Epileptic Disorders
MENUFacing the hidden wall in mesial extratemporal lobe epilepsy Volume 20, issue 1, February 2018
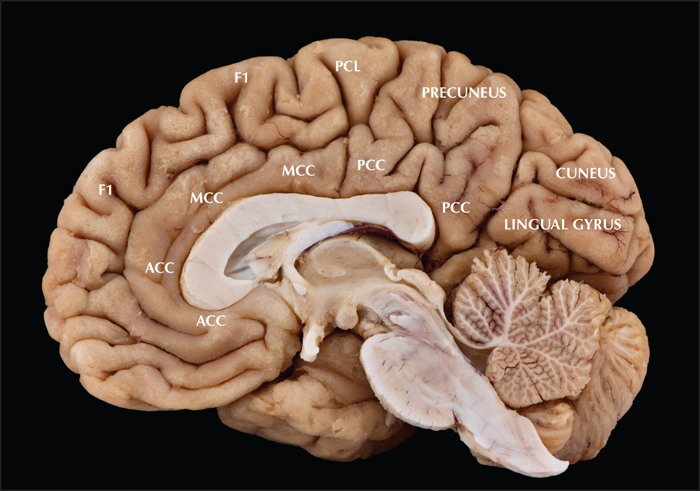
Figure 1
Mesial extratemporal lobe areas. The mesial extratemporal cortex encompasses the superior frontal gyrus (F1), including the SMA, pre-SMA and mesial prefrontal cortex, the paracentral lobule (PCL), the precuneus, the cingulate cortex (ACC, MCC and PCC), and the mesial occipital cortex (cuneus and lingual gyrus). The cingulate gyrus is divided into its anterior (ACC), middle (MCC), and posterior part (PCC).
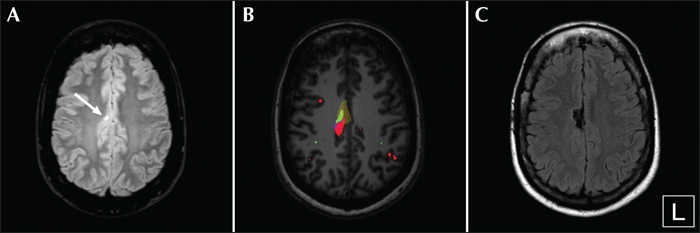
Figure 2
SISCOM in mesial frontal lobe epilepsy due to focal cortical dysplasia. This 46-year-old woman suffered from refractory frontal lobe epilepsy since the age of 7. Interictal EEGs showed right frontocentral (FP2, F8, F4, Fz and C4) sharp waves. Seizures started with eye and head deviation to the right, followed by hyperkinetic movements. Ictal EEGs showed rhythmic fast right frontocentral activity in some of the seizures. (A) FLAIR imaging showed a very discrete hyperintense region (arrow) in the right mesial frontal cortex. (B) Morphometric analysis showed an abnormal “extension” (blue), “junction” (green), and “thickness” (red) in this region, consistent with a focal dysplastic lesion. SISCOM (yellow), thresholded at +2 SD, showed a cluster of hyperperfusion overlapping with this structural abnormality. This non-invasive multimodal imaging enabled non-invasive delineation of the epileptogenic zone. (C) The patient underwent neurosurgery, targeting the focal dysplastic lesion in the anterior cingulate cortex overlapping the SISCOM hyperperfusion cluster. The neurosurgical resection was guided by intraoperative neuronavigation (Brainlab) and intraoperative neurophysiology (ECOG). Pathology showed focal cortical dysplasia type IIb. The patient has remained seizure-free (Engel IA after two years of follow-up). This example illustrates the possible use of a non-invasive approach with multimodal imaging to confirm a suspected epileptogenic zone.
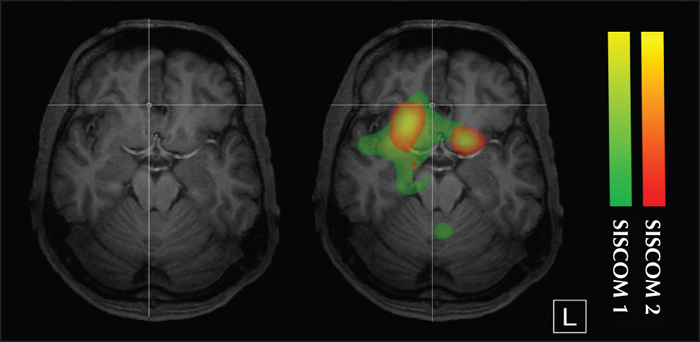
Figure 3
SISCOM in mesial frontal lobe epilepsy due to a tumour. This patient was a 45-year-old man who developed epilepsy at the age of 25 years. MRI showed a lesion with calcifications in the right mesial frontal lobe (white cross), consistent with a low-grade tumour. He was referred for ictal SPECT because both right and left temporal lobe seizures were documented during long-term video-EEG recordings. Two ictal SPECTs were obtained. SISCOM 1 (green yellow), thresholded at z=+1.5, showed a hyperperfusion cluster with the highest z-score near the lesion, but not overlapping it, and propagation towards the right and left temporal lobes. SISCOM 2 (red-yellow) showed two separate hyperperfusion clusters, with the highest z-score on the right. Using SISCOM, it was possible to resolve non-invasively an apparent discordancy between an epileptic lesion in the mesial frontal lobe and electroclinical data which suggested temporal lobe seizures, i.e. pseudotemporal lobe epilepsy.
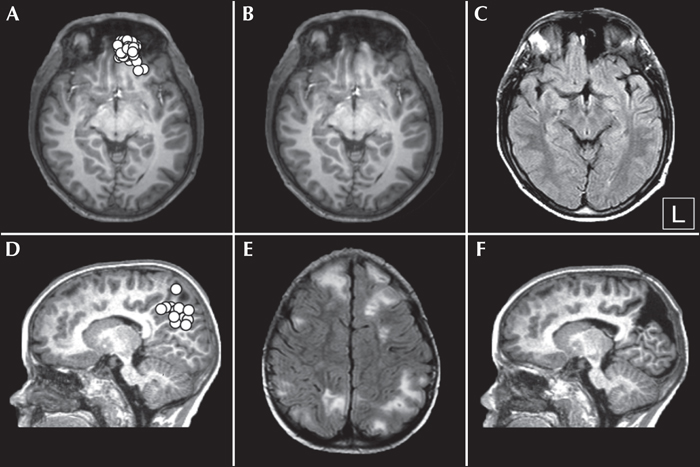
Figure 4
MEG in mesial ETLE. (A) MEG results from an 18-year-old man with refractory frontal lobe epilepsy (several seizures per night), with non-localizing interictal and ictal EEG at the sublobar level, MRI considered as negative, and non-contributory FDG-PET. MEG showed a focal cluster of epileptic sources at the level of the left gyrus rectus. (B) MEG-based reanalysis of MRI data revealed a subtle focal cortical dysplasia (FCD) at the level of the MEG cluster. The location of the seizure onset zone at the level of the FCD was confirmed by MEG-guided SEEG. (C) Post-operative MRI showing the resection cavity of the FCD type IIa. Outcome was Engel IA during the first 18 months post-surgery and Engel 1B (rare non-disabling seizures) for the next four years. (D) MEG results for a 4-year-old boy with tuberous sclerosis and refractory focal epilepsy (daily seizures) showing a focal cluster of epileptic sources at the level of a right mesial parietal tuber. (E) Flair MRI showing the multiple cortical tubers. (F) Post-operative MRI showing the resection cavity of the right mesial parietal tuber. Outcome was Engel IA with more than three years of follow-up. In this case, it was possible to differentiate between different possible epileptogenic lesions and determine the operative strategy non-invasively using MEG.
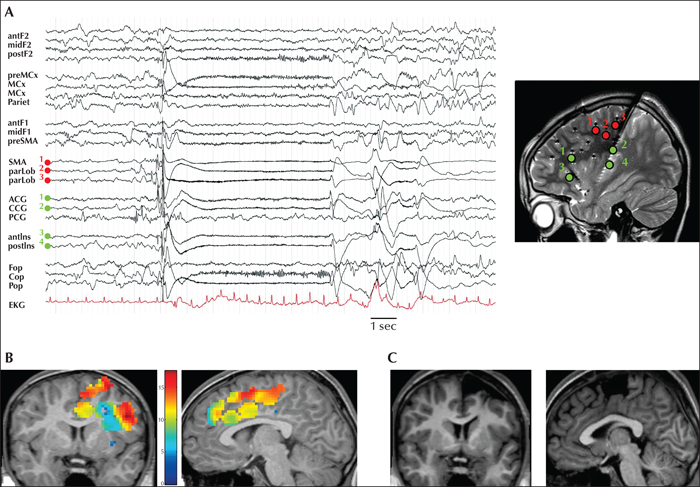
Figure 5
SEEG in SMA epilepsy. A right-handed, 12-year-old girl with no significant medical history developed epilepsy at the age of 5. Her seizures were characterized by a relatively brief right tonic posturing involving both upper and lower limbs, without loss of consciousness or speech impairment. Sudden tingling of the right leg could precede seizures. The interictal video-EEG pointed towards the left central region, as well as parietocentral and temporal areas. The first ictal EEG changes were apparent in the left precentral and frontopolar region. PET imaging revealed focal hypometabolism around the left superior frontal sulcus. (A) Since MRI did not show any lesion, SEEG was performed to investigate the left prefrontal and premotor regions, including the posterior insulo-opercular cortex. During SEEG, several typical seizures were recorded. Ictal low-voltage fast activity was more sustained on the premotor mesial cortex. SEEG implantation was performed under stereotactic conditions using a lateral orthogonal trajectory with the help of a computer-driven robotized arm for the oblique route; the left-sided electrode contacts are shown on both the MRI and the SEEG trace. Abbreviations: F1: superior frontal gyrus; F2: middle frontal gyrus; preMCx: premotor cortex; MCx: motor cortex; SMA: supplementary motor area (red contact 1); parLob: paracentral lobule (red contact 2/3); ACG: anterior cingulate gyrus (green contact 1); CCG: central cingulate gyrus (green contact 2); PCG: posterior cingulate gyrus; antins: anterior insula (green contact 3); postins: posterior insula (green contact 4); Fop: frontal operculum; Pop: parietal operculum; Cop: central operculum. (B) SEEG findings were further confirmed by the quantification of ictal high-frequency oscillations between 60 and 100 Hz. Epileptogenicity maps demonstrated the involvement of a larger network. The most significant activation was, however, found in the premotor mesial cortex, in line with the electroclinical findings. (C) Postoperative MRI illustrating the resection of the mesial premotor cortex. A frontomesial resection resulted in good functional and seizure outcome (Engel IB after four years of follow-up). Histopathology revealed FCD type IIa.
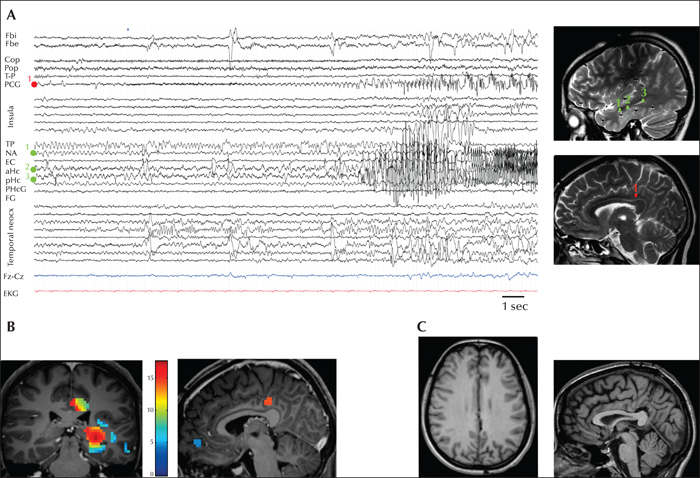
Figure 6
SEEG in posterior cingulate epilepsy. A 14-year-old, left-handed girl with drug-resistant epilepsy experienced epigastric sensations associated with a gustatory illusion, sometimes followed by a loss of consciousness and oro-alimentary automatisms. Speech was preserved during seizures. A focal lesion in the left thalamus, supposedly the result of a perinatal vascular event, was visible on MRI. FDG-PET showed clear left temporal hypometabolism. Interictal spikes were preferentially observed in the left temporal region. The typical ictal pattern involved rhythmic theta activity that was more posteriorly located, involving posterior temporal and centro-parietal regions. (A) Because of atypical findings on scalp EEG, and with no obvious lesion on MRI, an implantation with SEEG electrodes was proposed for this patient. An SEEG study was performed to investigate the left temporal and basal temporal regions, as well as the parietal and insulo-opercular cortex. During the seizure, SEEG revealed a low-voltage fast activity involving the parietal cingulate gyrus, which preceded the mesio-temporal discharge. SEEG implantation was performed; left-sided electrode contacts are shown on MRI and on the SEEG trace. Epileptic activity starts on the PCG (posterior cingulate gyrus) contact (red contact 1) and propagates to mesial temporal structures (NA: amygdala [green contact 1]; aHc: anterior hippocampus [green contact 2]; pHc: posterior hippocampus [green contact 3]). (B) The seizure onset zone was confirmed by epileptogenicity mapping, illustrating an important network involvement with rapid propagation to the mesial temporal region. (C) A very restricted parietal cingulate resection was performed. Neuropathology showed non-specific gliosis. The patient has been seizure-free since surgery (Engel IA with a follow-up of 33 months).

