L'Orthodontie Française
MENUSurgical and non-surgical maxillary expansion: expansion patterns, complications and failures Volume 93, special issue 1, Décembre 2022
- Key words: SARPE, DOME, MARPE, MSE, ALF, EASE, AGGA, DNA, OSA, Airway, Maxillary expansion, Nasomaxillary expansion
- DOI : 10.1684/orthodfr.2022.87
- Page(s) : 35-46
- Published in: 2022
Objective
The focus of this report was to analyze the pattern of maxillary expansion and complications in patients following surgical and non-surgical maxillary expansion presented for evaluation and second opinion.
Materials and Methods
During a 30-months period, 28 patients presented for second opinion following maxillary expansion performed elsewhere. The indication for treatment was obstructive sleep apnea (OSA). All patients reported a lack of symptomatic improvements and problems associated with the treatment. Clinical examination with pre- and post-expansion cone beam computed tomography (CBCT), and treatment photographs were analyzed.
Results
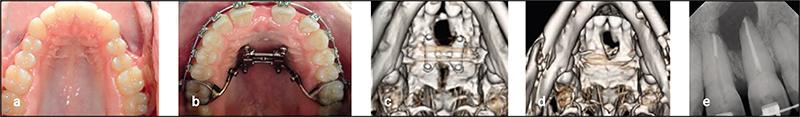
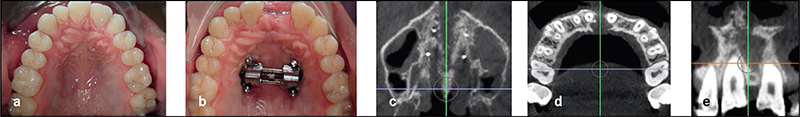
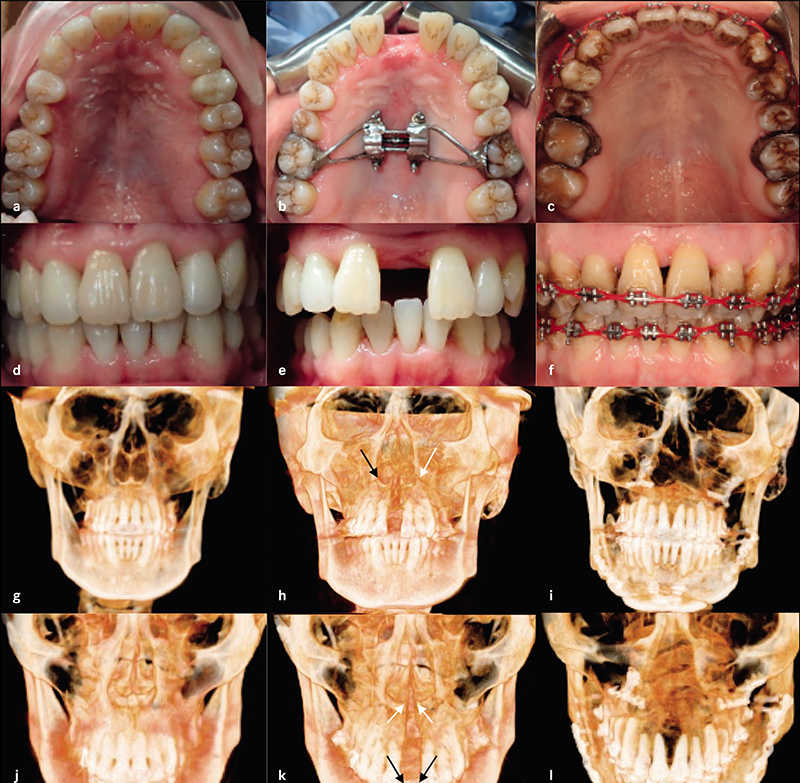
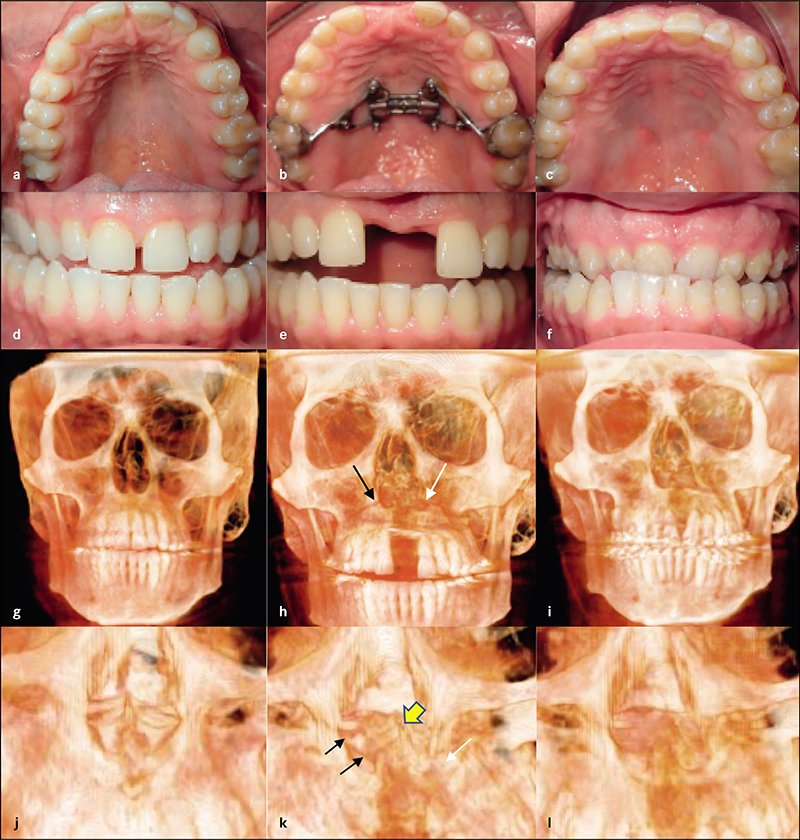
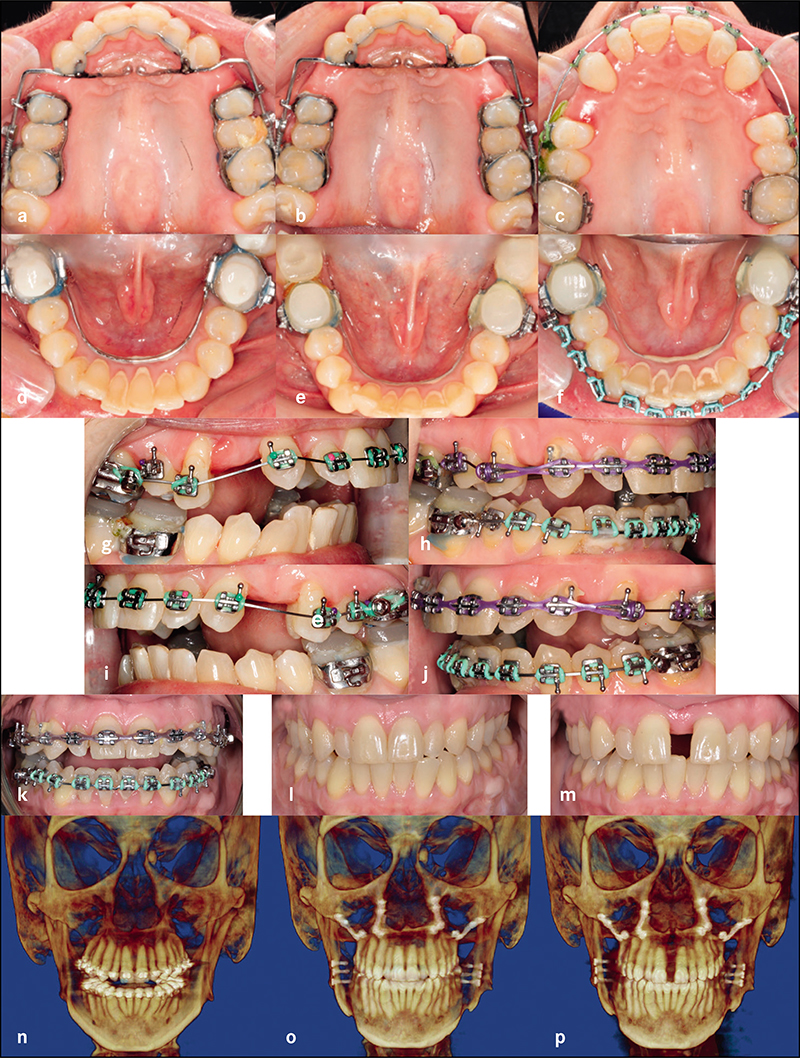
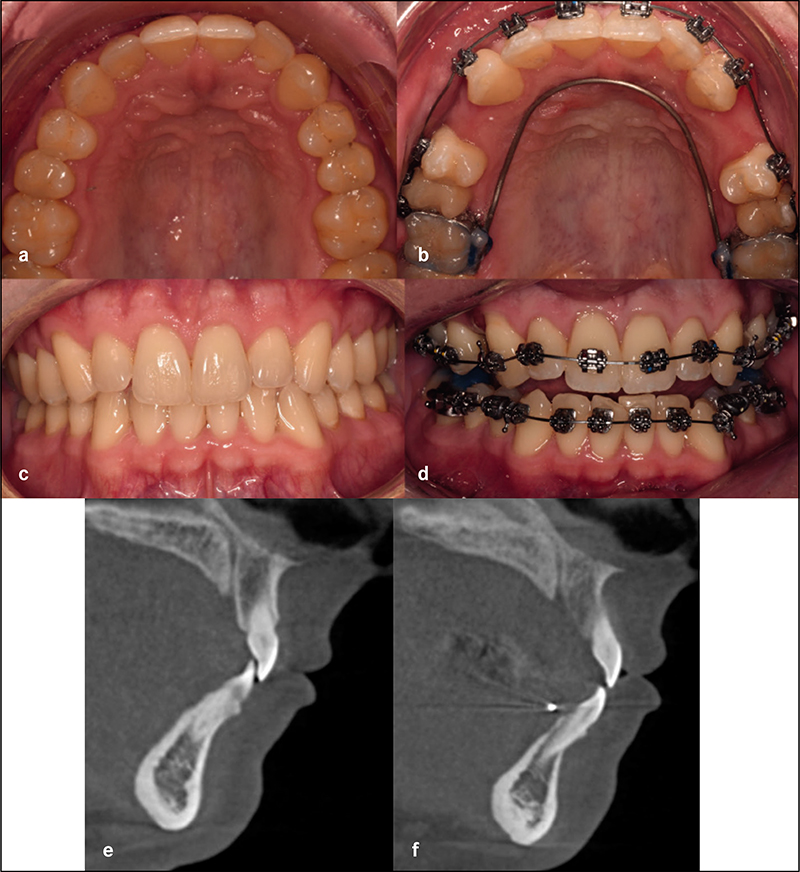
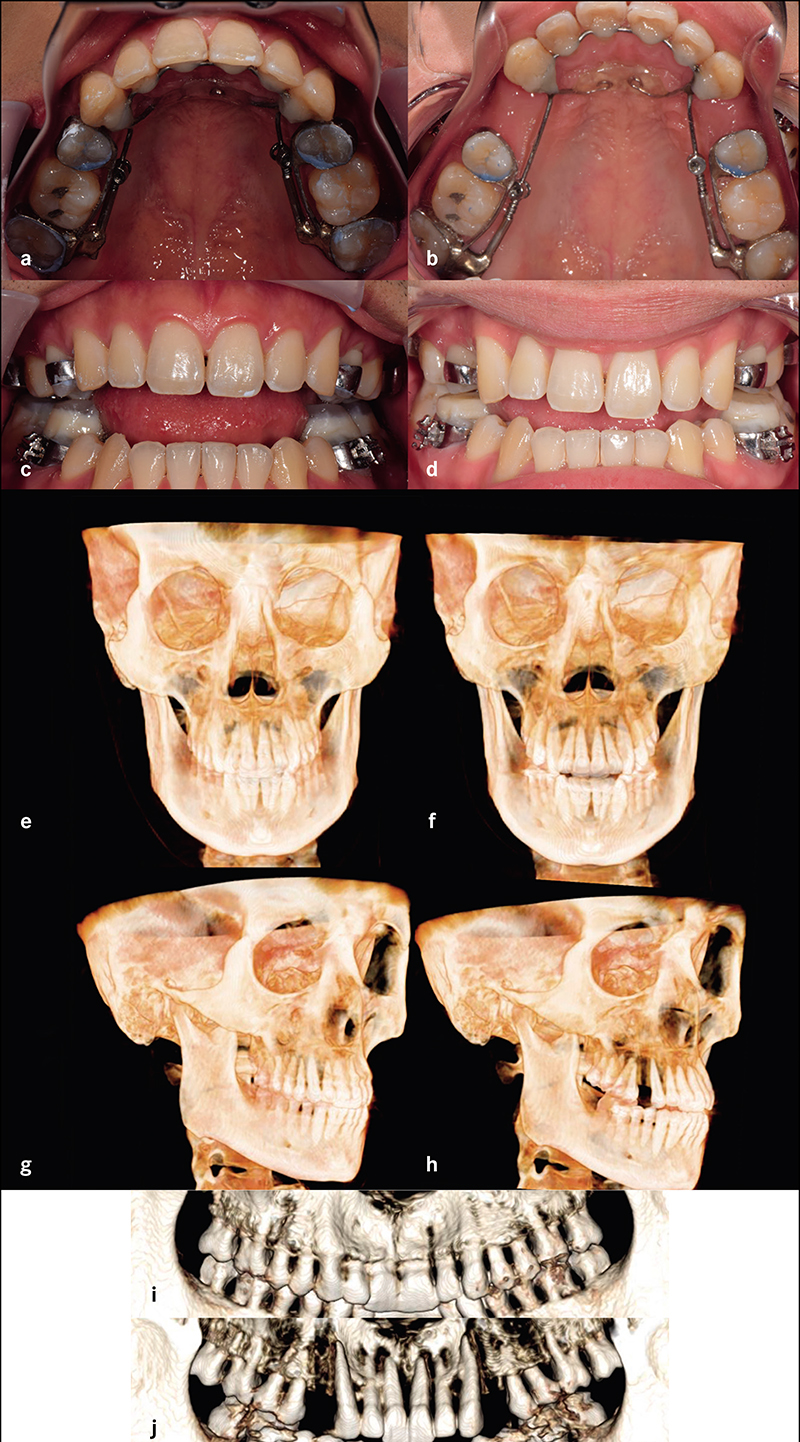
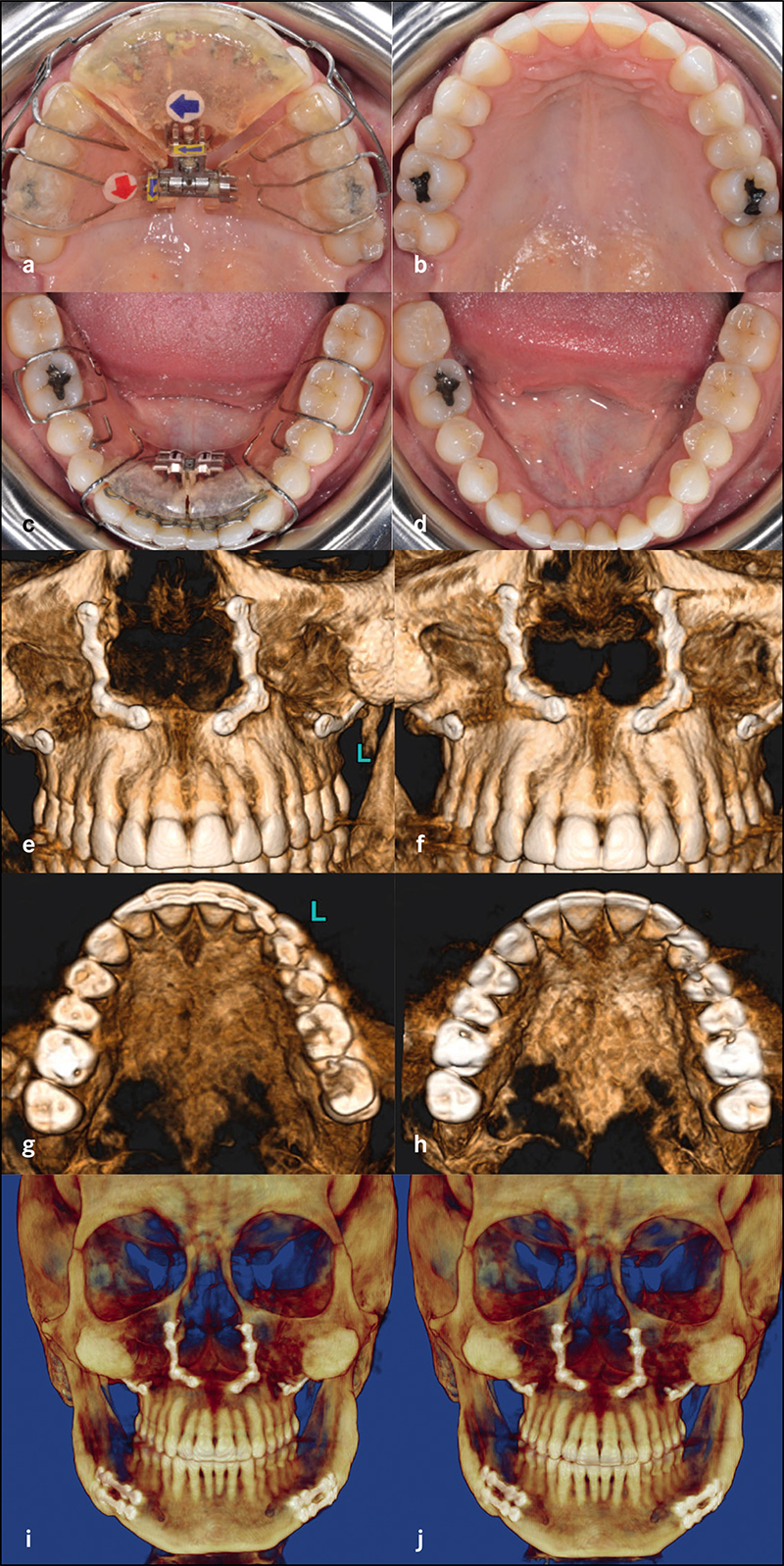
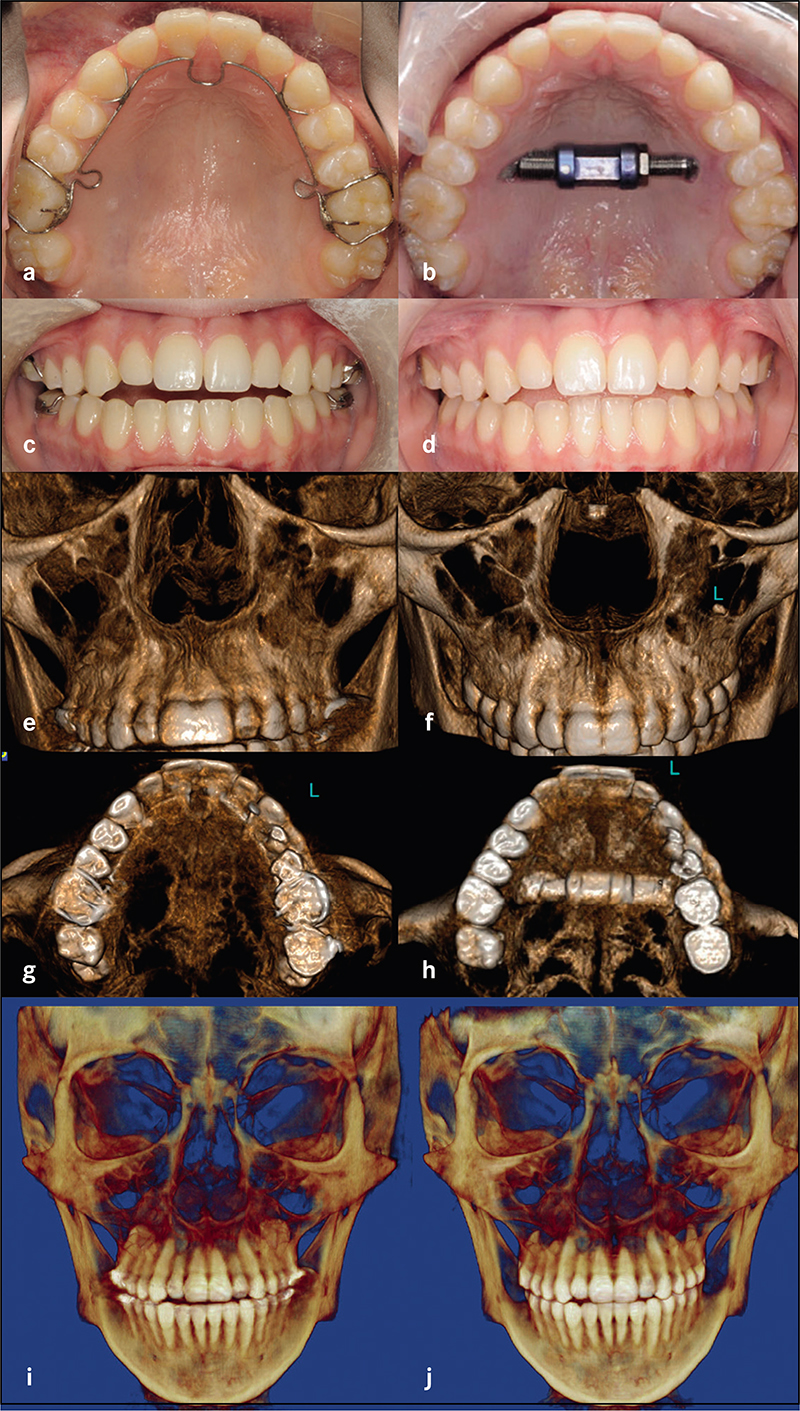
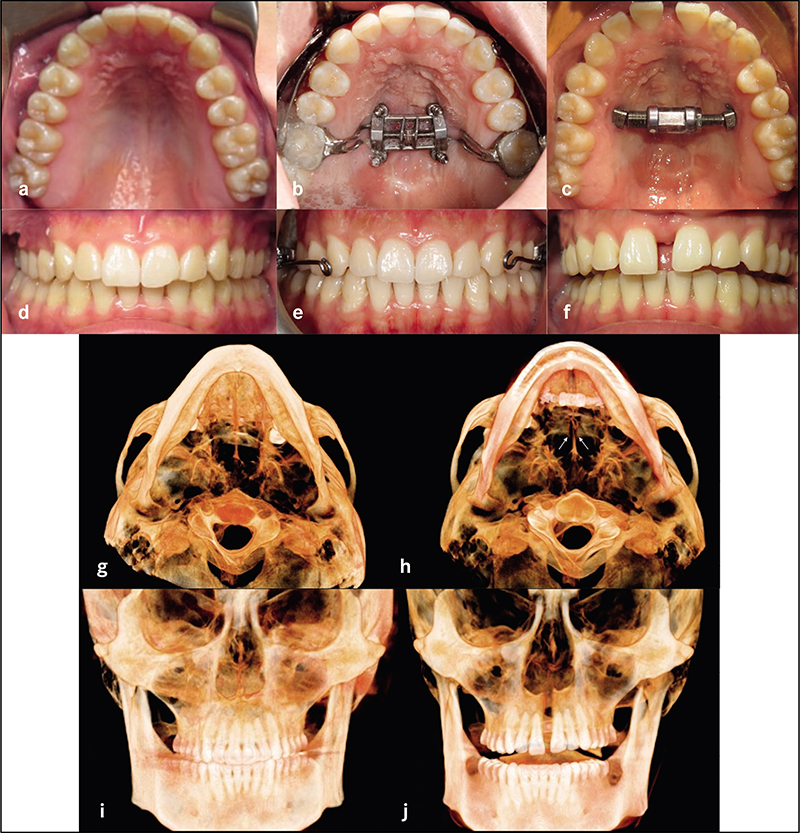
Complete clinical records and CBCT were available in 22 patients for analysis. Six patients had undergone surgical expansion with distraction osteogenesis maxillary expansion (DOME), and 16 patients had undergone a variety of non-surgical expansion with different appliances. All the DOME patients had anterior nasal spine (ANS) separation without posterior nasal spine (PNS) separation. Diastema ranging between 10-16 mm was noted in the DOME patients, and the ratio of anterior diastema to ANS separation was between 2:1 to 3:1. Bone defects existed between the central incisors at 18 months or beyond following DOME in all the patients despite bone grafting attempts in four patients. Anterior gingival recession occurred in two patients and four incisor teeth required endodontic therapy with long-term guarded prognosis. Sixteen patients underwent non-surgical maxillary expansion with four different appliances, including anterior growth guidance appliance (AGGA), daytime-nighttime appliance (DNA), advanced lightwire functionals appliance (ALF), and mini-screw assisted rapid palatal expansion (MARPE). The midpalatal suture did not separate in any of the 16 patients, and the expansion pattern was purely dental and dentoalveolar in nature. Lateral dental tipping, thinning of the labial/ buccal alveolar bone with gingival recession were noted in 10 patients. Significant mobility of the maxillary anterior teeth due to vertical and horizontal bone loss was noted in the five patients that underwent AGGA treatment.
Conclusions
Different maxillary expansion methods are currently being performed with varying outcomes. Critical analyses of these methods are needed to determine their impact and whether the desired outcomes are achieved.