European Journal of Dermatology
MENULeg ulcers associated with cutaneous vascular degeneration in a patient receiving pazopanib chemotherapy Volume 27, numéro 5, September-October 2017
Illustrations
Pazopanib is an oral multi-targeted tyrosine kinase inhibitor (TKI) used for the treatment of advanced renal cell carcinoma (RCC) and soft tissue sarcoma. Cutaneous adverse effects of pazopanib are very rare. We herein report a patient with advanced RCC who developed, during chemotherapy with pazopanib, multiple ulcers on both lower legs associated with cutaneous vascular degeneration.
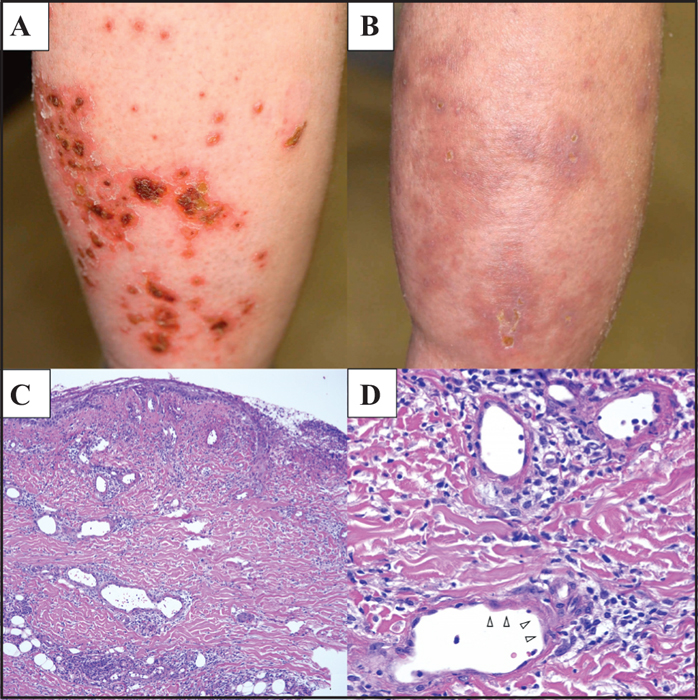
A 66-year-old man was diagnosed with metastatic RCC (of clear cell type) and underwent left nephrectomy. Thereafter, chemotherapy with sorafenib, in combination with interferon-α, was initiated to treat bone, lung, and brain metastases. He also received radiation to the femur and the brain. However, chemotherapy was discontinued after 29 days due to hand-foot syndrome induced by the sorafenib and a skin ulcer on the left thigh caused by the subcutaneous injection of interferon-α. He was administered pazopanib at 800 mg/day. Eight weeks after the initiation of pazopanib, he developed, on both his lower legs, multiple small skin ulcers of less than 20 mm in diameter, erythema, and oedema (figure 1A). A biopsy specimen from the ulcer of the right leg showed in the dermis diffuse lymphocytic infiltration and eosinophilic vascular degeneration, characterized by loss or degeneration of endothelial cells and thickening of the vessel walls. Although lymphocytic infiltration was observed around the degenerated vessels, no active vasculitis was seen (figure 1C, D). The ulcers enlarged despite topical application of a steroid ointment for one week. Thus, oral pazopanib was discontinued, and the ulcers significantly improved and epithelized within two weeks, with slight scarring and pigmentation (figure 1B). We presumed this case to be a cutaneous adverse drug reaction due to pazopanib. No skin ulcer recurrence has been observed in the one-year follow-up period.
TKIs are among the most successful drugs for treating metastatic RCC [1]. They are regarded as anti-angiogenic agents, and function primarily by inhibiting tumour angiogenesis and tumour cell survival signalling [1]. Pazopanib targets multiple tyrosine kinases, including VEGFR-1, -2 and -3 [2]. Serious cutaneous adverse effects of TKIs tend to occur during the initial two months of treatment, particularly in males and older patients [3]. Major adverse effects of pazopanib include hypertension, diarrhoea, hair colour changes, nausea, anorexia, and vomiting, whereas cutaneous manifestations are rare [3]. Hand-foot syndrome is frequently seen in patients treated with sorafenib and sunitinib, but less commonly with pazopanib [4]. Regarding the skin ulcers associated with pazopanib, there are only two similar published case reports [5, 6]. Both cases presented with multiple ulcers on the lower legs, as in our patient. To the best of our knowledge, detailed histopathological features of vascular degeneration have never been described in patients treated with pazopanib. In the present case, the vascular degeneration lacked apparent active vasculitis, suggesting that the vascular change was primarily due to the anti-angiogenic effect of pazopanib, rather than to vasculitis. Further cases should be accumulated to elucidate more precisely the mechanisms of pazopanib-associated skin ulcers.
Disclosure
Financial support: none. Conflict of interest: none.