European Cytokine Network
MENUAbsence of increased liver-related inflammatory markers in type 1 diabetes with metabolic syndrome: a nested case-control study from Brazil Volume 31, issue 4, December 2020
- Key words: fatty liver, IL-6, IL-17, tumor necrosis factor-α, C-reactive protein, metabolic syndrome, type 1 diabetes
- DOI : 10.1684/ecn.2020.0459
- Page(s) : 147-53
- Published in: 2020
Aims
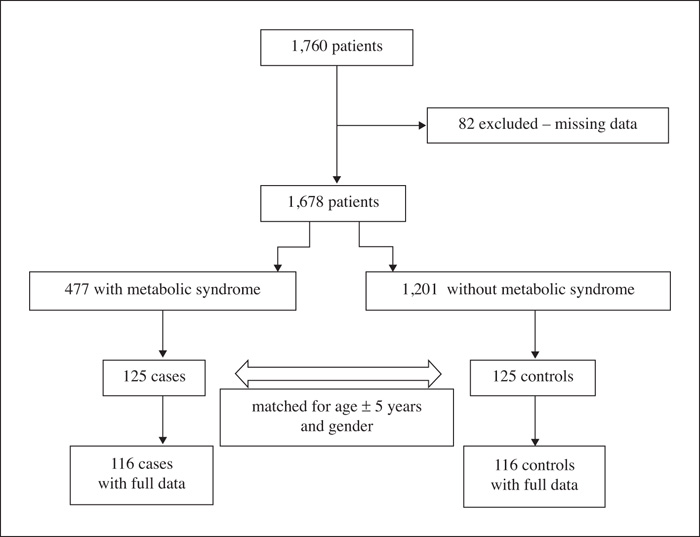
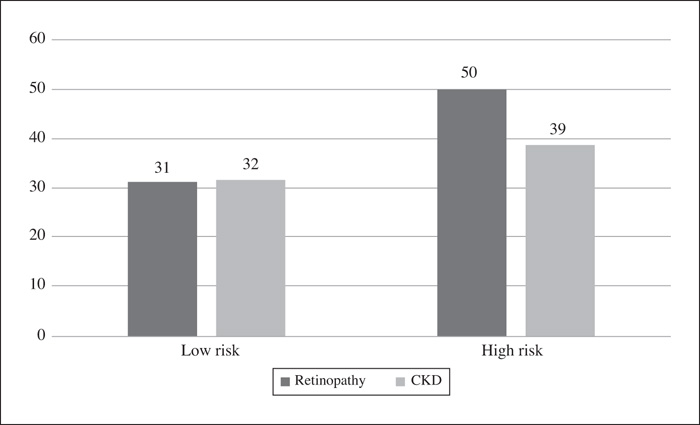
To examine the relationship between metabolic syndrome and serum levels of interleukin (IL)-6 and IL-17, tumor necrosis factor-α (TNF-α), and C-reactive protein (CRP), inflammatory biomarkers involved in nonalcoholic fatty liver disease (NAFLD) pathophysiology, in patients with type 1 diabetes. Methods: This was a cross-sectional, nested case-control study with 232 patients with type 1 diabetes (116 cases with metabolic syndrome and 116 controls without metabolic syndrome) who were matched for age and gender. A multivariable logistic regression with metabolic syndrome as the dependent variable was performed with inflammatory biomarkers and other parameters involved in NAFLD as independent variables. Results: Chronic kidney disease (CKD), retinopathy, body mass index (BMI), diabetes duration, alanine aminotransferase (ALT), fatty liver index (FLI), and CPR levels were associated with metabolic syndrome in univariate analysis. However, after adjustments in multivariable analysis, none of the liver-related inflammatory biomarkers persisted associated with metabolic syndrome. CKD, BMI, and ALT were associated with metabolic syndrome and retinopathy showed a tendency for association (p = 0.06). Conclusion: Although CRP, a nonspecific marker of inflammation, was associated with metabolic syndrome in univariate analysis, this fact did not persist after adjustments. No other inflammatory biomarkers showed an association with metabolic syndrome in type 1 diabetes. The group with metabolic syndrome had a higher frequency of diabetes’ complications and markedly increased FLI. FLI probably is more useful in detecting NAFLD than inflammatory biomarkers, but further prospective studies in individuals with type 1 diabetes, with abdominal ultrasound and FLI, are necessary to better support this hypothesis.