European Journal of Dermatology
MENUMuir-Torre syndrome caused by exonic deletion of MLH1 due to homologous recombination Volume 27, issue 1, January-February 2017
- Key words: hereditary nonpolyposis colorectal cancer, Lynch syndrome, MSH2, sebaceous adenoma, sebaceous carcinoma, squamous cell carcinoma
- DOI : 10.1684/ejd.2016.2916
- Page(s) : 54-8
- Published in: 2017
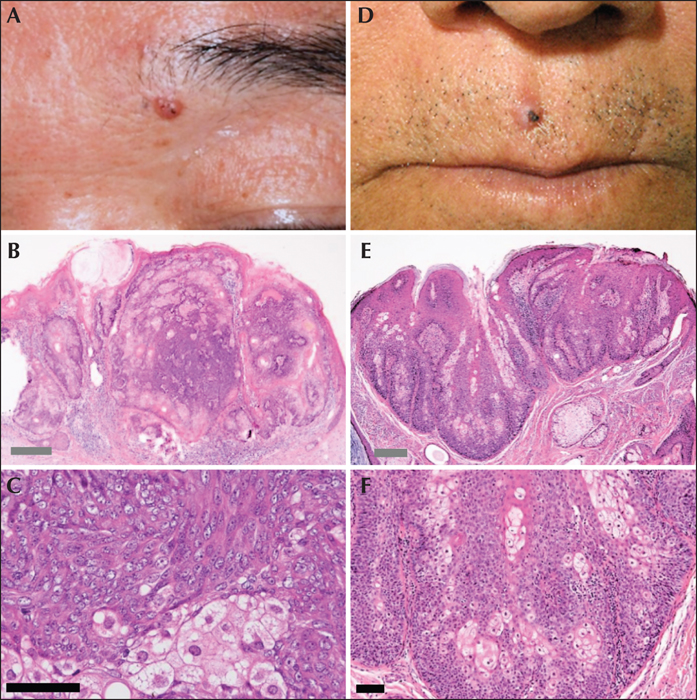
Background: Muir-Torre syndrome (MTS) is characterized by sebaceous neoplasms with internal malignancies and regarded as a variant of hereditary nonpolyposis colorectal cancer (HNPCC). Pathogenic variations of MTS have been identified in the MSH2, MLH1, and MSH6 genes, with the majority of variations located in MSH2. Objectives: To present an MTS patient who was the only individual with skin malignancies within a cancer-prone pedigree and to show the usefulness of RNA-based genetic analysis in the investigation of MTS. Materials & methods: A 77-year-old man who had operated X-ray equipment at his workplace in his twenties was clinically diagnosed with MTS and investigated by RNA-based analysis, multiplex ligation-dependent probe amplification, and genomic DNA sequencing. Results: The patient had suffered from sebaceous tumours, squamous cell carcinomas of the skin, and colon cancer. The patient's family history was remarkable for visceral malignant diseases. Genetic analysis revealed homologous recombination between two Alu elements within intron 4 and 5 of the MLH1 gene. The rearrangement caused a 1,222-bp deletion, including the entire exon 5. Deletion of exon 5 has previously been reported only in two patients with HNPCC, and not in patients with MTS. Conclusion: For the genetic analysis of MTS, the possibility of rare copy number variations of MLH1, as well as MSH2 variations, should be considered. RNA-based screening using puromycin is recommended in order to identify such variations. It remains unclear why only the proband among the pedigree had skin malignancies, however, the skin carcinogenesis might have been related to occupational radiation exposure.