European Journal of Dermatology
MENUDifferences in anatomical area-specific wound healing in hidradenitis suppurativa/acne inversa after surgery Volume 31, numéro 5, September-October 2021
- Mots-clés : acne inversa, CK15, CD200, secondary wound healing, progenitor cells
- DOI : 10.1684/ejd.2021.4148
- Page(s) : 623-9
- Année de parution : 2021
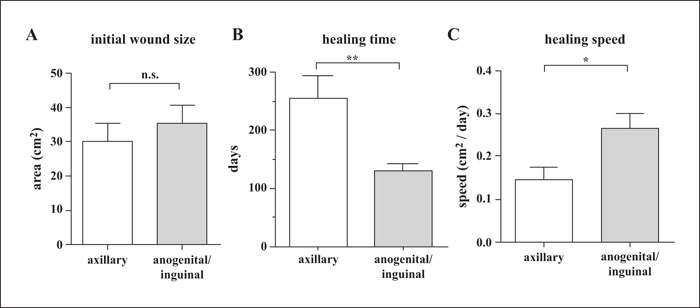
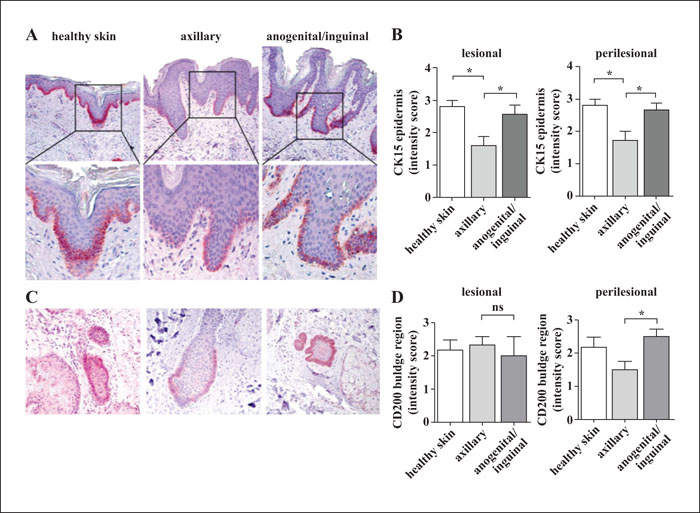
Background: Hidradenitis suppurativa/acne inversa is an inflammatory, debilitating disease for which wide local excision of the affected area with secondary wound healing is considered the treatment of first choice for the inactive scarring form or after adequate anti-inflammatory medical treatment. Objectives: In this study, we aimed to assess the duration of complete secondary wound healing after surgical intervention for hidradenitis suppurativa/acne inversa. Materials & Methods: Twenty-three surgical procedures in 17 consecutive patients (eight female, nine male) were evaluated for duration of secondary wound healing at axillary or anogenital/inguinal sites. To investigate the contribution of hair follicle bulge progenitor cells in wound re-epithelialization, tissue samples of lesional and perilesional skin were analysed for expression of the stem cell marker, cytokeratin 15 (CK15), and CD200, a marker for human follicular stem cells that resides in the bulge area. Results: Initial wound size did not differ significantly between surgical wounds in the axillary (mean: 30.0 cm2 ± 5.4) and anogenital/inguinal (mean: 35.3 cm2 ± 5.7) region. However, healing time to complete wound closure was almost twice as fast in the anogenital/inguinal (mean: 132 days ± 10.4) than axilla area (mean: 254 days ± 39.1; p < 0.01). The accelerated wound healing in the anogenital/inguinal region was accompanied by significantly enhanced CK15 and CD200 expression, compared to axillary wounds (p < 0.05). Conclusion: The anogenital/inguinal region showed significantly faster secondary wound healing after surgical intervention for hidradenitis suppurativa/acne inversa compared to axillary wounds. We suspect differences in pilosebaceous unit density and thus hair follicle progenitor cells (as mirrored by CK15 and CD200 expression) to be the main driver behind this finding.