Epileptic Disorders
MENUIntracranial investigation of a patient with nodular heterotopia and hippocampal sclerosis: dealing with a dual pathology Volume 19, numéro 2, June 2017
Auteurs
1 Epilepsy Program, Section of Neurology, Hospital Pablo Tobón Uribe, University of Antioquia, Medellín, Colombia
2 Saskatchewan Epilepsy Program, Division of Neurology, Department of Medicine, Royal University Hospital, University of Saskatchewan, Saskatoon, Saskatchewan
3 Clinical Neurophysiology Laboratory, Royal University Hospital, The Canadian Association of Electroneurophysiology Technologists (CAET), Saskatoon, Saskatchewan
4 Division of Neurosurgery, Department of Surgery, Royal University Hospital, University of Saskatchewan, Saskatoon, Saskatchewan, Canada
* Correspondence: José F. Téllez-Zenteno
Department of Medicine,
Division of Neurology Royal University Hospital,
Saskatoon, SK,
S7N 0W8 Canada
- Mots-clés : epilepsy surgery, dual pathology, periventricular nodular heterotopia, posterior-quadrant epilepsy, temporal lobectomy
- DOI : 10.1684/epd.2017.0912
- Page(s) : 195-201
- Année de parution : 2017
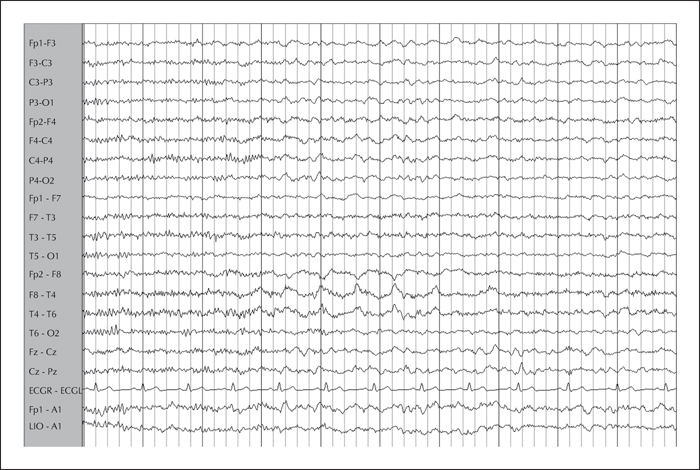
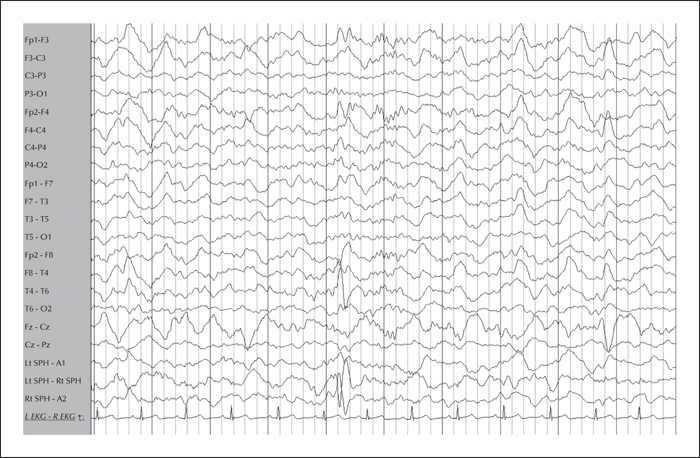
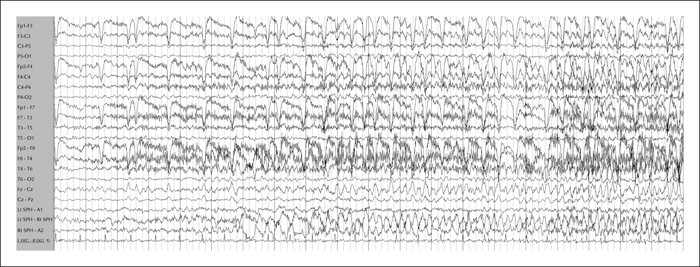
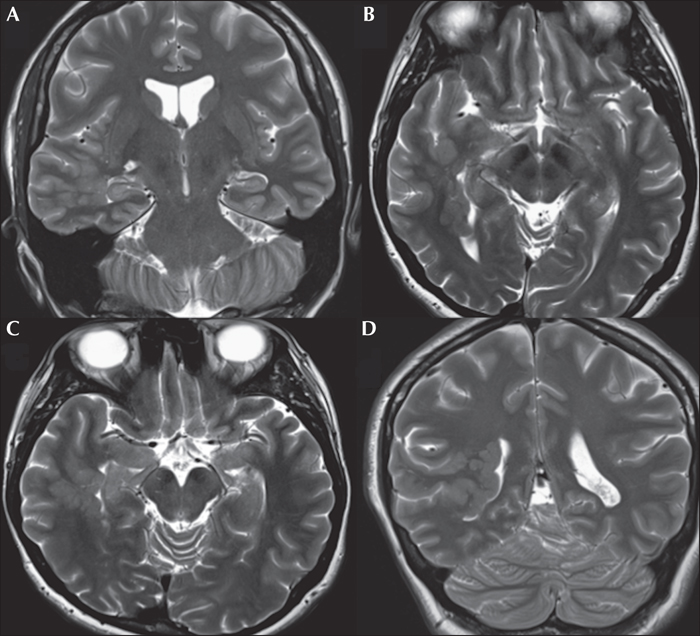
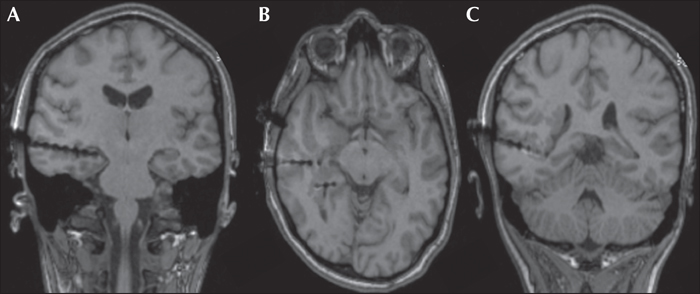
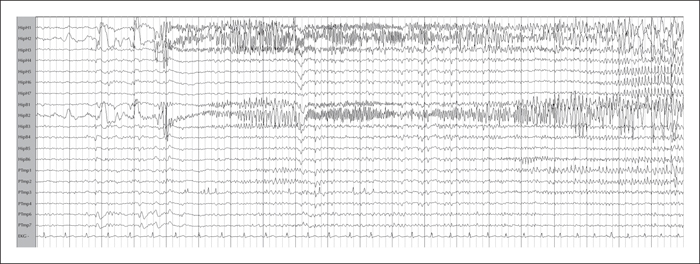
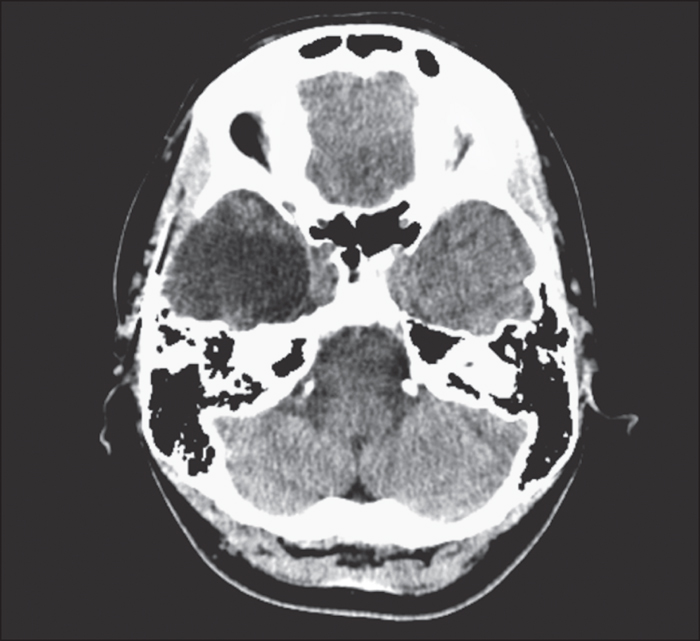
The pre-operative assessment and surgical management of patients with dual pathology is challenging. We describe a patient with drug-resistant focal epilepsy with hippocampal sclerosis and extensive periventricular nodular heterotopia in the same hemisphere. The semiology, scalp EEG, and imaging were divergent, but the presence of focal interictal and ictal epileptic discharges of the putative ictal onset zone resulted in successful localization of the epileptogenic zone. A less aggressive resection was performed based on intracranial EEG recording. The patient has been seizure-free for three years since resection. Electroclinical hypotheses and challenges in defining the epileptogenic network are discussed.