European Journal of Dermatology
MENUVitiligo and thyroid disease: a systematic review and meta-analysis Volume 28, numéro 6, November-December 2018
Department of Internal Medicine,
National Taiwan University Hospital Hsinchu Branch,
Hsinchu,
Taiwan
College of Medicine,
National Taiwan University,
Taipei,
Taiwan
School of Medicine,
College of Medicine,
Taipei Medical University,
Taipei,
Taiwan
- Mots-clés : vitiligo, thyroid disease, autoimmune thyroid disease, anti-thyroperoxidase antibody, anti-thyroglobulin antibody, meta-analysis
- DOI : 10.1684/ejd.2018.3449
- Page(s) : 750-63
- Année de parution : 2018
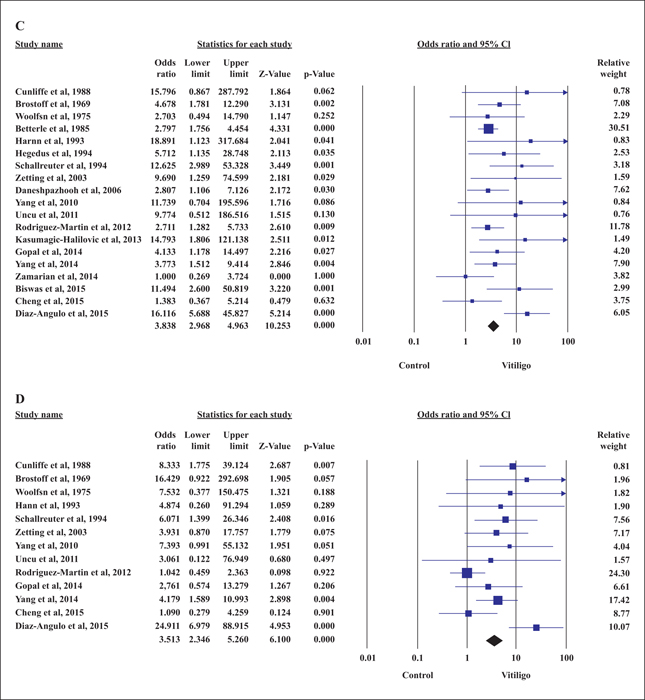
Vitiligo is associated with (autoimmune) thyroid disease. However, confounding factors, including type and onset of vitiligo, require elucidation. We conducted a meta-analysis to identify vitiligo patients with increased risk of (autoimmune) thyroid disease. Studies were identified based on searches in PubMed, MEDLINE, Embase, and the Cochrane Library from inception of these databases to August 31st, 2017. Odds ratios (ORs) for the prevalence of (autoimmune) thyroid disease and thyroid antibodies in vitiligo patients were pooled, and subgroup analysis was performed. Thirty-seven studies with 78,714 vitiligo patients met the inclusion criteria. The prevalence of thyroid disease (TD) (OR: 3.932; 95% CI: 2.230-6.933), autoimmune TD (OR: 5.879; 95% CI: 2.682-12.885), anti-thyroperoxidase (TPO) antibody (OR: 3.838; 95% CI: 2.968-4.963), and anti-thyroglobulin antibody (OR: 3.513; 95% CI: 2.346-5.260) was significantly higher in vitiligo patients than in controls. Notably, the prevalence of TD and anti-TPO antibody was significantly higher in patients with non-segmental vitiligo, compared to those with segmental vitiligo. In contrast, the prevalence of TD was significantly lower in early-, compared to the late-onset vitiligo group (OR: 0.333; 95% CI: 0.244-0.453). Physicians should be aware of the increased risk of (autoimmune) thyroid disease in vitiligo patients. We recommend routine screening for anti-thyroid antibodies in vitiligo patients.