European Cytokine Network
MENUInterleukin-17A serum levels in young patients with atopic dermatitis and food allergy Volume 32, numéro 3, September 2021
- Mots-clés : allergy, atopic dermatitis, atopy, food allergy, interleukin-17
- DOI : 10.1684/ecn.2021.0470
- Page(s) : 55-63
- Année de parution : 2021
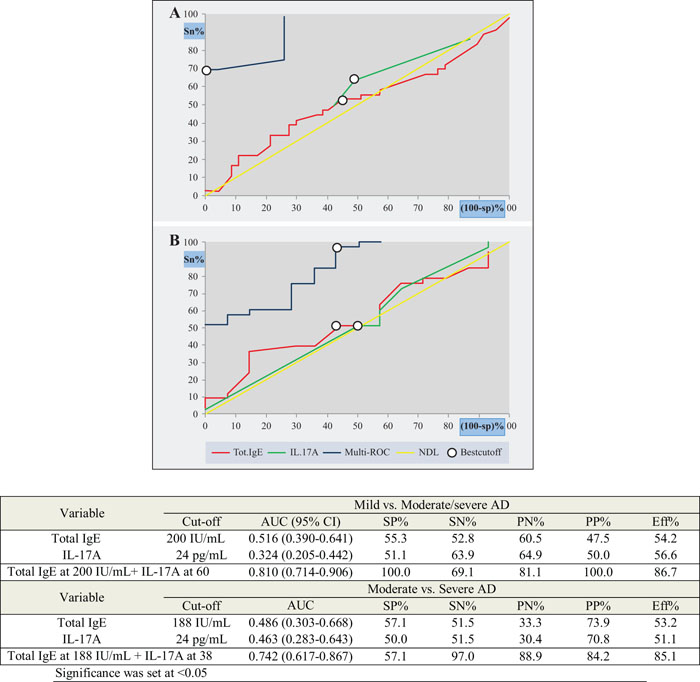
Background: Atopic dermatitis (AD) is a common skin disorder accompanied by skin barrier disruption. Patients with AD are commonly affected by food allergy. Objectives: The present case–control study aimed to assess interleukin-17A (IL-17A) serum levels in children with AD and food allergies and to determine whether increased serum levels of this inflammatory cytokine correlate with disease severity. Methods: Healthy control subjects and patients were tested for food allergen reactivity by skin prick test and specific, as well as total, immunoglobulin E (IgE) analysis. IL-17A serum levels were measured by enzyme-linked immunosorbent assay technique. Results: Patients with AD had significantly higher median (interquartile range) serum IL-17A (27 pg/mL [20–35] vs. 7 pg/mL [4.875–15.25]; P < 0.001) and total IgE levels (190 IU/mL [127–279] vs. 26.5 IU/mL [18.75–43.25]; P < 0.001) than controls and 44.6% (37/83) had a positive family history of allergy. Most patients with AD were reactive to two or three food allergens, with milk, eggs and nuts being the most common. No significant correlations were found between IL-17A levels and age and sex of patients, total IgE levels, the number and type of reactive food allergens and disease severity. In the receiver-operating characteristic analysis, the discriminating power of IL-17A and total IgE for AD severity was deficient when used alone but enhanced in combination. Conclusion: Serum IL-17A levels cannot be considered as a reliable AD severity measure and should be combined with other markers in a multimarker technique to enhance its predictive value.