Epileptic Disorders
MENUUnmasking the entity of ‘drug-resistant’ perioral myoclonia with absences: the twitches, darts and domes! Volume 23, issue 2, April 2021
- Key words: perioral myoclonia with absences, genetic generalized epilepsy, video-EEG, diagnosis
- DOI : 10.1684/epd.2021.1265
- Page(s) : 313-24
- Published in: 2021
Objective
Perioral myoclonia with absences (POMA) is not recognized as a unique electro-clinical syndrome and studies suggest its inclusion under the genetic generalized epilepsy (GGE) spectrum. The aim of this study was to explore the prevalence and electro-clinical homogeneity of this disorder in an epilepsy monitoring unit.
Methods
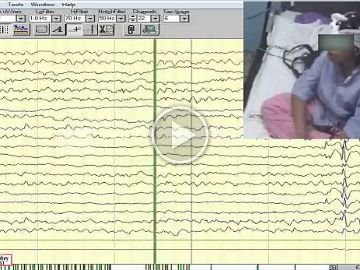
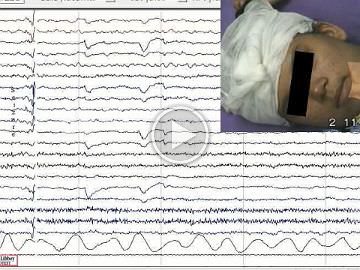
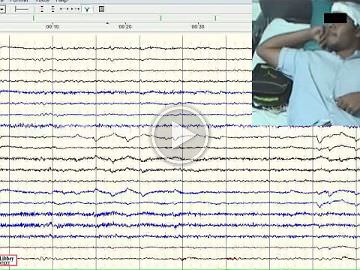
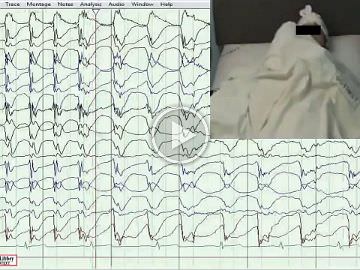
Between 2013 and 2019, among drug-resistant epilepsy patients who were referred for video-telemetry, those diagnosed with POMA based on the presence of documented absences with prominently observed peri-oral muscular contractions accompanied by generalized EEG features were included.
Results
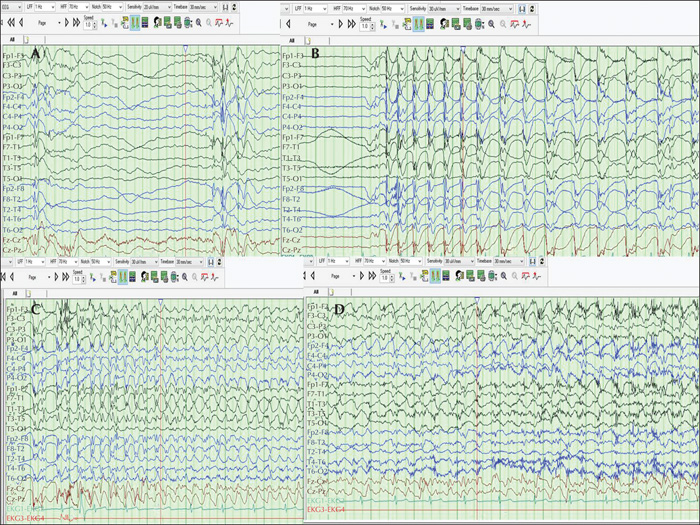
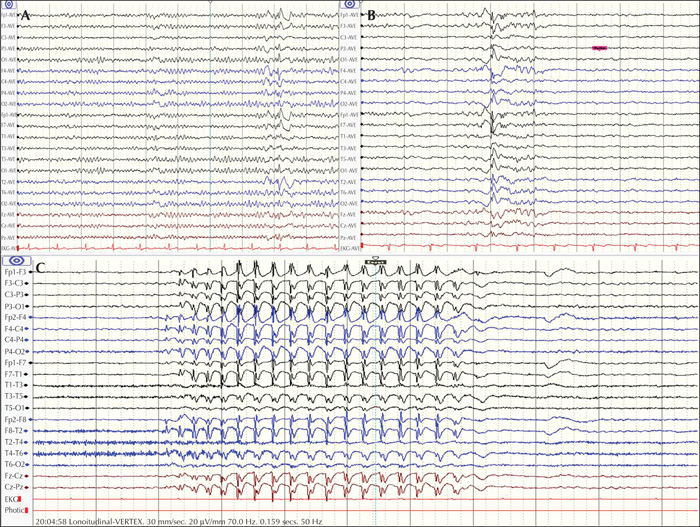
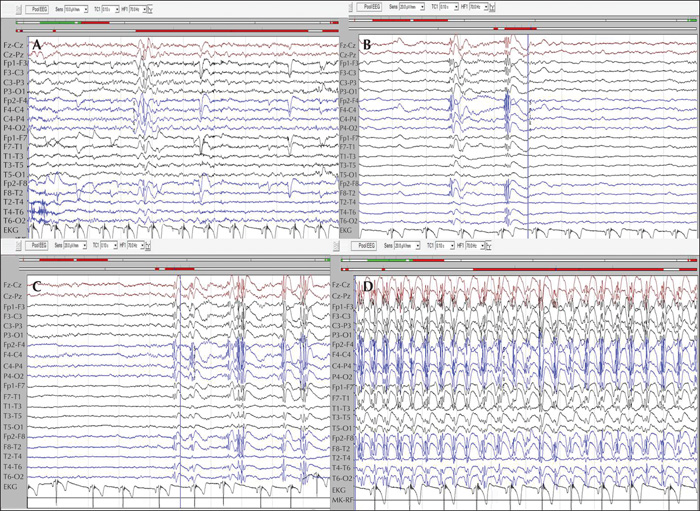
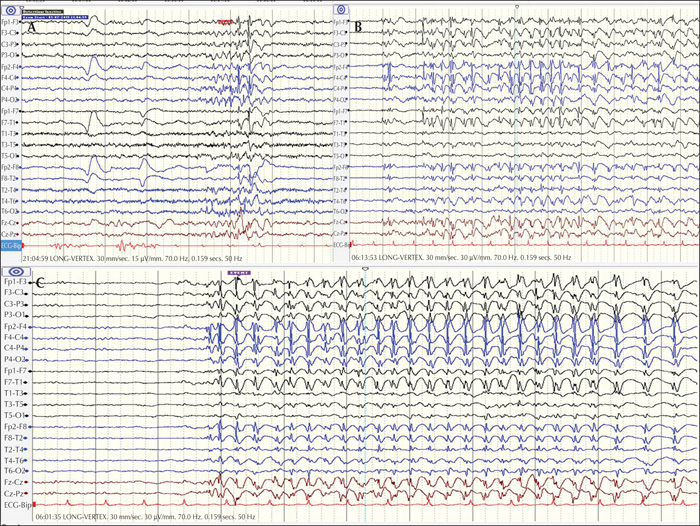
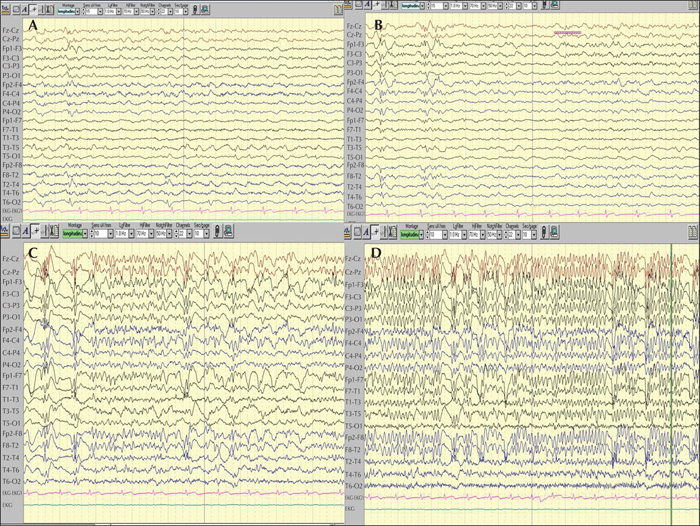
Among 62 patients who were diagnosed with absence epilepsy, five finally met the criteria for POMA (8.1%) with late childhood or adolescent onset of epilepsy. Four (80%) had a referral diagnosis of focal epilepsy based on historical focal features with exacerbation of seizures on oxcarbazepine. All five patients demonstrated brief absences with orbicularis oris muscle contractions accompanied by subtle focal phenomenology. One patient had concurrent axial-appendicular myoclonic jerks precipitated by hyperventilation. While four patients had strikingly identical interictal and ictal characteristics of typical absence epilepsy, one patient demonstrated additional atypical generalized polyspike discharges without a “dart-dome” morphology. Therapeutic response to introduction of sodium valproate was noted in all five patients. Features that were not consistent with the diagnosis were apparent in one patient who was re-classified with combined focal and generalized epilepsy. Differentiating aspects in this patient included multifocal discharges, background slowing, fast-recruiting ictal rhythms and valproate resistance.
Significance
This is one of the largest case series of POMA. This entity, which falls under the spectrum of GGE, remains under-diagnosed and its distinctive electro-clinical features need to be recorded in order to prevent misclassification as focal epilepsy of probable opercular origin. Background-slowing, atypical ictal rhythms and valproate unresponsiveness are not consistent with the diagnosis of this unique absence epilepsy. [Published with video sequences].