Epileptic Disorders
MENUReflex epilepsy and reflex seizures of the visual system: A clinical review Volume 2, numéro 3, Septembre 2000
Definition and history
Reflex epilepsy of the visual system is characterised by seizures precipitated by visual stimuli. We exclude seizures triggered by language processing, which usually involve some visual input such as reading. Historically, photosensitivity has meant an abnormal response to light, and since the development of the stroboscope, an abnormal response to stroboscopic (flicker) stimulation during EEG recording is generally called photosensitivity. More recently, "fixation-off sensitivity" without flicker sensitivity has been identified as a separate entity (see below). The modern environment is a rich source of potentially seizure-triggering visual stimuli delivered by flickering light, pattern, and video screens to which people are exposed at all ages, world-wide. There has been a revival of interest in visual sensitivity in the past 15 years. After important initial studies in the 1940s and 1950s, visual sensitivity was regarded more as a curiosity until the mass media reported seizures triggered in otherwise healthy children and young adults by video games and TV broadcasts. Television remains the commonest trigger of these seizures in daily life.
Seizures induced by light stimulation were known from classical antiquity, and in the 20th century, even before the EEG era [1], and Adrian and Matthews documented the effect of light on the normal EEG [2]. The stroboscope became available after World War II and rapidly led to further progress as flicker stimulation and its clinical and EEG effects could be easily studied. Important studies by Walter and Walter [3], and later by groups led by Gastaut in France and by Bickford in America, yielded basic information about those EEG responses to stroboscopic flicker (intermittent photic stimulation IPS) which were reliably linked to seizures. In the last quarter century, seizures triggered by more complex visual stimuli such as patterns were studied, and the importance of eye closure and the role of visual fixation in occipital lobe EEG phenomena were reported in detail (recently reviewed in [4-8]).
Responses to intermittent photic stimulation in the EEG laboratory
Several abnormal EEG responses to IPS have been described since the late 1940s, and their occurrence in the non-epileptic population and their clinical significance with respect to epilepsy have long been a subject of discussion. Walter and Walter [3] illustrated an absence attack provoked by the stroboscope in a child with epilepsy and presciently noted that 12-18 flashes/s were the most effective stimuli and that the triggered responses were similar to the spontaneous discharges "typical wave and spike". Almost at the same time, investigators led by Gastaut [9] in France and by Bickford [10] in the USA concluded that 2 main types of EEG response could be elicited; the "photomyoclonic" response (equivalent to Gastaut's "réponse fronto-polaire par recrutement") not linked to epilepsy, and the "photoconvulsive" ("réponse fronto-centrale hypersynchrone") response associated with epilepsy. The photomyoclonic response is now called photomyogenic and the photoconvulsive response is now called the photoparoxysmal response (PPR) [11]. Some early studies were hampered by a limited number of EEG channels and misleading EEG montages, and some of their conclusions now can be seen to be incorrect. For example, Walter and Walter [3] labelled an event that was probably a photomyogenic response as a "myoclonic seizure" and Mundy-Castle [12] misinterpreted both EEG and clinical responses to IPS in asymptomatic adults as epileptic events. There are other difficulties in comparing later studies of the response to IPS as a finding either associated with epilepsy or predictive of it. These include different definitions of photoparoxysmal patterns, different techniques of stimulation, different patient populations, and the number of EEGs performed for each subject. This can lead not only to false negative but also to false positive results, e.g., when a patient has spontaneous epileptiform discharges.
Today it is accepted that among responses to IPS in untreated subjects, only generalised paroxysmal epileptiform discharges (spikes, polyspikes, and spike-and-wave complexes) are clearly linked to epilepsy. Reilly and Peters [13] emphasised the predictive value of an epileptiform response which continues after the train of flashes stops but its predictive value as distinct from that of an otherwise identical response that ends with the train of flashes remains controversial. Kasteleijn-Nolst Trenité [14] found similar results, but brief persistence of the abnormal response can also be related to how quickly the technician stops the photostimulator after the response begins.
Photosensitivity is genetically determined. Familial sensitivity to IPS was first described in 1949 [15]. There is no difference in rates of photosensitivity between relatives of nonphotosensitive epileptic subjects and relatives of controls, but photosensitivity is significantly more common in relatives of photosensitive patients. Results of such studies (for example see references [16-18]), and of other studies of the response to IPS, are complicated by the age and sex dependence of the phenomenon, which is most frequent in adolescents and females, by different patient selection criteria, and by differences in how IPS is performed. A recent study [18] reports that photosensitivity is significantly more common in 5-10 year-old siblings of proband offspring of a photosensitive parent (50%) than in siblings of photosensitive children without parental photosensitivity (14%). The highest risk of seizure (33%) was in photosensitive siblings of a proband with parental photosensitivity and the lowest (4%) in nonphotosensitive siblings of probands without parental photosensitivity. Photosensitivity occurring in some patients with identifiable epileptic syndromes, e.g., juvenile myoclonic epilepsy, is inherited separately from the other epileptic disorder. A single gene for photosensitivity has not yet been identified.
In normal children and adults, figures for sensitivity to IPS depend on age and sex distribution of the study population, the criteria for normality, and on how strictly the abnormal response to IPS is defined. Interpreting the response to IPS in an individual patient is also subject to caution: sensitivity is influenced by level of alertness, whether the eyes are open, closed, or closing at the beginning of IPS and during stimulation, the properties of the stimulator, how it is used, and the frequencies and intensity of the flashes. It is incorrect to conclude that a patient is not sensitive to IPS from a single test session. Red flashes have been found to be especially provocative of PPR. Different results reported for the effect of red stimulation are related to the different wavelengths used, and only long-wavelength red (> 600 nm) is more provocative: this stimulates red cones only, without the normal colour opponency which would be elicited by red stimuli matched to red cone sensitivity at 580 nm [19]. Even so, except for special research projects, laboratory IPS is delivered using standard stroboscopic flashes without coloured filters and normative studies have used these stimuli for decades.
Different approaches have been used to study the incidence and prevalence of sensitivity to IPS. These divide broadly into studies of asymptomatic subjects with an abnormal response to IPS, and investigations of patients with a history of seizures.
Paroxysmal responses to IPS are well documented in apparently normal subjects, especially children and adolescent girls. Doose [20] found photoparoxysmal responses in 7.6% of 662 normal children, but did not exclude those with headache or a family history of epilepsy. These investigators also used looser criteria for an abnormal response to IPS than those used by experts now. Eeg-Olofsson and Petersén [21] used stricter criteria for the normal population, excluding those with headache, paroxysmal abdominal pain, or a family history of epilepsy, and found that 8% of 673 normal children aged 1-15 years had "abnormal patterns" with IPS. Only 2/181 (1%) subjects between 16-21 years old had these, both of them women. Criteria for an abnormal response to IPS were, however, loose, including diffuse paroxysmal slow activity and spikes without generalisation. The age and sex distribution of sensitivity to IPS in both studies is shown in figure 1. Screening studies of normal young adult male candidates for aircrew training in the UK showed the fall-off in photosensitivity expected in a somewhat older population of males, with just 0.3% showing epileptiform activity with IPS only, and 0.5% with epileptiform activity both at rest and with IPS. Follow-up showed that the only subject who later developed epilepsy had epileptiform activity both spontaneously and with IPS [22].
Studies in epileptic patients show that an epileptiform response to IPS is found in about 10%-20% of children and 5%-10% of adults, and that this response is more common in females at any age. The flash frequencies most likely to elicit a PPR range typically from 9-18 flashes/s. Only about 3% of the photosensitive population is sensitive to IPS at 1-3 flashes/s. It is important to note that about 48% are sensitive at 50 flashes/s and that about 15% are sensitive at 60 flashes/s, which are also the frequencies of AC current in Europe and North America respectively [23].
Photosensitivity does not constitute an epileptic syndrome on its own. It is found in all the main categories of epileptic disorders and can be a characteristic of some disorders such as eyelid myoclonia with absences (EMA) (see below). Sensitivity to IPS is customarily divided into 3 groups: patients with flicker-induced seizures only, patients with flicker sensitivity and some other epileptic disorder, and asymptomatic subjects with photosensitivity as an isolated finding. Most subjects in this last group are primary school age and adolescent girls, and many such subjects have migraine [24]. However, this last category is now unclear, as Kasteleijn-Nolst Trenité et al. have shown that over half of known photosensitive epilepsy patients questioned immediately after stimulation denied having had brief but clear-cut seizures induced by IPS and documented by video-EEG monitoring [25]. This must raise the question of whether asymptomatic photosensitive subjects have unnoticed reflex seizures triggered by stimuli encountered in daily life.
Pure photosensitive epilepsy is characterised by generalised seizures exclusively provoked by flicker. According to Jeavons and Harding [23], 40% of photosensitive patients have this variety of epilepsy, and television is the most common precipitating factor. Video games, implicated for more than a decade, have recently become notorious, although not all such cases represent pure photosensitive epilepsy. Other typical environmental stimuli include discothèque lights and sunlight reflected from snow or the sea or interrupted by roadside structures or trees.
Pure photosensitive epilepsy is typically a disorder of adolescence, with a female predominance (reviewed in [6, 23]). The seizures are reported to be typically generalised tonic-clonic, as in 84% of Jeavons and Harding's patients, whereas absences occurred in 6%, partial motor seizures, possibly asymmetric myoclonus in some cases, in 2.5%, and myoclonic seizures in 1.5% of patients. However, these proportions are subject to selection bias: patients will come to medical attention after a convulsion in front of the TV but may have already had many less obvious unobserved seizures while watching TV. The developmental and neurological examinations are normal. Resting EEG may be normal in about half the patients, but spike-and-wave complexes may be seen with eye closure. Intermittent photic stimulation evokes a photoconvulsive response in virtually all patients. Depending on the photic stimulus and on the patient's degree of photosensitivity, the clinical response ranges from subtle eyelid myoclonus to a generalised tonic-clonic convulsion.
Pure photosensitive epilepsy is typically conceptualised as a variety of idiopathic generalised epilepsy, but rare cases have been reported in which EEG and clinical evidence favours the occipital lobe origin, as predicted by theoretical models and by studies of pattern-sensitive epilepsy (see below).
Flicker-induced occipital lobe partial seizures
Intermittent photic stimulation can also induce clear-cut partial seizures originating in the occipital lobe. As in more typical photosensitive subjects, environmental triggers include TV and video games. Many of these patients have idiopathic photosensitive occipital lobe epilepsy, a relatively benign, age-related syndrome without spontaneous seizures. Patients with spontaneous seizures, symptomatic localisation-related epilepsy, and occipital lesions have also been reported, including patients with coeliac disease. Others may have localised or regional dysplastic lesions. Some have Lafora disease. The clinical seizure pattern depends on the pattern of spread: the visual stimulus triggers initial visual symptoms which may be followed by versive movements and motor seizures, but migraine-like symptoms of throbbing headache, nausea, and at times vomiting in the immediate postictal period or even as part of the seizure (ictus emeticus), are common and can lead to delayed or incorrect diagnosis [5]. Occasional patients have been documented with subtle localised occipital ictal activity beginning during IPS, but with visual symptoms becoming clinically evident only several minutes later, after IPS had ended. This pattern may explain why some patients have seizures soon after ending a sustained exposure to visual stimuli such as a video game rather than while playing the game [26]. It is then difficult to discriminate spontaneous from evoked seizures.
Photosensitivity with spontaneous generalised seizures
Jeavons and Harding [23] found that about one third of their photosensitive patients with environmentally precipitated attacks also had spontaneous seizures similar to the reflex seizures of pure photosensitive epilepsy. Spike and wave activity was common in the resting EEG of patients with spontaneous seizures, and only 39% of patients had normal resting EEGs. Photosensitivity may accompany idiopathic generalised epilepsies, especially juvenile myoclonic epilepsy, and is typical in EMA. It may also occur with crytogenic generalised epilepsies such as severe myoclonic epilepsy of infancy (Dravet Syndrome), or with degenerative gray matter encephalopathies such as Lafora's disease, Unverricht-Lundborg disease, Kufs' disease, the neuronal ceroid lipofuscinoses, and others collectively known as the progressive myoclonus epilepsies in which photosensitivity at low flash frequencies is typical. These syndromes are associated with photic cortical reflex myoclonus and the patients also have clear-cut action myoclonus.
Pattern-sensitive epilepsy
Pattern sensitive epilepsy consists of seizures triggered by viewing patterns, typically stripes. Almost all such patients are sensitive to IPS, and about one-third of photosensitive patients may have epileptiform EEG abnormalities on viewing stationary striped patterns. Pattern sensitivity is enhanced if the pattern vibrates. Clinical pattern sensitivity is much less common, about 2% in Jeavons and Harding's work [23] and was found in 6% of subjects by Kasteleijn-Nolst Trenité [14]. Pattern sensitive epilepsy is characterised by generalised convulsions, absences, or brief myoclonic attacks provoked by viewing patterns such as escalator steps, and striped wallpaper or clothing. It is of particular interest because the generalized clinical events and EEG abnormalities are activated by an occipital cortical stimulation [4].
Self-induction of visual-sensitive seizures
Patients with all types of visually induced seizures may induce attacks with manoeuvres producing visual stimulation and may be compulsively drawn to sources of flicker or pattern stimulation such as TV screens. Patients sensitive to eye closure may use a compulsively repeated eye rolling and eyelid flicker movement to self-stimulate. Monitoring has shown that the range of stimulatory behaviours is a seizure trigger rather than being a manifestation of the seizure. Intensely pleasurable sensations have been reported with these, and some patients induce seizures to relieve stress or to gain attention. Recognition of such a sensation may help in differentiating EMA from self-induced seizures. Many patients may refuse treatment or not comply with it [8, 27].
Fixation-off sensitivity
The term "fixation-off sensitivity" (FOS) has been applied to describe subjects in whom epileptiform EEG activity, typically bioccipital, appears with abolition of visual fixation. Panayiotopoulos and co-workers have explored this phenomenon in detail (for a review, see [7]) and described clinical patterns of the associated seizures. Testing for FOS requires complete darkness or the use of devices such as goggles with high-diopter lenses to abolish fixation: the epileptiform activity can be suppressed, and thus missed during testing, if the subject fixates on even tiny sources of light such as those on the EEG machine console. Panayiotopoulos has emphasised the importance of distinguishing the act of eye closure from the eyes closed and eyes open states in evaluating spontaneous and triggered epileptiform EEG abnormalities. Patients with FOS are not typically sensitive to IPS but often have florid interictal occipital epileptiform activity with the eyes closed. This must be distinguished from eyelid myoclonia with absences (EMA), in which photosensitivity is present and in which epileptiform EEG activity and brief attacks appear with eye closure. Further discussion of FOS is beyond the scope of this paper.
Seizures induced by television and electronic screen games
Seizures induced by television screens and video games have been reported for decades [28, 29]. Television-induced seizures were initially thought to be related to malfunctioning of the set, but advances in understanding of epileptic sensitivity to light and especially of pattern sensitivity have led to better understanding of the epileptogenic properties of TV screens. In the 1990s, electronic screen games became widespread and news reports of triggered seizures brought this issue to the public eye. After specific TV commercials were found to trigger seizures, the role of screen content in triggering seizures became generally recognised. More recent outbreaks of seizures triggered by animated cartoon broadcasts have become notorious [19, 30]. These events have also caused many patients with epilepsy who are not photosensitive to believe erroneously that they are at risk from video games and these patients need accurate information about their personal risk [31].
A television screen produces flicker at the mains frequency, effectively generating IPS at 60 Hz in North America and 50 Hz in Europe. Photosensitivity is more common at the lower frequency, with nearly 50% of patients sensitive to 50 Hz IPS [23], and TV sensitivity has indeed been a greater problem in Europe than in North America. Television-induced seizures, however, are not only related to AC frequency flicker. Wilkins et al. [32, 33] described patients sensitive to IPS at 50 Hz, who apparently were sensitive to whole-screen flicker even at distances greater than 1 meter from the screen. Others were not sensitive to the AC frequency flicker, but responded to the vibrating pattern of interleaved lines at half the AC frequency that can be discerned only close to the screen. Wilkins et al. emphasised that increased distance from the screen decreased the ability to resolve the line pattern and that a small screen evoked less epileptiform activity than a large one. Binocular viewing was also needed to trigger attacks. Domestic video games using the home TV screen viewed at close distances for long periods of time, and at times under conditions of sleep deprivation and possible alcohol or nonmedical drug use can thus, not surprisingly, trigger seizures in predisposed individuals not known to have epilepsy, as well as in known photosensitive patients.
Not all seizures triggered by TV and similar screens fit this pattern. Seizures can be triggered even at greater distances and by noninterlaced screens without flicker, and flashing or patterned screen content has been implicated in these. Nevertheless, the 50/25 Hz frequency appears to be a powerful determinant of screen sensitivity and in countries with 50 Hz AC, special 100 Hz TV sets have been shown to greatly reduce the risk of attacks [34].
The broadcasting of certain forms of flashing or patterned screen content has been responsible for outbreaks of photosensitive seizures, most notably in Japan, where 685 people, most with no history of epilepsy, were hospitalised after viewing a Pocket Monsters cartoon [19, 30]: broadcast standards now exist in the United Kingdom and in Japan to reduce this risk but not in the USA or in Canada. European Community standards are expected soon. Further outbreaks are to be expected if viewers, especially mass audiences of adolescents, are exposed to such screen content when guidelines either do not exist or when they are violated [19]. These incidents are both predictable and preventable.
Seizures triggered by electronic screen games are closely linked to pattern sensitivity [35, 36]. In Europe, patients with video-game triggered seizures are also more likely to be sensitive to IPS at 50 Hz than are photosensitive patients without video-game seizures [37]. However, electronic screen games add additional factors not generally applicable to passive TV viewing, which may lead to seizures in predisposed subjects [36]. Although video-game sensitivity is usually not distinct from epileptic photosensitivity, some subjects are not photosensitive and may have seizures by chance, or induced by thinking or other factors involved in playing the game [35, 38]. Patient-dependent factors include not only the type and degree of visual or other sensitivity, but also elements such as prolonged play, at times with sleep deprivation, and possible nonmedical drug use. Screen-dependent factors are similar to those for TV, but the patient is usually closer to the TV set when playing a screen game. Image-dependent factors are important: certain types of screen background, movement, flashes, lines or stripes, spirals, etc., are predictably more epileptogenic than others. The steady maximal brightness (brightness of the brightest scene lasting > 10 s) should not be > 100 lux. Software or game-dependent factors include the speed of the game, the type of visual-motor interaction demanded by the game (typically by using a joystick, mouse, or keyboard), the types of eye movement required, and the cognitive processes involved in play. Puzzle games, for example, may not present provocative flashes or movements, but may have strongly patterned screen content and require manipulation of spatial information [36].
Prognosis and treatment
Photosensitive epilepsies are usually diagnosed in childhood or adolescence. The prognosis for control of the seizures induced by visual stimulation is generally very good, especially in pure photosensitive epilepsy and in juvenile myoclonic epilepsy, in which valproate is the drug of choice. However, only about 25% of patients with these conditions will lose their photosensitivity, and this only in their third decade [39]. Thus most such patients will relapse if medication is discontinued and especially if this is done too early, in their teens. Serial EEG evaluation using a standardised protocol, recently reviewed by a European expert panel [40], with determination of the photosensitivity range (see video) can thus be helpful to assess the response to treatment and for evaluation of photosensitivity after withdrawal of medication. The wider the range the more the patient is at risk of experiencing visually evoked seizures in daily life [14].
Patients with pure photosensitive epilepsy may be interested in treatment without drugs. Stimulus avoidance and stimulus modification can be practical in some patients and can also be combined with AED treatment. The effectiveness of these manoeuvres will depend on the individual's degree of photosensitivity, awareness of subtle signs and symptoms when exposed to potentially provocative stimuli, and on patient compliance. Avoidance of obvious sources of flashing lights and video games, especially more provocative ones such as Super Mario World [36], avoiding prolonged game play, increased distance from the TV set, view-ing a small TV in a well-lit room, and using a remote control to avoid approaching the set are all important and useful strategies. Covering one eye and turning away if the screen flickers or if myoclonic jerks occur is a helpful technique. The use of special 100 Hz TV sets has been shown to reduce sensitivity in many patients: the screen is inherently less provocative than a 50 Hz screen, but screen content may still be provocative. There are as yet no published studies on the effect of 120 Hz screens in North America where the TV screen is powered by 60 Hz current.
When needed, the drug of choice is valproate in monotherapy. Experience suggests that clobazam could be a helpful adjunct. Lamotrigine, topiramate, and levetiracetam have also been recommended as possible second choices but there are no conclusive studies of prolonged use of these drugs in human photosensitivity.
Prevention of mass outbreaks or small numbers of TV-induced seizures such as those triggered in the United Kingdom by certain advertisements or by the Japanese Pocket Monster programme involves preventing the broadcasting of potentially dangerous screen content. This has been a focus of intense attention recently: it is important to emphasise that while not every such seizure can be prevented, mass outbreaks are preventable and can be expected to occur when guidelines for screen content do not exist or when they are contravened.
Standardisation of intermittent phonic stimulation in the routine EEG laboratory
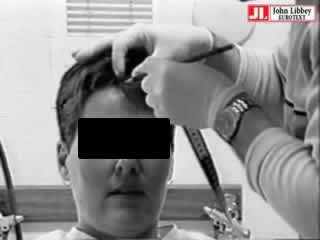
Responses to IPS are dependent on the frequencies used, on the characteristics of the stimulator, and on how it is used. It is important to deliver stimuli that are likely to elicit abnormal responses in subjects with photosensitive seizures while minimising the chance of such responses in others. We suggest avoiding the automatic stimulation sequences available on some EEG machines. The technician must be able to stop IPS as soon as generalised epileptiform activity occurs: induction of a convulsive seizure should be avoided as it is not very informative and is unpleasant and potentially dangerous. Recommendations for a standardised protocol for performing and reporting results of IPS have been made by a European expert panel and were recently reported [40]. The accompanying video provides an illustration of how this is performed: the procedure is neither difficult nor time consuming.
Because of the important role of the TV screen itself in triggering seizures independent of programme content, routine IPS should include stimulation at frequencies of 50-60 flashes/s depending on the local AC frequency, and the corresponding 25 or 30 flashes/s rate. Some degenerative disorders are associated with abnormal responses to slow rates and stimulation protocols should include rates of 1, 2, and 3 flashes/s.
Responses to IPS depend on certain characteristics of the photostimulator. The flashes must be sufficiently bright and the stimulator must deliver consistently bright flashes through-out the required frequency range of 1-60 flashes/s. Many commercial stimulators are not capable of delivering this range of flash rates and others cannot do so with consistent flash intensity. Some have small rectangular surfaces. The Grass PS-22 photostimulator meets these criteria with only a slight reduction of intensity at high flash rates [6]. The 13-cm circular lamp housing is fitted with a diffuser: this is recommended, even with other stimulators, to reduce variability which may be due to the different types of flash tubes and stimulator surfaces. A 13-cm round surface will provide a sufficiently large visual field at a viewing distance of 30 cm and permit observation of the patient. Another photostimulator meeting these criteria is the SIGMA Medicin Technik FSA 10 - 2D and 10 2-O stimulators, recently developed and tested by the manufacturer and by the Dutch epilepsy centre Stichting Epilepsie Instellingen Nederland (SEIN).
Videotape legend
The video includes a demonstration of a standardized EEG laboratory procedure for intermittent photic stimulation (IPS) and for determining the photosensitivity range. It also demonstrates sensitivity to IPS, television, video games, and pattern.
Method of intermittent photic stimulation: after the patient has been placed 30 cm from the photic stimulator, separate 10-second trains of flashes are given for each frequency with intervals of at least 7 seconds between stimulus trains. The eyes are open for the first 5 seconds of each train of flashes and closed for another 5 seconds. We advise the following frequencies: 1, 2, 4, 6, 8, 10, 12, 14, 16, 18, 20 flashes/second and 60, 50, 40, 30, 25 flashes/second. Stimuli start at 1 and progress to 20 flashes/second unless generalized epileptiform discharges are evoked at a lower frequency. Stimulation is resumed at 60 flashes/second, decreasing to 25 with the same precautions. Total screening time is 6 minutes or less [6].
CONCLUSION
Patients with visual-sensitive seizures are familiar to the epilepsy specialist, but general neurologists, paediatricians, and general practitioners should also expect to encounter them. The modern environment provides many sources of epileptogenic stimulation for these patients and for those with previously unsuspected photosensitivity: the prognosis for most is excellent if the trigger is recognised and appropriate treatment begun and continued. Sensitivity to TV screens and video games is not rare and restrictions on potentially dangerous screen content are needed to prevent outbreaks of triggered seizures. The treatment of epileptic photosensitivity is a good example of an approach combining antiepileptic drugs, other individual measures, and a role for society at large.
Received July 24, 2000 / Accepted July 28, 2000