Gériatrie et Psychologie Neuropsychiatrie du Vieillissement
MENUBurnout in nursing staff caring for patients with dementia: role of empathy and impact of empathy-based training program Volume 16, issue 2, Juin 2018
- Key words: geriatric care, job satisfaction, perspective-taking, sympathy, Validation training
- DOI : 10.1684/pnv.2018.0735
- Page(s) : 215-22
- Published in: 2018
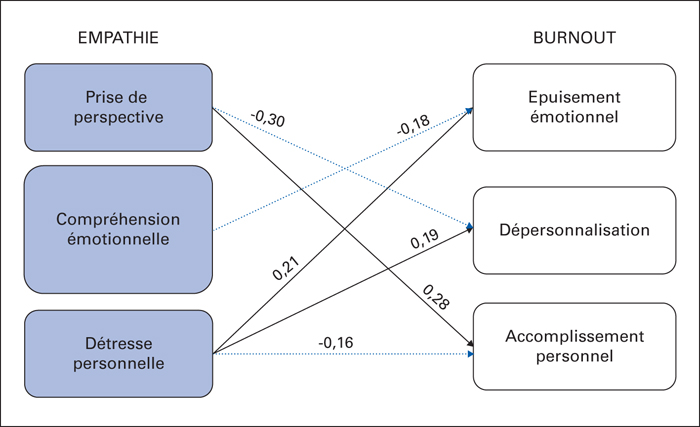
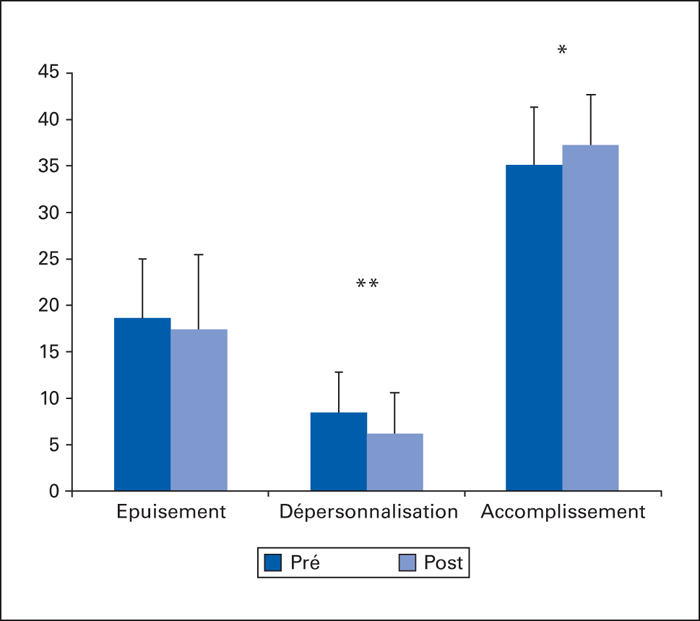
Objectives: Although relationships between empathy and burnout have been reported, it remains unclear whether empathy should be considered as a predictive or a protective factor. A multidimensional approach towards empathy was selected to determine whether cognitive and emotional aspects might differently contribute to the burnout (first study). In a second study, we aimed at investigating the effect of empathy-based training program on empathic skills and burnout.Methods: The first survey was conducted among 124 nursing staff from 10 geriatric residential facilities. They filled out (i) the Maslach burnout inventory (assessing emotional exhaustion, depersonalization and personal accomplishment); (ii) two empathy questionnaires assessing both cognitive (perspective-taking, i.e. the tendency to adopt another person's point of view) and emotional empathy (compassionate care, i.e. the propensity to take patients’ feelings into account; and personal distress, i.e. feelings of discomfort in relationships). In the second study, questionnaires were filled out by 41 caregivers before and after an empathy-based training program (Validation®).Results: results showed that higher personal distress predicted higher burnout scores while higher compassionate care predicted lower emotional exhaustion and higher perspective-taking predicted lower depersonalization as well as higher accomplishment. Results from the second study showed that personal distress decreased after the Validation training and nursing staffs reported lower depersonalization and higher accomplishment. Conclusion: The first study suggests that, in predicting the decrease of burnout symptomatology, perspective-taking and the propensity for compassionate care should be considered as protective factors, whereas personal distress can be considered as a predictive factor. Moreover, empathy-based training programs such as Validation® could contribute to the prevention of burnout by decreasing signs of personal distress. The nature of this component (empathy or sympathy) is discussed.