Hépato-Gastro & Oncologie Digestive
MENUDefinition, concepts, scores and classification of Acute-on-Chronic Liver Failure (ACLF): a practical review Volume 24, supplement 3, Novembre 2017
- Key words: Acute-on-Chronic Liver Failure (ACLF), organ failure, liver transplantation, withdrawal of care
- DOI : 10.1684/hpg.2017.1511
- Page(s) : 64-71
- Published in: 2017
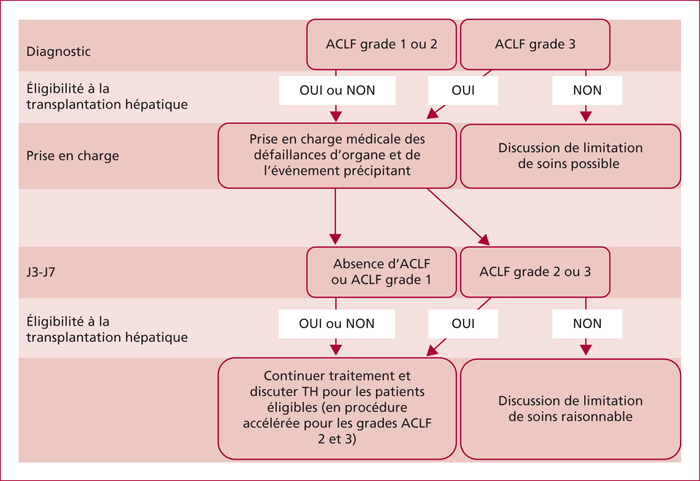
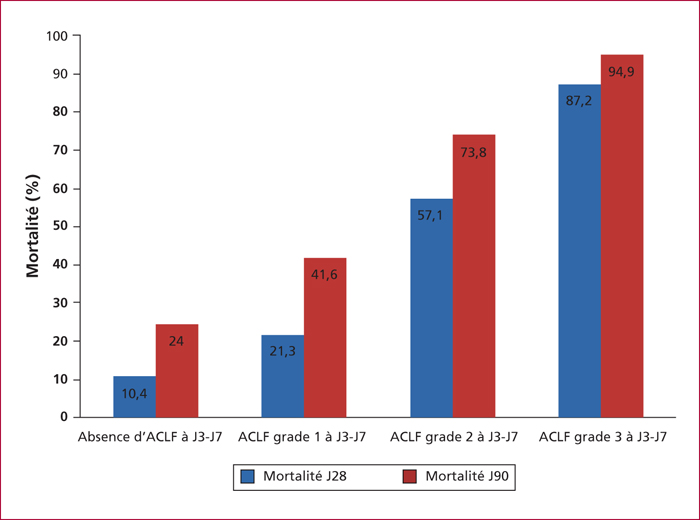
Acute-on-Chronic Liver Failure (ACLF) has been recently defined as a highly prevalent syndrome consisting of acute decompensation associated with organ failure(s) and high short-term mortality. Specific features of this syndrome have been described: presence of systemic inflammatory syndrome which is non-systematically associated with an infectious event, a rapid clinical course of the syndrome in the first days after admission and the concept of non-mandatory precipitating event. Since the CANONIC (Chronic Liver Failure (CLIF) Consortium ACLF In Cirrhosis) study, ACLF has been graduated (3 grades) according to the number of organ failure(s) and the associated risk of 28-day mortality (ranging from 22,1% to 76,7%). The CLIF-C OF (CLIF-Consortium Organ Failure) defines the grade of ACLF depending on the number of failure(s). CLIF-C ACLF (CLIF-Consortium ACLF) has been developed in order to improve the performance in mortality prediction of available scores. When combining CLIF-C OF, leucocytes count and age, the CLIF-C ACLF obtain the greatest performance in prediction of mortality. These scores when calculated sequentially at admission and after day 3 to 7 of medical management are useful for: 1) improvement in outcome prediction, 2) identification of patients to address to liver transplantation, 3) identification of patients that are the more susceptible to benefit from new medical treatments in order to avoid liver transplantation thanks to the reversibility of the decompensation.