Epileptic Disorders
MENUImproved seizure burden and cognitive performance in a child treated with responsive neurostimulation (RNS) following febrile infection related epilepsy syndrome (FIRES) Volume 22, numéro 6, December 2020
- Mots-clés : responsive neurostimulation, pediatric epilepsy, FIRES
- DOI : 10.1684/epd.2020.1224
- Page(s) : 811-6
- Année de parution : 2020
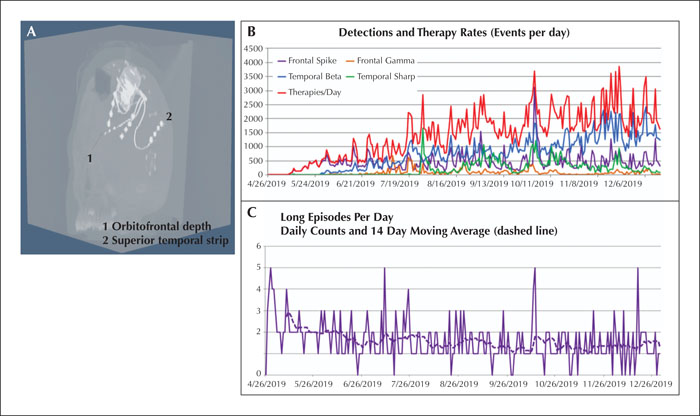
Responsive neurostimulation (RNS) is an emerging therapy for patients with refractory focal epilepsy who are not candidates for surgical resection, with limited published experience in the pediatric population. We report a case of refractory multifocal epilepsy following febrile infection related epilepsy syndrome (FIRES) in which surgical resection was not feasible due to multifocal independent seizures and risk of cognitive deficit, and RNS was pursued. Relevant RNS data and neuropsychological testing results were reviewed. By eight months after implantation, decreased frequency and severity of clinical seizures were noted, and RNS data revealed decreased “long episodes,” reduced spread of electrographic seizures, and fewer detections. Neuropsychological assessment, though potentially confounded by stimulant medication, revealed significant improvement in multiple cognitive domains, particularly working memory and processing speed, at six months. These findings illustrate success in detecting and aborting seizures, and additionally suggest a neuromodulatory effect of RNS stimulation. Our case demonstrates feasibility, efficacy and safety of RNS in a pediatric patient with FIRES, with evidence to also suggest cognitive improvement.