutaneous melanoma is associated with PD-L1 expression Volume 30, numéro 4, July-August 2020
- Mots-clés : nodular melanoma, PD-L1, PD-1, CD3, CD8, FoxP3, tumor infiltrating lymphocytes, Breslow index, tumor microenvironment
- DOI : 10.1684/ejd.2020.3846
- Page(s) : 352-7
- Année de parution : 2020
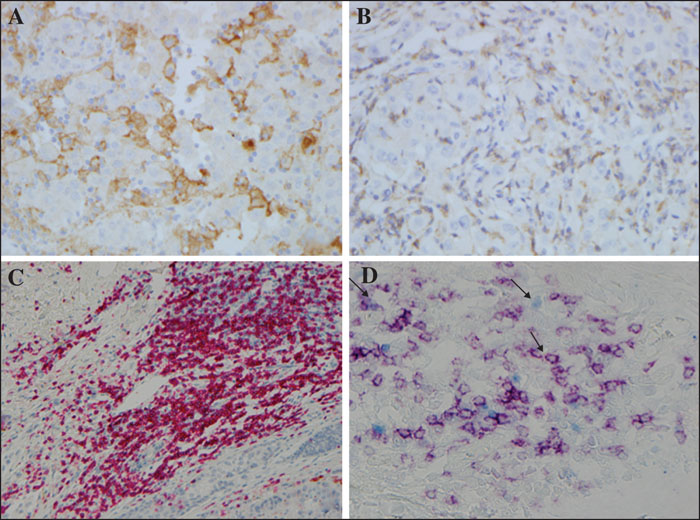
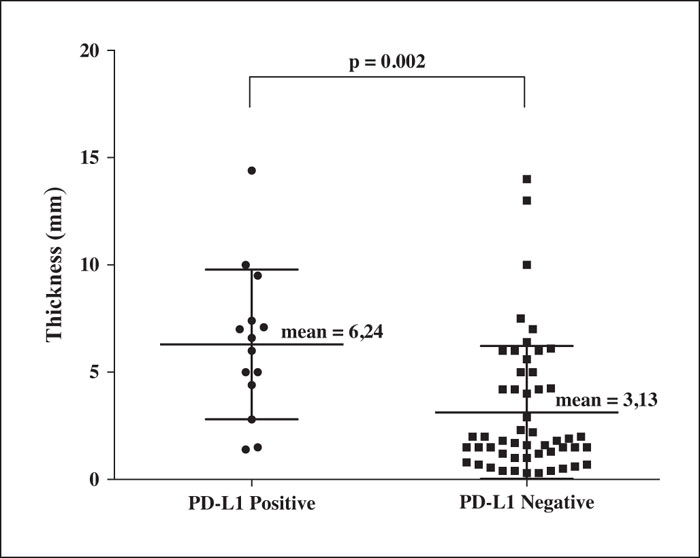
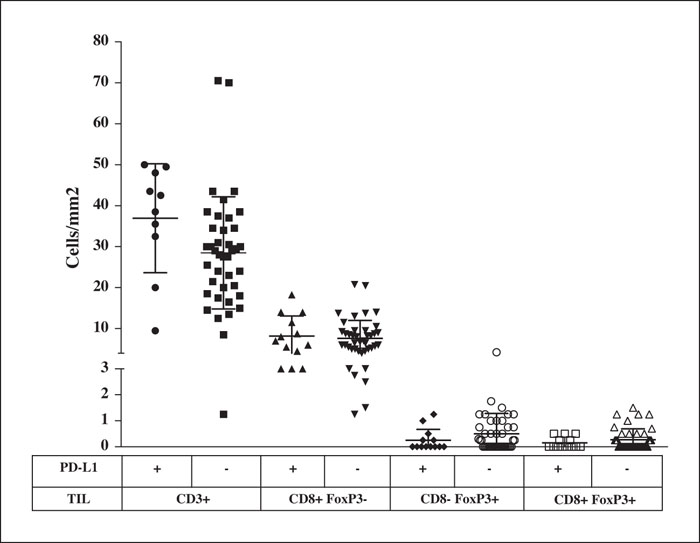
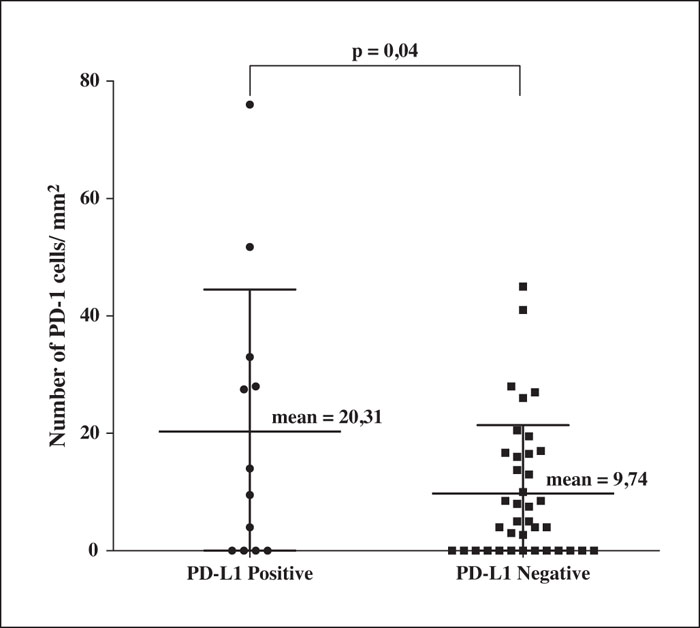
Background: In previous studies, patients with Stage III melanomas expressing PD-L1 in more than 5% of their neoplastic cells had improved recurrence-free survival with anti-PD1 adjuvant therapy. Objectives: We examined PD-L1 expression as a possible biomarker of primary cutaneous melanomas in the vertical growth phase. Materials and Methods: This was a retrospective study including 66 patients with invasive primary cutaneous melanomas. We assessed patient clinical and histopathological data and performed immunohistochemical assays with melanoma specimens from the patients to evaluate PD-L1, PD-1, CD3, CD8 and FoxP3 expression. Results: We observed PD-L1 expression in 21% (14/66) of our samples, and this expression correlated with increased melanoma thickness (p = 0.002) and nodular-type melanoma (p = 0.001). After adjusting for tumor thickness using a logistic regression test, the association of PD-L1 with nodular-type melanoma persisted. Nodular-type melanoma was 6.48 times more likely to be positive for PD-L1 than other histological types (p = 0.014; 95% CI: 1.46-28.82). As expected, PD-L1 expression correlated with the number of PD-1-expressing cells in the tumor-infiltrating lymphocyte population (p = 0.04). No correlation with PD-L1 was observed for age, sex, tumor site, skin phototype, ulceration status, sentinel lymph node status, metastasis development or survival. Regarding the immune profile of the tumor-infiltrating lymphocytes of PD-L1-positive and -negative groups, no significant differences were observed in the numbers of CD3 + , CD8 + FoxP3-, CD8-FoxP3+ and CD8 + FoxP3+ cells by immunohistochemistry. Conclusion: Nodular-type melanoma is associated with PD-L1 expression and may be a suitable candidate for adjuvant therapy of primary melanomas treated with immunotherapy.